This is a preprint.
Quantification of measurable residual disease using duplex sequencing in adults with acute myeloid leukemia
- PMID: 37034683
- PMCID: PMC10081409
- DOI: 10.1101/2023.03.26.23287367
Quantification of measurable residual disease using duplex sequencing in adults with acute myeloid leukemia
Update in
-
Quantification of measurable residual disease using duplex sequencing in adults with acute myeloid leukemia.Haematologica. 2024 Feb 1;109(2):401-410. doi: 10.3324/haematol.2023.283520. Haematologica. 2024. PMID: 37534515 Free PMC article.
Abstract
The presence of measurable residual disease (MRD) is strongly associated with treatment outcomes in acute myeloid leukemia (AML). Despite the correlation with clinical outcomes, MRD assessment has yet to be standardized or routinely incorporated into clinical trials. Discrepancies have been observed between different techniques for MRD assessment and there remains a need to compare centralized, high-quality multiparametric flow cytometry (MFC) and ultrasensitive next-generation sequencing (NGS) in AML patients with diverse mutational profiles. In 62 patients with AML, aged 18-60, in first complete remission after intensive induction therapy on the randomized phase 3 SWOG-S0106 clinical trial, MRD detection by MFC was compared with a 29 gene panel utilizing duplex sequencing (DS), an NGS method that generates double-stranded consensus sequences to reduce false positive errors. Using DS, detection of a persistent mutation utilizing defined criteria was seen in 22 (35%) patients and was strongly associated with higher rates of relapse (68% vs 13% at year 5; HR, 8.8; 95% CI, 3.2-24.5; P<0.001) and decreased survival (32% vs 82% at year 5; HR, 5.6; 95% CI, 2.3-13.8; P<0.001). MRD as defined by DS strongly outperformed MFC, which was observed in 10 (16%) patients and marginally associated with higher rates of relapse (50% vs 30% at year 5; HR, 2.4; 95% CI, 0.9-6.7; P=0.087) and decreased survival (40% vs 68% at year 5; HR, 2.5; 95% CI, 1.0-6.3; P=0.059). Furthermore, the prognostic significance of DS MRD status at the time of remission was similar on both randomized arms of the trial, predicting S0106 clinical trial outcomes. These findings suggest that DS is a powerful tool that could be used in patient management and for early treatment assessment in clinical trials.
Conflict of interest statement
Conflict of Interest
The National Heart, Lung, and Blood Institute receives research funding for the laboratory of CSH from Sellas and the Foundation of the NIH AML MRD Biomarkers Consortium. MO consults for Merck and Biosight and serves on the data safety monitoring committee for Celgene, Glycomimetic, and Grifols. JH, THS, CCV, ES, and JJS are employees and stockholders of TwinStrand Biosciences. BLW consults for Amgen and Kite Pharma. HE: COI: AbbVie; Agios Pharmaceuticals; ALX Oncology; Amgen; Daiichi Sankyo; FORMA Therapeutics; Forty Seven; Gilead Sciences; GlycoMimetics; ImmunoGen; Jazz Pharmaceuticals; MacroGenics; Novartis; PTC Therapeutics; Research Funding: AbbVie; Agios Pharmaceuticals; Bristol Myers Squibb; Celgene; Incyte Corporation; Jazz Pharmaceuticals; Novartis; Speakers Bureau: AbbVie; Independent review committee: AbbVie; Agios Pharmaceuticals; Astellas; Bristol Myers Squibb; Celgene; Daiichi Sankyo; Genentech; GlycoMimetics; Incyte Corporation; Jazz Pharmaceuticals; Kura Oncology.
Figures



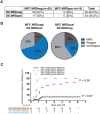

References
-
- Siegel RL, Miller KD, Fuchs HE, Jemal A. Cancer statistics, 2022. CA Cancer J Clin 2022. Jan; 72(1): 7–33. - PubMed
-
- Dohner H, Wei AH, Appelbaum FR, Craddock C, DiNardo CD, Dombret H, et al. Diagnosis and management of AML in adults: 2022 recommendations from an international expert panel on behalf of the ELN. Blood 2022. Sep 22; 140(12): 1345–1377. - PubMed
-
- Short NJ, Fu C, Berry DA, Walter RB, Freeman SD, Hourigan CS, et al. Association of hematologic response and assay sensitivity on the prognostic impact of measurable residual disease in acute myeloid leukemia: a systematic review and meta-analysis. Leukemia 2022. Dec; 36(12): 2817–2826. - PMC - PubMed
Publication types
Grants and funding
LinkOut - more resources
Full Text Sources
