Spinal Extramedullary Arteriovenous Fistulas: A 15-Year Endovascular Treatment Experience in a Tertiary Care Hospital in Thailand
- PMID: 37055176
- PMCID: PMC10478700
- DOI: 10.14444/8446
Spinal Extramedullary Arteriovenous Fistulas: A 15-Year Endovascular Treatment Experience in a Tertiary Care Hospital in Thailand
Abstract
Background: Spinal arteriovenous shunts are rare diseases. Different classifications have been proposed, but the most widely used are those classified by locations. Different locations (i.e., intramedullary and extramedullary) have different treatment outcomes and different posttreatment angiographical results. Our study presents the 15-year endovascular treatment outcomes of patients who had spinal extramedullary arteriovenous fistulas (AVFs) at Ramathibodi Hospital, which is a tertiary care hospital in Thailand.
Methods: A retrospective medical record and imaging review of all patients with spinal extramedullary AVFs, which were confirmed by a diagnostic spinal angiogram in our institute from January 2006 to December 2020, were performed. The angiographic complete obliteration rate in the first session of endovascular treatment, clinical outcomes of the patients, and complications of the procedures for all eligible patients were analyzed.
Results: Sixty-eight eligible patients were included in the study. The most common diagnosis was spinal dural AVF (45.6%). The most common presenting symptoms were weakness, numbness, and bowel-bladder involvement (70.6%, 67.6%, and 57.4%, respectively). Ninety-four percent had spinal cord edema in preoperative magnetic resonance imaging. All patients had pial venous reflux. Sixty-four patients (94.1%) received endovascular treatment as the first option. The complete obliteration rate in the first session of endovascular treatment was 75% and was high in all subgroups except for the perimedullary AVF group. The overall intraoperative complication of endovascular treatment was 9.4%. Follow-up imaging showed no residual AVF in 50 patients (87.7%). Most of the patients (57.4%) had improvement of neurological functions at 3- to 6-month follow-up.
Conclusion: Treatment results of spinal extramedullary AVFs were good in terms of angiographic aspects and clinical outcomes. This may have resulted from the locations of the AVFs, which mostly did not involve the spinal cord arterial supply, with the exception of perimedullary AVFs. Although perimedullary AVF is difficult to treat, it can be cured by careful catherization and embolization.
Keywords: Spinal arteriovenous shunts; angiographic complete obliteration rate; endovascular treatment.
This manuscript is generously published free of charge by ISASS, the International Society for the Advancement of Spine Surgery. Copyright © 2023 ISASS. To see more or order reprints or permissions, see http://ijssurgery.com.
Conflict of interest statement
Declaration of Conflicting Interests : The authors declare no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
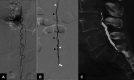
Figures




Similar articles
-
Multimodal treatment strategies for complex pediatric cerebral arteriovenous fistulas: contemporary case series at Barrow Neurological Institute.J Neurosurg Pediatr. 2015 Jun;15(6):615-24. doi: 10.3171/2014.11.PEDS14468. Epub 2015 Mar 27. J Neurosurg Pediatr. 2015. PMID: 25815632
-
Endovascular embolization for symptomatic perimedullary AVF and intramedullary AVM: a series and a literature review.Neuroradiology. 2012 Apr;54(4):349-59. doi: 10.1007/s00234-011-0880-0. Epub 2011 May 10. Neuroradiology. 2012. PMID: 21556862
-
Microsurgical or endovascular strategy for complete obliteration of spinal arteriovenous shunts in a single-institute 10-year retrospective study.J Clin Neurosci. 2020 Oct;80:195-202. doi: 10.1016/j.jocn.2020.08.015. Epub 2020 Aug 26. J Clin Neurosci. 2020. PMID: 33099345
-
Spinal Arteriovenous Shunts: Angioarchitecture and Historical Changes in Classification.Neurol Med Chir (Tokyo). 2017 Jul 15;57(7):356-365. doi: 10.2176/nmc.ra.2016-0316. Epub 2017 May 18. Neurol Med Chir (Tokyo). 2017. PMID: 28515372 Free PMC article. Review.
-
Treatment of high cervical arteriovenous fistulas in the craniocervical junction region.Front Neurol. 2023 Jun 27;14:1164548. doi: 10.3389/fneur.2023.1164548. eCollection 2023. Front Neurol. 2023. PMID: 37441609 Free PMC article. Review.
Cited by
-
An Update on Spinal Dural Arteriovenous Fistulae: Case Series and Systematic Review.Cureus. 2024 Jul 27;16(7):e65537. doi: 10.7759/cureus.65537. eCollection 2024 Jul. Cureus. 2024. PMID: 39188459 Free PMC article.
References
LinkOut - more resources
Full Text Sources
