Lesion-level correspondence and longitudinal properties of paramagnetic rim and slowly expanding lesions in multiple sclerosis
- PMID: 37036134
- PMCID: PMC10176750
- DOI: 10.1177/13524585231162262
Lesion-level correspondence and longitudinal properties of paramagnetic rim and slowly expanding lesions in multiple sclerosis
Abstract
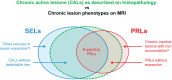
Background: Paramagnetic rim lesions (PRLs) and slowly expanding lesions (SELs) have been posited as markers of chronic active lesions (CALs).
Objective: To assess the lesion-level concordance of PRLs and SELs in MS and to characterize changes in brain tissue integrity in CALs over time.
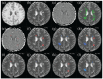
Methods: MRIs were analyzed from a substudy of AFFINITY [NCT03222973], a phase 2 trial of opicinumab in relapsing MS. Assessments included (1) identification of SELs based on longitudinal MRIs over 72 weeks, and identification of PRLs on susceptibility-weighted imaging (SWI) filtered phase images at week 72; (2) evaluation of subject-level correlation of SEL and PRL counts, volumes, and degree of lesion-level overlap between SELs and PRLs; and (3) characterization of tissue integrity over time in overlapping and non-overlapping SELs and PRLs.
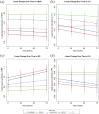
Results: In 41 subjects, 119 chronic PRLs and 267 SELs were detected. Of 119 (39.5%) chronic PRLs, 47 co-localized with a SEL; 46/267 (17.2%) SELs co-localized with a PRL. PRLs co-localized with SELs showed expansion and worsening microstructural damage over time. SELs with and without co-localization with PRLs showed ongoing tissue damage.
Conclusions: Chronic MS lesions identified as both PRL and SEL were associated with the most severe accumulation of tissue damage.
Trial registration: AFFINITY [NCT03222973].
Keywords: Chronic active lesions; MRI; multiple sclerosis; opicinumab; paramagnetic lesions; slow expanding lesions.
Conflict of interest statement
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: C.E. has received speaker honoraria from EMD Serono and is an employee of NeuroRx Research. D.L.A. has received grants from Biogen, Immunotec, and Novartis and consulting fees from Biogen, Celgene, Frequency Therapeutics, Genentech/Roche, Med-Ex Learning, Merck, Novartis, the Population Council, Queens University and Sanofi Aventis, and has an ownership interest in NeuroRx. D.A. has received personal compensation from NeuroRx Research. Z.T. is an employee of Biogen. B.Z., A.G., S.B., D.P.B., and E.F. are employees and shareholders of Biogen. D.A.R., D.F. and A.M.E. have nothing to disclose.
Figures
Similar articles
-
Relationship between paramagnetic rim lesions and slowly expanding lesions in multiple sclerosis.Mult Scler. 2023 Mar;29(3):352-362. doi: 10.1177/13524585221141964. Epub 2022 Dec 14. Mult Scler. 2023. PMID: 36515487 Free PMC article.
-
Longitudinal Multiparametric Quantitative MRI Evaluation of Acute and Chronic Multiple Sclerosis Paramagnetic Rim Lesions.J Magn Reson Imaging. 2025 Apr;61(4):1812-1828. doi: 10.1002/jmri.29583. Epub 2024 Sep 6. J Magn Reson Imaging. 2025. PMID: 39239775 Free PMC article.
-
Slowly expanding lesions relate to persisting black-holes and clinical outcomes in relapse-onset multiple sclerosis.Neuroimage Clin. 2022;35:103048. doi: 10.1016/j.nicl.2022.103048. Epub 2022 May 16. Neuroimage Clin. 2022. PMID: 35598462 Free PMC article.
-
Advances in neuroimaging of multiple sclerosis.Curr Opin Neurol. 2025 Jun 1;38(3):205-216. doi: 10.1097/WCO.0000000000001360. Epub 2025 Mar 19. Curr Opin Neurol. 2025. PMID: 40104925 Review.
-
In vivo imaging of chronic active lesions in multiple sclerosis.Mult Scler. 2022 Apr;28(5):683-690. doi: 10.1177/1352458520958589. Epub 2020 Sep 23. Mult Scler. 2022. PMID: 32965168 Free PMC article. Review.
Cited by
-
B cell depletion therapy does not resolve chronic active multiple sclerosis lesions.EBioMedicine. 2023 Aug;94:104701. doi: 10.1016/j.ebiom.2023.104701. Epub 2023 Jul 10. EBioMedicine. 2023. PMID: 37437310 Free PMC article.
-
Changes in MRI Workflow of Multiple Sclerosis after Introduction of an AI-Software: A Qualitative Study.Healthcare (Basel). 2024 May 9;12(10):978. doi: 10.3390/healthcare12100978. Healthcare (Basel). 2024. PMID: 38786390 Free PMC article.
-
Determinants of long-term paramagnetic rim lesion evolution in people with multiple sclerosis.Ann Clin Transl Neurol. 2025 Feb;12(2):267-279. doi: 10.1002/acn3.52253. Epub 2024 Nov 18. Ann Clin Transl Neurol. 2025. PMID: 39556505 Free PMC article.
-
Imaging chronic active lesions in multiple sclerosis: a consensus statement.Brain. 2024 Sep 3;147(9):2913-2933. doi: 10.1093/brain/awae013. Brain. 2024. PMID: 38226694 Free PMC article. Review.
-
Advanced MRI Techniques: Diagnosis and Follow-Up of Multiple Sclerosis.Diagnostics (Basel). 2024 May 28;14(11):1120. doi: 10.3390/diagnostics14111120. Diagnostics (Basel). 2024. PMID: 38893646 Free PMC article. Review.
References
-
- Kuhlmann T, Ludwin S, Prat A, et al.. An updated histological classification system for multiple sclerosis lesions. Acta Neuropathol 2017; 133(1): 13–24. - PubMed
-
- Fransen NL, Hsiao CC, van der Poel M, et al.. Tissue-resident memory T cells invade the brain parenchyma in multiple sclerosis white matter lesions. Brain 2020; 143(6): 1714–1730. - PubMed
-
- Ramaglia V, Rojas O, Naouar I, et al.. The ins and outs of central nervous system inflammation — lessons learned from multiple sclerosis. Ann Rev Immunol 2021; 39(1): 199–226. - PubMed
Publication types
MeSH terms
Associated data
LinkOut - more resources
Full Text Sources
Medical
Research Materials

