Phenotype tailored lifestyle intervention on weight loss and cardiometabolic risk factors in adults with obesity: a single-centre, non-randomised, proof-of-concept study
- PMID: 37007741
- PMCID: PMC10050763
- DOI: 10.1016/j.eclinm.2023.101923
Phenotype tailored lifestyle intervention on weight loss and cardiometabolic risk factors in adults with obesity: a single-centre, non-randomised, proof-of-concept study
Abstract
Background: Lifestyle interventions for weight loss are currently not individualised to underlying pathophysiology and behavioral traits in obesity. We aim to compare the outcome of a standard lifestyle intervention (SLI) to phenotype-tailored lifestyle interventions (PLI) on weight loss, cardiometabolic risk factors and physiologic variables contributing to obesity.
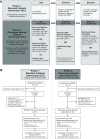
Methods: This 12-week, single-centre non-randomised proof-of-concept clinical trial including men and women aged 18-65 years with a body mass index (BMI) greater than 30 without history of any bariatric procedure, and current use of any medication known to affect weight. Participants lived anywhere in the United States, and underwent in-person testing in Rochester, MN at a teaching hospital. All participants completed in-person phenotype testing at baseline and after 12 weeks. Participants were assigned to their intervention based on their period of enrollment. In the first phase, participants were assigned to SLI with a low-calorie diet (LCD), moderate physical activity, and weekly behavioral therapy sessions. In the second phase, other participants were assigned to PLI according to phenotype: abnormal satiation (time-restricted volumetric LCD); abnormal postprandial satiety (LCD with pre-meal protein supplementation); emotional eating (LCD with intensive behavioral therapy); and abnormal resting energy expenditure (LCD with post-workout protein supplementation and high-intensity interval training). The primary outcome was total body weight loss in kg at 12 weeks using multiple imputation for missing data. Linear models estimated the association of study group allocation and study endpoints adjusting for age, sex, and baseline weight. This study was registered with ClinicalTrials.gov, NCT04073394.
Findings: Between July 2020 and August 2021, 211 participants were screened, and 165 were assigned to one of the two treatments in the two phases: 81 SLI (mean [SD] age 42.9 [12] years; 79% women; BMI 38.0 [6.0]) and 84 PLI (age 44.8 [12.2] years; 83% women; BMI 38.7 [6.9]); 146 completed the 12-week programs. The weight loss was -7.4 kg (95%CI, -8.8, -6.0) with PLI vs. -4.3 kg (95%CI, -5.8, -2.7) with SLI (difference, -3.1 kg [95%CI, -5.1 to -1.1]; P = 0.004). No adverse events were reported in any group.
Interpretation: Phenotype-tailored lifestyle interventions may result in significant weight loss, but a randomised controlled trial is required to confirm causality.
Funding: Mayo Clinic; NIH (K23-DK114460).
Keywords: Lifestyle interventions; Obesity phenotypes; Weight loss diet.
© 2023 The Author(s).
Conflict of interest statement
AA is a stockholder in Gila Therapeutics and Phenomix Sciences; he served as a consultant for Rhythm Pharmaceuticals, General Mills, Amgen, Bausch Health, RareStone; has contracts with Vivus Inc, Satiogen Pharmaceutical, and Rhythm pharmaceutical; and has a patent submitted for biomarkers of phenotype tailored diet. MC is a stockholder in Phenomix Sciences. No other disclosure to be reported. DHD receives royalties from the book, The Mayo Clinic Diet and consulting fees from the app that includes the Mayo Clinic Diet. All other authors declare no competing interests.
Figures

References
-
- Heymsfield S.B., Wadden T.A. Mechanisms, pathophysiology, and management of obesity. N Engl J Med. 2017;376(3):254–266. - PubMed
-
- LeBlanc E.L., Patnode C.D., Webber E.M., Redmond N., Rushkin M., O'Connor E.A. Behavioral and pharmacotherapy weight loss interventions to prevent obesity-related morbidity and mortality in adults: an updated systematic review for the US preventive services task force. Agency for Healthcare Research and Quality (US); Rockville, MD: 2018. U.S. Preventive services task force evidence syntheses, formerly systematic evidence reviews. - PubMed
-
- Acosta A., Streett S., Kroh M.D., et al. White paper AGA: POWER - practice guide on obesity and weight management, education, and resources. Clin Gastroenterol Hepatol. 2017;15(5):631–649.e10. - PubMed
Associated data
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

