Parameter D: New Measure of Airflow Obstruction
- PMID: 36989246
- PMCID: PMC10718182
- DOI: 10.1513/AnnalsATS.202209-816OC
Parameter D: New Measure of Airflow Obstruction
Abstract
Rationale: Currently used spirometry measures of airflow obstruction are influenced by demographics, predominantly by age, complicating selection of diagnostic thresholds for the presence of airflow obstruction. Objectives: To develop diagnostic thresholds for Parameter D, a new metric for detection of airflow obstruction, which quantifies the rate of rise of expiratory volume over time. Methods: We analyzed spirometry data of normal subjects enrolled in the 2007-2008, 2009-2010, and 2011-2012 NHANES (National Health and Nutrition Examination Survey) cohorts and calculated Parameter D using the expiratory volume-time curve. Relationships between demographics and lung function (forced expiratory volume in 1 second [FEV1], FEV1/forced vital capacity [FVC], and Parameter D) were tested using generalized linear models in NHANES and UK Biobank. The variation in lung function explained by demographics was estimated using R2. A diagnostic threshold was developed for Parameter D using population-based percentiles. Based on concordance between the lower limit of normal (LLN) for FEV1/FVC and the Parameter D threshold, four groups were identified: normal (no airflow obstruction by either criterion), D+chronic obstructive pulmonary disease (D+COPD; positive by Parameter D only), D-COPD (positive by LLN only), and COPD (positive by both criteria), and associations with structural lung disease, exacerbations, and mortality were tested using multivariable analyses. Results: In contrast to FEV1 and FEV1/FVC, demographics cumulatively explained only 9% of the variance in Parameter D in NHANES (n = 4,945) and 3% in UK BioBank (n = 109,623). In COPDGene (Genetic Epidemiology of Chronic Obstructive Pulmonary Disease) (n = 9,542), a diagnostic threshold of -3.15 resulted in the identification of an additional 10.8% of participants with airflow obstruction. A total of 3.7% had FEV1/FVC < LLN but were missed by the Parameter D threshold. Compared with subjects in the normal group, after adjustment for age, sex, race, body mass index, pack-years of smoking, and current smoking status, D+COPD was associated with worse structural lung disease (odds ratio [OR] for ⩾5% emphysema, 1.71; 95% confidence interval [CI], 1.37-2.12; OR for functional small airway disease ⩾ 15%, 2.1; 95% CI, 1.79-2.67) and significant symptoms (OR for modified Medical Research Council dyspnea score ⩾ 2, 1.25; 95% CI, 1.07-1.47; OR for St. George's respiratory questionnaire ⩾ 25, 1.31; 95% CI, 1.13-1.53), a greater frequency of exacerbations (incidence rate ratio, 1.26; 95% CI, 1.10-1.46), and higher mortality (hazard ratio, 1.32; 95% CI, 1.10-1.57). Over 5 years, 28% of the D+COPD group versus 8% of normal group progressed to COPD by traditional criteria. Conclusions: Parameter D is not affected by age, and a normal population-based diagnostic threshold results in the early identification of additional individuals with airflow obstruction with a substantial amount of structural lung disease and respiratory symptoms.
Keywords: Parameter D; airflow obstruction; chronic obstructive pulmonary disease; spirometry.
Figures
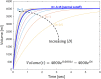


Comment in
-
D for Destiny? Parameter D and Chronic Obstructive Pulmonary Disease.Ann Am Thorac Soc. 2023 Jul;20(7):953-954. doi: 10.1513/AnnalsATS.202304-373ED. Ann Am Thorac Soc. 2023. PMID: 37387627 No abstract available.
References
-
- Vogelmeier CF, Criner GJ, Martinez FJ, Anzueto A, Barnes PJ, Bourbeau J, et al. Global Strategy for the Diagnosis, Management, and Prevention of Chronic Obstructive Lung Disease 2017 report: GOLD executive summary. Am J Respir Crit Care Med . 2017;195:557–582. - PubMed
-
- Hankinson JL, Odencrantz JR, Fedan KB. Spirometric reference values from a sample of the general U.S. population. Am J Respir Crit Care Med . 1999;159:179–187. - PubMed

