Shared decision-making for children with medical complexity in community health services: a scoping review
- PMID: 37012004
- PMCID: PMC10083859
- DOI: 10.1136/bmjpo-2023-001866
Shared decision-making for children with medical complexity in community health services: a scoping review
Abstract
Background: Children with medical complexity is an increasing population whose parents and healthcare providers face multiple decisions. Shared decision-making is a process where patients, their families and healthcare providers collaborate to make decisions based on clinical evidence and informed preferences of the family. Shared decision-making has benefits for the child, family and healthcare providers, including improved parental understanding of the child's difficulties, increased participation, improved coping skills and more efficient healthcare use. It is, however, poorly implemented.
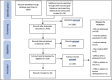
Aims and methods: A scoping review was conducted to explore shared decision-making for children with medical complexity in community health services, including how shared decision-making is defined in research, how it is implemented, including barriers and facilitators and recommendations for research. Six databases were systematically searched for papers published in English up to May 2022: Medline, CINAHL, EMBASE, PsycINFO, PubMed, Cochrane Database of Systematic Reviews and sources of grey literature. The review is reported according to the Preferred Reporting Items for Scoping Reviews.
Results: Thirty sources met the inclusion criteria. Most factors can either be a facilitator or barrier to shared decision-making depending on the context. Two significant barriers to shared decision-making in this population include uncertainty about the child's diagnosis, prognosis, and treatment options and the presence of hierarchy and power imbalance during clinical encounters with healthcare providers. Further influencing factors include continuity of care, the availability of accurate, accessible, adequate, and balanced information and the interpersonal and communication skills of parents and healthcare providers.
Conclusion: Uncertainty about diagnosis, prognosis and treatment outcomes for children with medical complexity are additional challenges to the known barriers and facilitators to shared decision-making in community health services. Effective implementation of shared decision-making requires advancement of the evidence base for children with medical complexity, reducing power imbalance in clinical encounters, improving continuity of care, and improving the availability and accessibility of information resources.
Keywords: Health services research.
© Author(s) (or their employer(s)) 2023. Re-use permitted under CC BY. Published by BMJ.
Conflict of interest statement
Competing interests: No, there are no competing interests.
Figures
References
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Miscellaneous