Relentless placoid chorioretinitis: A review of four cases in pediatric and young adult patients with a discussion of therapeutic strategies
- PMID: 37051435
- PMCID: PMC10083237
- DOI: 10.3389/fped.2023.885230
Relentless placoid chorioretinitis: A review of four cases in pediatric and young adult patients with a discussion of therapeutic strategies
Abstract
Introduction: Relentless placoid chorioretinitis (RPC) is a rare, bilateral disease of the retinal pigment epithelium. The clinical course is prolonged and relapsing. No standard treatment has been established to date. The purpose of this case series is to report four cases of RPC in pediatric and young adult patients in which varying treatments were used, comparing them to previously published cases.
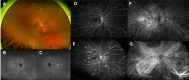
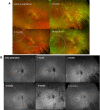
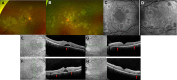
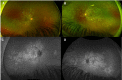
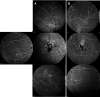
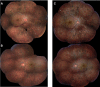
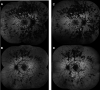
Methods: A literature review was conducted to investigate currently published presentations and treatment options for RPC. A multicenter retrospective chart review was also performed on four consecutive patients. These patients were diagnosed with RPC because of new chorioretinitis lesions continuing to appear without or despite therapy for 5-36 months (2 patients), with a clinical course prolonged and relapsing, or because of the atypical location of the multiple lesions (>50) extending from the posterior pole to the equator and mid-peripheral retina (all four patients), which were not consistent with other entities like acute posterior multifocal placoid pigment epitheliopathy and serpiginous choroiditis.
Results: All four cases of RPC received oral or IV steroids acutely, and three of these patients were transitioned to a steroid-sparing agent and biologic therapy: anti-TNF alpha or anti-IL-6. Quiescence of the chorioretinitis lesions was obtained after 7 months, 1 month, and 36 months; however, the latter had issues with treatment adherence. Mycophenolate mofetil was insufficient to control the disease in one patient, but tocilizumab and infliximab thereafter were effective after cessation of adalimumab due to side effects. Adalimumab when started the first month after the presentation was effective in controlling the disease in one patient. After the failure of interferon-alpha-2a, one patient displayed long-term control with infliximab. One patient did not require a steroid-sparing agent after oral prednisone taper as there was no evidence of progression or recurrence.
Conclusion: This case series adds to the current knowledge regarding potential treatments for RPC, specifically the use of anti-TNF-alpha treatment and anti-IL-6 tocilizumab. In this case study, relapses of RPC were found among patients on mycophenolate mofetil and interferon-alpha-2a, and one case did not relapse on oral steroids without a steroid-sparing agent. Our findings suggest that adalimumab, infliximab, and tocilizumab may be useful medications to obtain quiescence of RPC.
Keywords: adalimumab; infliximab; interferon-alpha-2a; relentless placoid chorioretinitis; tocilizumab; uveitis.
© 2023 Zaheer, Odden, Gagrani, Zaguia, Lowder, Coca, Rosenkranz, Patil, Ores, Boussion,Indermill, Sedira, Sahel, Nischal, Goldstein and Errera.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures





Similar articles
-
Relentless Placoid Chorioretinitis: A Case Series of Successful Tapering of Systemic Immunosuppressants Achieved with Adalimumab.Case Rep Ophthalmol. 2019 May 2;10(1):145-152. doi: 10.1159/000500077. eCollection 2019 Jan-Apr. Case Rep Ophthalmol. 2019. PMID: 31143110 Free PMC article.
-
Cyclosporine and prednisolone combination therapy as a potential therapeutic strategy for relentless placoid chorioretinitis.Am J Ophthalmol Case Rep. 2019 Mar 23;14:87-91. doi: 10.1016/j.ajoc.2019.03.005. eCollection 2019 Jun. Am J Ophthalmol Case Rep. 2019. PMID: 30984889 Free PMC article.
-
Long-term follow-up of a bilateral acute posterior multifocal placoid pigment epitheliopathy following COVID-19 infection: a case report.J Ophthalmic Inflamm Infect. 2024 Jan 4;14(1):2. doi: 10.1186/s12348-023-00382-x. J Ophthalmic Inflamm Infect. 2024. PMID: 38177891 Free PMC article.
-
Relentless placoid chorioretinitis.Surv Ophthalmol. 2025 Jul 22:S0039-6257(25)00127-4. doi: 10.1016/j.survophthal.2025.07.009. Online ahead of print. Surv Ophthalmol. 2025. PMID: 40706821 Review.
-
Placoid lesions of the retina: progress in multimodal imaging and clinical perspective.Br J Ophthalmol. 2022 Jan;106(1):14-25. doi: 10.1136/bjophthalmol-2020-318337. Epub 2021 Jan 19. Br J Ophthalmol. 2022. PMID: 33468489 Review.
Cited by
-
Relentless Placoid Chorioretinitis: A Differential Diagnosis and Management Approach in a Challenging Case.Cureus. 2025 Jul 24;17(7):e88688. doi: 10.7759/cureus.88688. eCollection 2025 Jul. Cureus. 2025. PMID: 40861541 Free PMC article.
-
Changes in optical coherence tomography (OCT) parameters in follow-up of acute posterior multifocal placoid pigment epitheliopathy (APMPPE).Int Ophthalmol. 2025 Aug 22;45(1):344. doi: 10.1007/s10792-025-03718-9. Int Ophthalmol. 2025. PMID: 40844668
References
-
- Jones BE, Jampol LM, Yannuzzi LA, Tittl M, Johnson MW, Han DP, et al. Relentless placoid chorioretinitis: a new entity or an unusual variant of serpiginous chorioretinitis? Arch Ophthalmol. (2000) 118(7):931–8. 10-1001/pubs.Ophthalmol.-ISSN-0003-9950-118-7-ecs80142 - PubMed
Publication types
LinkOut - more resources
Full Text Sources

