The Impact of Medical Nutrition Intervention on the Management of Hyperphosphatemia in Hemodialysis Patients with Stage 5 Chronic Kidney Disease: A Case Series
- PMID: 36981958
- PMCID: PMC10049720
- DOI: 10.3390/ijerph20065049
The Impact of Medical Nutrition Intervention on the Management of Hyperphosphatemia in Hemodialysis Patients with Stage 5 Chronic Kidney Disease: A Case Series
Abstract
The treatment and interdisciplinary management of patients with chronic kidney disease (CKD) continue to improve long-term outcomes. The medical nutrition intervention's role is to establish a healthy diet plan for kidney protection, reach blood pressure and blood glucose goals, and prevent or delay health problems caused by kidney disease. Our study aims to report the effects of medical nutrition therapy-substituting foods rich in phosphorus-containing additives with ones low in phosphates content on phosphatemia and phosphate binders drug prescription in stage 5 CKD patients with hemodialysis. Thus, 18 adults with high phosphatemia levels (over 5.5 mg/dL) were monitored at a single center. Everyone received standard personalized diets to replace processed foods with phosphorus additives according to their comorbidities and treatment with prosphate binder drugs. Clinical laboratory data, including dialysis protocol, calcemia, and phosphatemia, were evaluated at the beginning of the study, after 30 and 60 days. A food survey was assessed at baseline and after 60 days. The results did not show significant differences between serum phosphate levels between the first and second measurements; thus, the phosphate binders' initial doses did not change. After 2 months, phosphate levels decreased considerably (from 7.322 mg/dL to 5.368 mg/dL); therefore, phosphate binder doses were diminished. In conclusion, medical nutrition intervention in patients with hemodialysis significantly reduced serum phosphate concentrations after 60 days. Restricting the intake of processed foods containing phosphorus additives-in particularized diets adapted to each patient's comorbidities-and receiving phosphate binders represented substantial steps to decrease phosphatemia levels. The best results were significantly associated with life expectancy; at the same time, they showed a negative correlation with the dialysis period and participants' age.
Keywords: chronic kidney disease; compliance; hemodialysis; medical nutrition therapy; phosphate binder drugs; phosphatemia.
Conflict of interest statement
The authors declare no conflict of interest.
Figures
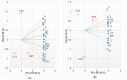
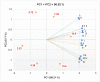
References
-
- World Health Organisation, Chronic Kidney Disease. [(accessed on 1 February 2023)]. Available online: https://www.paho.org/en/topics/chronic-kidney-disease.
-
- Levey A.S., Eckardt K.U., Dorman N.M., Christiansen S.L., Hoorn E.J., Ingelfinger J.R., Inker L.A., Levin A., Mehrotra R., Palevsky P.M., et al. Nomenclature for kidney function and disease: Report of a Kidney Disease: Improving Global Outcomes (KDIGO) Consensus Conference. Kidney Int. 2020;97:1117–1129. doi: 10.1016/j.kint.2020.02.010. - DOI - PubMed
-
- National Institute of Diabetes and Digestive and Kidney Diseases. [(accessed on 1 February 2023)]; Available online: https://www.niddk.nih.gov/health-information/kidney-disease/chronic-kidn....
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical

