Isolating Neurologic Deficits in Cervical Spondylotic Myelopathy: A Case-Controlled Study, Using the NIH Toolbox Motor Battery
- PMID: 37064579
- PMCID: PMC10101713
- DOI: 10.1212/CPJ.0000000000200126
Isolating Neurologic Deficits in Cervical Spondylotic Myelopathy: A Case-Controlled Study, Using the NIH Toolbox Motor Battery
Abstract
Background and objectives: Patients with cervical spondylotic myelopathy (CSM) have motor impairments, including weakness, imbalance, and loss of dexterity. The reliable assessment of these symptoms is critical for treatment decisions. This study aimed to determine, for the first time, the use of the NIH Toolbox motor battery (NIHTBm) in the objective assessment of motor deficits in patients with CSM.
Methods: Patients with symptoms and MRI evidence of CSM and age-matched healthy controls (HC), with no evidence of spinal disorder or surgery were included in this case-control study based on our inclusion and exclusion criteria. We performed motor tests, dexterity, gait speed, grip strength, and balance tests, using the NIHTBm in patients with CSM and HCs. Motor impairment rates were determined in patients with CSM based on the NIHTBm scores. We determined the association between NIHTBm scores and patient-reported outcome scores; patient-reported outcome measures (the modified Japanese Orthopedic Association [mJOA] and Nurick grade) to determine the association. One-way analysis of variance was used to analyze group differences and the Spearman rank correlation to determine the relationship between assessment scores.
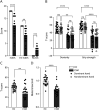
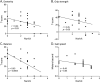
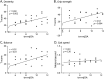
Results: We enrolled 24 patients with CSM with a mean age (SD) of 57.96 (10.61) years and 24 age-matched HCs with a mean age (SD) of 53.17 (6.04) years in this study. Overall, we observed a significant decrease in the motor function T-scores mean (SD): dexterity 31.54 (14.82) vs 51.54 (9.72), grip strength 32.00 (17.47) vs 56.79 (8.46), balance 27.58 (16.65) vs 40.21 (6.35), and gait speed 0.64 (0.18) vs 0.99 (0.17) m/s, in patients with CSM compared with that in HCs. The lower extremity dysfunction scores on the NIHTBm, balance (ρ = -0.67) and gait speed (ρ = -0.62), were associated with higher Nurick grades. We observed a similar but weaker association with the Nurick grades and NIHTBm tests: dexterity (ρ = -0.49) and grip strength (ρ = -0.31) scores. The total motor mJOA showed a positive but weak association with NIHTBm scores, gait speed (ρ = 0.38), balance (ρ = 0.49), grip strength (ρ = 0.41), and dexterity (ρ = 0.45).
Discussion: Patients with CSM had significantly lower NIHTBm scores compared with HCs. The results from the NIHTBm are consistent with the clinical presentation of CSM showing patients have motor impairments in both upper and lower extremities. As a neurologic-specific scale, NIHTBm should be used in the evaluation and clinical management of patients with CSM.
Copyright © 2023 The Author(s). Published by Wolters Kluwer Health, Inc. on behalf of the American Academy of Neurology.
Conflict of interest statement
F. Muhammad, A. Baha, G. Haynes, H. Shakir, M. Omini, and M. Martin report no disclosures relevant to the manuscript. K.A. Weber II received funding from the National Institute on Neurologic Disorders and Stroke (grant K23NS104211 and L30NS108301). M. Paliwal, M. Van Hal, and D. Dickson report no disclosures relevant to the manuscript. Y. Dhaher received funding from the National Institute of Arthritis and Musculoskeletal and Skin Diseases (grant R01 AR06976-03). Y.D. Zhao reports no disclosures relevant to the manuscript. Z.A. Smith is funded by NIH-NINDS K23 grant K23NS091430, Presbyterian Health Foundation Team Science Research, and Oklahoma Shared Clinical and Translational Research (OSCTR) NIH-IDeA grant. Full disclosure form information provided by the authors is available with the full text of this article at Neurology.org/cp.
Figures
References
-
- Revanappa K, Moorthy R, Jeyaseelan V, Rajshekhar V. Modification of Nurick scale and Japanese Orthopedic Association score for Indian population with cervical spondylotic myelopathy. Neurol India. 2015;63(1):24-29. - PubMed
Grants and funding
LinkOut - more resources
Full Text Sources
Research Materials
