Tumor deposits in colorectal cancer: Refining their definition in the TNM system
- PMID: 36998291
- PMCID: PMC10043773
- DOI: 10.1002/ags3.12652
Tumor deposits in colorectal cancer: Refining their definition in the TNM system
Abstract
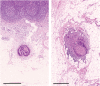
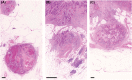
Tumor deposits (TDs) are discontinuous tumor spread in the mesocolon/mesorectum which is found in approximately 20% of colorectal cancer (CRC) and negatively affects survival. We have a history of repeated revisions on TD definition and categorization in the tumor-node-metastasis (TNM) system leading to stage migration. Since 1997, TDs have been categorized as T or N factors depending on their size (TNM5) or contour (TNM6). In 2009, TNM7 provided the category of N1c for TDs in a case without positive lymph nodes (LNs), which is also used in TNM8. However, increasing evidence suggests that these revisions are suboptimal and only "partially" successful. Specifically, the N1c rule is certainly useful for oncologists who are having difficulty with TDs in a case with no positive LNs. However, it has failed to maximize the value of the TNM system because of the underused prognostic information of individual TDs. Recently, the potential value of an alternative staging method has been highlighted in several studies using the "counting method." For this method, all nodular type TDs are individually counted together with positive LNs to derive the final pN, yielding a prognostic and diagnostic value that is superior to existing TNM systems. The TNM system has long stuck to the origin of TDs in providing its categorization, but it is time to make way for alternative options and initiate an international discussion on optimal treatment of TDs in tumor staging; otherwise, a proportion of patients end up missing an opportunity to receive the optimal adjuvant treatment.
Keywords: Extramural cancer deposits without lymph node structure (EX); Lymph node metastasis; Tumor deposits (TDs); Tumor‐node‐metastasis (TNM) system; tumor stage.
© 2023 The Authors. Annals of Gastroenterological Surgery published by John Wiley & Sons Australia, Ltd on behalf of The Japanese Society of Gastroenterological Surgery.
Conflict of interest statement
Hideki Ueno is a current Associate Editor of the Annals of Gastroenterological Surgery.
Figures



References
-
- Sobin LH, Wittekind C. UICC TNM classification of malignant tumours. 5th ed. New York, NY: John Wiley & Sons; 1997.
Publication types
LinkOut - more resources
Full Text Sources

