Tumour budding-based grading as independent prognostic biomarker in HPV-positive and HPV-negative head and neck cancer
- PMID: 37045906
- PMCID: PMC10241901
- DOI: 10.1038/s41416-023-02240-y
Tumour budding-based grading as independent prognostic biomarker in HPV-positive and HPV-negative head and neck cancer
Erratum in
-
Correction: Tumour budding-based grading as independent prognostic biomarker in HPV-positive and HPV-negative head and neck cancer.Br J Cancer. 2024 Feb;130(3):511. doi: 10.1038/s41416-023-02521-6. Br J Cancer. 2024. PMID: 38191610 Free PMC article. No abstract available.
Abstract
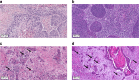
Background: The prognostic significance of tumour budding (TB) and minimal cell nest size (MCNS) was shown in human papillomavirus (HPV)-negative head and neck squamous cell carcinomas (HNSCC). However, the optimisation of cutpoints, the prognostic impact in HPV-positive HNSCC, and the comparison with other histopathological grading systems are insufficiently investigated.
Methods: TB and MCNS were analysed digitally in 1 and 10 high-power fields (HPF) of 331 HPV-positive and HPV-negative cases from TCGA. Optimising the cutpoints a new cellular dissociation grading (CDG) system was defined and compared to the WHO grading and the Brandwein-Gensler (BG) risk model.
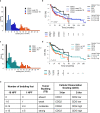
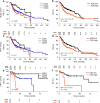
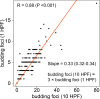
Results: The two-tiered CDG system based solely on TB yielded optimal prognostic stratification with shortened overall survival for CDG-high cases. Optimal cut-offs were two buds (1 HPF) and six buds (10 HPF), respectively. Analysing MCNS did not add prognostic significance to quantifying TB. CDG was a significant prognostic marker in HPV-negative and HPV-positive tumours and prognostically superior to the WHO and BG systems. High CDG was associated with clinically occult lymph-node metastases.
Conclusions: The most comprehensive study of TB in HNSCC so far confirmed its prognostic impact in HPV-negative tumours and for the first time in HPV-positive tumours. Further studies are warranted to evaluate its applicability for therapy guidance in HNSCC.
© 2023. The Author(s).
Conflict of interest statement
PS: Speaker’s fees: AstraZeneca, Incyte, Janssen. Advisory Boards: BMS, MSD, AstraZeneca, Roche. Funding for research: Roche, Chugai, BMS, Novartis. AS: Advisory Board/Speaker’s Bureau: Astra Zeneca, AGCT, Bayer, BMS, Eli Lilly, Illumina, Janssen, MSD, Novartis, Pfizer, Roche, Seattle Genetics, Takeda, Thermo Fisher. Grants: Bayer, BMS, Chugai, Incyte. WW: Advisory Boards and speaker’s fees: Roche, MSD, BMS, AstraZeneca, Pfizer, Merck, Lilly, Boehringer, Novartis, Takeda, Bayer, Amgen, Astellas, Eisai, Illumina, Siemens, Agilent, ADC, GSK and Molecular Health. Funding for research: Roche, MSD, BMS and AstraZeneca. MB: Funding through Deutsche Krebshilfe (German Cancer Aid). Advisory Board and speaker´s fee: BMS, MSD. Funding: BMS. JB: Funding through Deutsche Krebshilfe (German Cancer Aid). The remaining authors declare no competing interests.
Figures

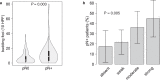
Comment in
-
Tumour budding in head and neck cancer: what have we learnt and the next steps towards clinical implementation.Br J Cancer. 2024 Jan;130(1):1-2. doi: 10.1038/s41416-023-02531-4. Epub 2023 Dec 14. Br J Cancer. 2024. PMID: 38097743 Free PMC article. No abstract available.
Similar articles
-
Dynamic changes of the EMT spectrum between circulating tumor cells and the tumor microenvironment in human papillomavirus-positive head and neck squamous cell carcinoma.Oral Oncol. 2023 Feb;137:106296. doi: 10.1016/j.oraloncology.2022.106296. Epub 2022 Dec 24. Oral Oncol. 2023. PMID: 36571985
-
HPV genotypes and their prognostic significance in head and neck squamous cell carcinomas.J Clin Virol. 2012 Feb;53(2):116-20. doi: 10.1016/j.jcv.2011.11.005. Epub 2011 Dec 15. J Clin Virol. 2012. PMID: 22177275
-
Antibody Responses to Cancer Antigens Identify Patients with a Poor Prognosis among HPV-Positive and HPV-Negative Head and Neck Squamous Cell Carcinoma Patients.Clin Cancer Res. 2019 Dec 15;25(24):7405-7412. doi: 10.1158/1078-0432.CCR-19-1490. Epub 2019 Aug 23. Clin Cancer Res. 2019. PMID: 31444248
-
Human Papillomavirus Infection in Head and Neck Squamous Cell Carcinomas: Transcriptional Triggers and Changed Disease Patterns.Front Cell Infect Microbiol. 2020 Dec 2;10:537650. doi: 10.3389/fcimb.2020.537650. eCollection 2020. Front Cell Infect Microbiol. 2020. PMID: 33344262 Free PMC article. Review.
-
Quantitative diffusion magnetic resonance imaging for prediction of human papillomavirus status in head and neck squamous-cell carcinoma: A systematic review and meta-analysis.Neuroradiol J. 2019 Aug;32(4):232-240. doi: 10.1177/1971400919849808. Epub 2019 May 14. Neuroradiol J. 2019. PMID: 31084347 Free PMC article.
Cited by
-
Multi-omics analysis to uncover the molecular basis of tumor budding in head and neck squamous cell carcinoma.NPJ Precis Oncol. 2025 Mar 13;9(1):73. doi: 10.1038/s41698-025-00856-2. NPJ Precis Oncol. 2025. PMID: 40082664 Free PMC article.
-
Tumour budding in head and neck cancer: what have we learnt and the next steps towards clinical implementation.Br J Cancer. 2024 Jan;130(1):1-2. doi: 10.1038/s41416-023-02531-4. Epub 2023 Dec 14. Br J Cancer. 2024. PMID: 38097743 Free PMC article. No abstract available.
-
Tumor budding and lymphovascular invasion as prognostic factors in p16-positive oropharyngeal squamous cell carcinomas.Br J Cancer. 2025 Feb;132(2):212-221. doi: 10.1038/s41416-024-02912-3. Epub 2024 Nov 29. Br J Cancer. 2025. PMID: 39613843 Free PMC article.
-
Segmentation-Free Outcome Prediction from Head and Neck Cancer PET/CT Images: Deep Learning-Based Feature Extraction from Multi-Angle Maximum Intensity Projections (MA-MIPs).Cancers (Basel). 2024 Jul 14;16(14):2538. doi: 10.3390/cancers16142538. Cancers (Basel). 2024. PMID: 39061178 Free PMC article.
-
The modified Polsby-Popper score, a novel quantitative histomorphological biomarker and its potential to predict lymph node positivity and cancer-specific survival in oral tongue squamous cell carcinoma.Cancer Med. 2024 Jan;13(1):e6824. doi: 10.1002/cam4.6824. Epub 2023 Dec 22. Cancer Med. 2024. PMID: 38132808 Free PMC article.
References
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical

