Short sleep duration associated with the incidence of cardio-cerebral vascular disease: a prospective cohort study in Shanghai, China
- PMID: 37003977
- PMCID: PMC10067235
- DOI: 10.1186/s12872-023-03205-y
Short sleep duration associated with the incidence of cardio-cerebral vascular disease: a prospective cohort study in Shanghai, China
Abstract
Importance: Sleep duration plays an important role in predicting CCVD incidence, and have implications for reducing the burden of CCVD. However, the association between sleep duration and predicted cardio-cerebral vascular diseases (CCVD) risk remains to be fully understood.
Objective: To investigate the effects of sleep duration on the development of CCVD among Chinese community residents.
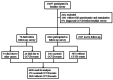
Design: A prospective cohort study. The baseline survey was conducted from January 2013 to July 2013. The cohort has been followed until December 31, 2016 using a combination of in-person interviews and record linkages with the vital registry of Pudong New Area, Shanghai, China.
Subjects: A total of 8245 Chinese community residents were initially enrolled in the cohort. Of those, 6298 underwent the follow-up examination.
Exposure: Self-reported sleep duration and sleep quality were obtained via the questionnaire. Sleep duration was divided into five categories: ≤5, 6, 7, 8, or ≥ 9 h per day.
Main outcome(s) and measure(s): CCVD, Coronary heart disease (CHD) and Stroke occurrence, Hazard ratios (HRs) and 95% confidence intervals (95% CIs) were calculated using Fine-Gray proportional subdistribution hazards models.
Results: During a median follow-up of 3.00 years (IQR 2.92-3.08), we observed 370 participants have had incident CCVD events, of whom 230 had CHDs, 169 had strokes, and 29 had both. After adjustment for relevant confounders, short sleepers (≤ 5 h) had 83% higher risk of total CCVD incidence (HR: 1.83; 95% CI: 1.32-2.54), 82% higher risk of CHD incidence (HR: 1.82; 95% CI: 1.21-2.75), and 82% higher risk of stroke incidence (HR: 1.82; 95% CI: 1.12-2.98) in contrast to the reference group (7 h). Some of these U-shaped relationships varied by age, and were more pronounced in individuals aged < 65 years. Individuals who slept ≤ 5 h per day with baseline hypertension had the highest risk of CCVD incidence (HR: 3.38, 95% CI 2.08-5.48), CHD incidence (HR: 3.11, 95% CI 1.75-5.53), and stroke incidence (HR: 4.33, 95% CI 1.90-9.86), compared with those sleep 7 h and without baseline hypertension.
Conclusions: Short sleep duration is independently associated with greater incidence of CCVD, CHD and stroke.
Question What exactly is the relationship between sleep duration and CCVD occurrence in Chinese community residents?
Keywords: Cardio-cerebral vascular disease; Coronary heart disease; Prospective cohort study; Sleep duration; Stroke.
© 2023. The Author(s).
Conflict of interest statement
The authors declare that they have no competing interests.
Figures



Similar articles
-
Sex-specific associations between extreme sleep duration and prevalence of cardio-cerebral vascular disease: a community-based cross-sectional study.Sleep Med. 2018 Feb;42:61-67. doi: 10.1016/j.sleep.2017.11.1148. Epub 2018 Jan 9. Sleep Med. 2018. PMID: 29458747
-
Association of exhaled carbon monoxide with risk of cardio-cerebral-vascular disease in the China Kadoorie Biobank cohort study.Sci Rep. 2020 Nov 11;10(1):19507. doi: 10.1038/s41598-020-76353-2. Sci Rep. 2020. PMID: 33177548 Free PMC article.
-
Changes in Sleep Patterns, Genetic Susceptibility, and Incident Cardiovascular Disease in China.JAMA Netw Open. 2024 Apr 1;7(4):e247974. doi: 10.1001/jamanetworkopen.2024.7974. JAMA Netw Open. 2024. PMID: 38652473 Free PMC article.
-
Association between sarcopenia with incident cardio-cerebrovascular disease: A systematic review and meta-analysis.Biosci Trends. 2023 Sep 15;17(4):293-301. doi: 10.5582/bst.2023.01130. Epub 2023 Aug 11. Biosci Trends. 2023. PMID: 37574268
-
Sleep duration and risk of cardio-cerebrovascular disease: A dose-response meta-analysis of cohort studies comprising 3.8 million participants.Front Cardiovasc Med. 2022 Sep 27;9:907990. doi: 10.3389/fcvm.2022.907990. eCollection 2022. Front Cardiovasc Med. 2022. PMID: 36237900 Free PMC article.
Cited by
-
Healthy Sleep Pattern, Metabolic Diseases, and Risk of Stroke: The Kailuan Cohort Study.Nat Sci Sleep. 2024 Aug 5;16:1169-1178. doi: 10.2147/NSS.S468522. eCollection 2024. Nat Sci Sleep. 2024. PMID: 39131166 Free PMC article.
-
Associations between insomnia and large vessel occlusion acute ischemic stroke: An observational study.Clinics (Sao Paulo). 2023 Nov 2;78:100297. doi: 10.1016/j.clinsp.2023.100297. eCollection 2023. Clinics (Sao Paulo). 2023. PMID: 37924679 Free PMC article.
-
Prestroke sleep and stroke: a narrative review.Sleep Breath. 2025 Jun 21;29(4):221. doi: 10.1007/s11325-025-03391-3. Sleep Breath. 2025. PMID: 40542905 Review.
-
Inadequate sleep increases stroke risk: evidence from a comprehensive meta-analysis of incidence and mortality.Geroscience. 2025 Jun;47(3):4679-4695. doi: 10.1007/s11357-025-01593-x. Epub 2025 Mar 12. Geroscience. 2025. PMID: 40072786 Free PMC article.
-
Associations between self-reported sleep duration and incident cardiovascular diseases in a nationwide prospective cohort study of Chinese middle-aged and older adults.Front Cardiovasc Med. 2024 Dec 9;11:1474426. doi: 10.3389/fcvm.2024.1474426. eCollection 2024. Front Cardiovasc Med. 2024. PMID: 39717448 Free PMC article.
References
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

