Critical care pharmacy workforce: a 2020 re-evaluation of the UK deployment and characteristics
- PMID: 37004069
- PMCID: PMC10064945
- DOI: 10.1186/s12960-023-00810-y
Critical care pharmacy workforce: a 2020 re-evaluation of the UK deployment and characteristics
Abstract
Introduction: Critical care pharmacists improve the quality and efficiency of medication therapy whilst reducing treatment costs where they are available. UK critical care pharmacist deployment was described in 2015, highlighting a deficit in numbers, experience level, and critical care access to pharmacy services over the 7-day week. Since then, national workforce standards have been emphasised, quality indicators published, and service commissioning documents produced, reinforced by care quality assessments. Whether these initiatives have resulted in further development of the UK critical care pharmacy workforce is unknown. This evaluation provides a 2020 status update.
Methods: The 2015 electronic data entry tool was updated and circulated for completion by UK critical care pharmacists. The tool captured workforce data disposition as it was just prior to the COVID-19 pandemic, at critical care unit level.
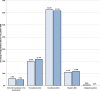
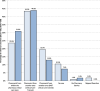
Main findings: Data were received for 334 critical care units from 203 organisations (96% of UK critical care units). Overall, 98.2% of UK critical care units had specific clinical pharmacist time dedicated to the unit. The median weekday pharmacist input to each level 3 equivalent bed was 0.066 (0.043-0.088) whole time equivalents, a significant increase from the median position in 2015 (+ 0.021, p < 0.0001). Despite this progress, pharmacist availability remains below national minimum standards (0.1/level 3 equivalent bed). Most units (71.9%) had access to prescribing pharmacists. Geographical variation in pharmacist staffing levels were evident, and weekend services remain extremely limited.
Conclusions: Availability of clinical pharmacists in UK adult critical care units is improving. However, national standards are not routinely met despite widely publicised quality indicators, commissioning specifications, and assessments. Additional measures are needed to address persistent deficits and realise gains in organisational and patient-level outcomes. These measures must include promotion of cross-professional collaborative working, adjusted funding models, and a nationally recognised training pathway for critical care pharmacists.
Keywords: Census; Distribution; Hospital; Intensive care; Organisation; Pharmacy; Planning.
© 2023. Crown.
Conflict of interest statement
The authors declare they have no competing interests.
Figures


References
-
- National Institute for Health and Care Excellence. Medicines optimisation: the safe and effective use of medicines to enable the best possible outcomes. NICE guideline. 2015. https://www.nice.org.uk/guidance/ng5/chapter/1-recommendations. [Accessed 07/09/2022]. - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

