Sporadic pancreatic neuroendocrine neoplasms: A retrospective clinicopathological and outcome analysis from a Latvian study group
- PMID: 37021091
- PMCID: PMC10069647
- DOI: 10.3389/fsurg.2023.1131333
Sporadic pancreatic neuroendocrine neoplasms: A retrospective clinicopathological and outcome analysis from a Latvian study group
Abstract
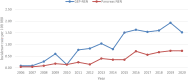
Background: Although pancreatic neuroendocrine neoplasms (PNEN) are rare, there has been a constant increase in incidence. Furthermore, PNEN present unique clinical behaviors and long-term survival can be expected even in the presence of metastases as compared with ductal adenocarcinoma of the pancreas. Determining the best therapeutic approach and proper timing of therapy requires knowledge of reliable prognostic factors. Therefore, the aim of this study was to explore clinicopathological features, treatment, and survival outcomes of patients with PNEN based on Latvian gastroenteropancreatic neuroendocrine neoplasm (GEP-NEN) registry data.
Method: Patients with confirmed PNEN at Riga East Clinical University Hospital and Pauls Stradins Clinical University Hospital, between 2008 and 2020, were retrospectively analyzed. Data were collected and included in EUROCRINE, an open-label international endocrine surgical registry.
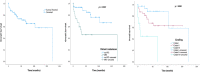
Results: In total, 105 patients were included. The median age at diagnosis was 64 years (IQR 53.0-70.0) for males and 61 years (IQR 52.5-69.0) for females. In 77.1% of patients, tumors were hormonally nonfunctional. Among those with functioning PNEN, 10.5% of patients presented with hypoglycemia and were diagnosed with insulinoma, 6.7% of patients presented with symptoms related to carcinoid syndrome; 30.5% of patients showed distant metastases at the time of diagnosis, and surgery was performed in 67.6% of patients. Notably, for five patients with nonfunctional PNEN <2 cm, a "watch and wait" approach was used; none of the patients developed metastatic disease. The median length of hospital stay was 8 days (IQR 5-13). Major postoperative complications were found in 7.0% of patients, and reoperation was conducted for 4.2% of patients, due to postpancreatectomy bleeding (2/71) and abdominal collection (1/71). The median follow-up period was 34 months (IQR 15.0-68.8). The OS at the last follow-up was 75.2% (79/105). The observed 1-, 5- and 10-year survival rates were 87.0, 71.2 and 58.0, respectively. Seven of the surgically treated patients had tumor recurrence. The median time of recurrence was 39 months (IQR 19.0-95.0). A univariable Cox proportional hazard analysis provided evidence that a nonfunctional tumor, a larger tumor size, the presence of distant metastases, a higher tumor grade, and the tumor stage were strong, negative predictors of OS.
Conclusion: Our study represents the general trends of clinicopathological features and treatment of PNEN in Latvia. For PNEN patients, tumor functionality, size, distant metastases, grade, and stage may be useful to predict OS and must be confirmed in further studies. Furthermore, a "surveillance" strategy might be safe for selected patients with small asymptomatic PNEN.
Keywords: epidemiology; pancreatic neuroendocrine neoplasm; postoperative complications; surgery; survival.
© 2023 Ptasnuka, Truskovs, Ozolins, Narbuts, Sperga and Plaudis.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures
References
-
- Rindi G, Capella C, Solcia E. Introduction to a revised clinicopathological classification of neuroendocrine tumors of the gastroenteropancreatic tract. Q J Nucl Med. (2000) 44(1):13–21. - PubMed
LinkOut - more resources
Full Text Sources