A systematic review of the effect of COVID-19 on semen parameters
- PMID: 37035366
- PMCID: PMC10033148
- DOI: 10.1016/j.heliyon.2023.e14776
A systematic review of the effect of COVID-19 on semen parameters
Abstract
Background and objectives: Since the outbreak of COVID-19, more and more studies have proved that it has an impact on the male reproductive system. The purpose of this article is to investigate the effects of COVID-19 on male semen parameters, further analyze the incidence and risk factors of diseases related to semen parameters, and put forward to corresponding preventive measures.
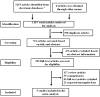
Methods: Retrieved from PubMed, Embase, The Cochrane Library, Web of Science, Clinicaltrails, CNKI, CBM, Wanfang Database and VIP to collect research on the effects of COVID-19 on the male reproductive system. The literature search was conducted until January 2022. In strict accordance with the inclusion and exclusion criteria, two researchers independently screened the literature and comprehensively analyzed five cohort studies on the impact of COVID-19 on male reproductive system. The Newcastle-Ottawa Scale (NOS) was used to evaluate the quality of the included cohort studies, and Revman 5.4.1 was applied for statistical analysis.
Results: Semen volume (RR = -0.10; 95% CI: 0.45, 0.26; P = 0.60), there was no significant difference between the test group and the control group; Sperm count (RR = -45.28; 95% CI: 66.38, 24.19; P = 0.0001), the sperm count of the COVID-19 test group was lower than that of the control group, and the difference was statistically significant; Sperm concentration (RR = -15.65 × 106; 95%CI: 31.52 × 106, 0.21 × 106; P = 0.05), there was no significant difference between the test group and the control group; progressive sperm motility (RR = 4.31; 95% CI: 4.62, 13.24; P = 0.34), there was no effect on progressive sperm motility in the COVID-19 test group compared with the control group.
Conclusions: COVID-19 can reduce semen quality and affect male fertility. However, due to the limitations of this study, this conclusion needs to be further verified by large-sample, high-quality prospective cohort studies on the long-term effects of COVID-19 on male reproductive function.
Keywords: COVID-19; Male fertility; Semen volume; Sperm concentration; Sperm count.
© 2023 Published by Elsevier Ltd.
Conflict of interest statement
The authors declare no competing interests.
Figures
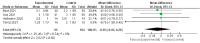


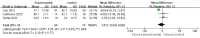

References
-
- Sacha C.R., Vagios S., Hammer K.C., Fitz V.W., Souter I., Bormann C.L. When and where during COVID-19: the effect of at-home semen collection on sperm parameters, fertilization rate, and blastocyst rate. Fertil. Steril. 2020;114(3):e555. doi: 10.1016/j.fertnstert.2020.09.110. - DOI
-
- Holtmann N., Edimiris P., Andree M., Doehmen C., Baston-Buest D., Adams O., et al. Assessment of SARS-CoV-2 in human semen-a cohort study. Fertil. Steril. 2020;114(2):233–238. doi: 10.1016/j.fertnstert.2020.05.028. Epub 2020/07/12. PubMed PMID: 32650948; PubMed Central PMCID: PMCPMC7256599. - DOI - PMC - PubMed
-
- Temiz M.Z., Dincer M.M., Hacibey I., Yazar R.O., Celik C., Kucuk S.H., et al. Investigation of SARS-CoV-2 in semen samples and the effects of COVID-19 on male sexual health by using semen analysis and serum male hormone profile: a cross-sectional, pilot study. Andrologia. 2021;53(2) doi: 10.1111/and.13912. Epub 2020/11/28. PubMed PMID: 33244788; PubMed Central PMCID: PMCPMC7744846. - DOI - PMC - PubMed
Publication types
LinkOut - more resources
Full Text Sources

