Seroepidemiology of Leptospira serovar Hardjo and associated risk factors in smallholder dairy cattle in Tanzania
- PMID: 37018175
- PMCID: PMC10075398
- DOI: 10.1371/journal.pntd.0011199
Seroepidemiology of Leptospira serovar Hardjo and associated risk factors in smallholder dairy cattle in Tanzania
Abstract
Background: Smallholder dairy farming is crucial for the Tanzanian dairy sector which generates income and employment for thousands of families. This is more evident in the northern and southern highland zones where dairy cattle and milk production are core economic activities. Here we estimated the seroprevalence of Leptospira serovar Hardjo and quantified potential risk factors associated with its exposure in smallholder dairy cattle in Tanzania.
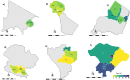
Methods: From July 2019 to October 2020, a cross-sectional survey was carried out in a subset of 2071 smallholder dairy cattle. Information about animal husbandry and health management was collected from farmers, and blood was taken from this subset of cattle. Seroprevalence was estimated and mapped to visualize potential spatial hotspots. The association between a set of animal husbandry, health management and climate variables and ELISA binary results was explored using a mixed effects logistic regression model.
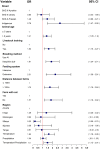
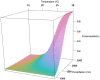
Results: An overall seroprevalence of 13.0% (95% CI 11.6-14.5%) for Leptospira serovar Hardjo was found in the study animals. There was marked regional variations with the highest seroprevalence in Iringa 30.2% (95% CI 25.1-35.7%) and Tanga 18.9% (95% CI 15.7-22.6) with odds ratios of OR = 8.13 (95% CI 4.23-15.63) and OR = 4.39 (95% CI 2.31-8.37), respectively. Multivariate analysis revealed the individual animal factors that were a significant risk for Leptospira seropositivity in smallholder dairy cattle were: animals over 5 years of age (OR = 1.41, 95% CI 1.05-1.9); and indigenous breed (OR = 2.78, 95% CI 1.47-5.26) compared to crossbred animals SHZ-X-Friesian (OR = 1.48, 95% CI 0.99-2.21) and SHZ-X-Jersey (OR = 0.85, 95% CI 0.43-1.63). Farm management factors significantly associated with Leptospira seropositivity included: hiring or keeping a bull for raising purposes (OR = 1.91, 95% CI 1.34-2.71); distance between farms of more than 100 meters (OR = 1.75, 95% CI 1.16-2.64); cattle kept extensively (OR = 2.31, 95% CI 1.36-3.91); farms without cat for rodent control (OR = 1.87, 95% CI 1.16-3.02); farmers with livestock training (OR = 1.62, 95% CI 1.15-2.27). Temperature (OR = 1.63, 95% CI 1.18-2.26), and the interaction of higher temperature and precipitation (OR = 1.5, 95%CI 1.12-2.01) were also significant risk factors.
Conclusion: This study indicated seroprevalence of Leptospira serovar Hardjo, as well as the risk factors driving dairy cattle leptospirosis exposure in Tanzania. The study showed an overall high leptospirosis seroprevalence with regional variations, where Iringa and Tanga represented the highest seroprevalence and risk. The study highlighted the urgent need to understand the human exposures and risks from this important zoonosis to develop control measures and awareness of the problem and quantify the economic and production impacts through abortion and milk loss. In addition, given that the available data was limited to Leptospira serovar Hardjo, the study recommends more studies to identify serologically the most common serovars in cattle for targeted vaccination and risk reduction.
Copyright: © 2023 Motto et al. This is an open access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Conflict of interest statement
The authors have declared that no competing interests exist.
Figures

Similar articles
-
Herd and animal level seroprevalence and associated risk factors of Leptospira interrogans sensu lato serovar Hardjo in cattle in southwest Ethiopia.BMC Vet Res. 2024 Dec 6;20(1):553. doi: 10.1186/s12917-024-04418-9. BMC Vet Res. 2024. PMID: 39639266 Free PMC article.
-
Seroprevalence and herd-level risk factors for seroprevalence of Leptospira spp. in sheep, beef cattle and deer in New Zealand.N Z Vet J. 2018 Nov;66(6):302-311. doi: 10.1080/00480169.2018.1507770. Epub 2018 Sep 16. N Z Vet J. 2018. PMID: 30122123
-
Seroprevalence and risk factors associated with Leptospira Hardjo among commercial dairy cattle farms of Rupandehi district, Nepal.BMC Vet Res. 2025 Jul 5;21(1):442. doi: 10.1186/s12917-025-04882-x. BMC Vet Res. 2025. PMID: 40618117 Free PMC article.
-
A cluster of three cases of leptospirosis in dairy farm workers in New Zealand.N Z Med J. 2014 Jan 24;127(1388):13-20. N Z Med J. 2014. PMID: 24481382 Review.
-
Bovine leptospirosis: effects on reproduction and an approach to research in Colombia.Trop Anim Health Prod. 2022 Aug 9;54(5):251. doi: 10.1007/s11250-022-03235-2. Trop Anim Health Prod. 2022. PMID: 35943610 Free PMC article. Review.
Cited by
-
Detection and Determinants of Leptospira Infection in Rodents, Cattle, and Humans in Muheza District, Tanzania: A Call for One Health Approach.Public Health Chall. 2025 Mar 24;4(1):e70043. doi: 10.1002/puh2.70043. eCollection 2025 Mar. Public Health Chall. 2025. PMID: 40496120 Free PMC article.
-
Molecular and serological prevalence of Leptospira spp. among slaughtered cattle and associated risk factors in the Bahr El Ghazal region of South Sudan.BMC Vet Res. 2024 Jul 6;20(1):296. doi: 10.1186/s12917-024-04154-0. BMC Vet Res. 2024. PMID: 38971746 Free PMC article.
-
Heat Stress Effects on Physiological and Milk Yield Traits of Lactating Holstein Friesian Crossbreds Reared in Tanga Region, Tanzania.Animals (Basel). 2024 Jun 28;14(13):1914. doi: 10.3390/ani14131914. Animals (Basel). 2024. PMID: 38998026 Free PMC article.
-
Seroprevalence and associated risk factors for bovine leptospirosis in Egypt.Sci Rep. 2024 Feb 26;14(1):4645. doi: 10.1038/s41598-024-54882-4. Sci Rep. 2024. PMID: 38409338 Free PMC article.
-
Serological Survey of Leptospira spp. in Livestock and Rodents from Different Settlements in the Kilombero Wetland, Tanzania.Pathogens. 2024 Dec 1;13(12):1059. doi: 10.3390/pathogens13121059. Pathogens. 2024. PMID: 39770319 Free PMC article.
References
-
- Hartskeerl RA, Collares-Pereira M, Ellis WA, Meny P, Menéndez C, Ashfield N, et al.. (2018) Etiologies of Illness among Patients Meeting Integrated Management of Adolescent and Adult Illness District Clinician Manual Criteria for Severe Infections in Northern Tanzania: Implications for Empiric Antimicrobial Therapy. PLoS Negl Trop Dis. 9(2):1–7. 10.4269/ajtmh.14-0496 - DOI - PMC - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Miscellaneous

