Propensity for Clinically Meaningful Improvement and Surgical Failure After Anterior Cruciate Ligament Repair
- PMID: 37065184
- PMCID: PMC10102942
- DOI: 10.1177/23259671221146815
Propensity for Clinically Meaningful Improvement and Surgical Failure After Anterior Cruciate Ligament Repair
Abstract
Background: Primary repair of the anterior cruciate ligament (ACL) confers an alternative to ACL reconstruction in appropriately selected patients.
Purpose: To prospectively assess survivorship and to define the clinically meaningful outcomes after ACL repair.
Study design: Case series; Level of evidence, 4.
Methods: Included were consecutive patients with Sherman grade 1-2 tears who underwent primary ACL repair with or without suture augmentation between 2017 and 2019. Patient-reported outcomes (Lysholm, Tegner, International Knee Documentation Committee, Western Ontario and McMaster Universities Osteoarthritis Index, and Knee injury and Osteoarthritis Outcome Score [KOOS] subscales) were collected preoperatively and at 6 months, 1 year, and 2 years postoperatively. The minimal clinically important difference (MCID) was calculated using a distribution-based method, whereas the Patient Acceptable Symptom State (PASS) and substantial clinical benefit (SCB) were calculated using an anchor-based method. Plain radiographs and magnetic resonance imaging (MRI) were obtained at 6 months, 1 year, and 2 years postoperatively.
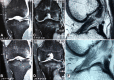
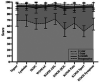
Results: A total of 120 patients were included. The overall failure rate was 11.3% at 2 years postoperatively. Changes in outcome scores required to achieve the MCID ranged between 5.1 and 14.3 at 6 months, 4.6 and 8.4 at 1 year, and 4.7 and 11.9 at 2 years postoperatively. Thresholds for PASS achievement ranged between 62.5 and 89 at 6 months, 75 and 89 at 1 year, and 78.6 and 93.2 at 2 years postoperatively. Threshold scores (absolute/change based) for achieving the SCB ranged between 82.8 and 96.4/17.7 and 40.1 at 6 months, between 94.7 and 100/23 and 45 at 1 year, and between 95.3 and 100/29.4 and 45 at 2 years. More patients achieved the MCID and PASS at 1 year compared with 6 months and 2 years. For SCB, this trend was also observed for non-KOOS outcomes, while for KOOS subdomains, more patients achieved the SCB at 2 years. High-intensity signal of the ACL repair (odds ratio [OR], 31.7 [95% CI, 1.5-73.4]; P = .030) and bone contusions on MRI (OR, 4.2 [95% CI, 1.7-25.2]; P = .041) at 1 year postoperatively were independently associated with increased risk of ACL repair failure.
Conclusion: The rate of clinically meaningful outcome improvement was high early after ACL repair, with the greatest proportion of patients achieving the MCID, PASS, and SCB at 1 year postoperatively. Bone contusions involving the posterolateral tibia and lateral femoral condyle as well as high repair signal intensity at 1 year postoperatively were independent predictors of failure at 2 years postoperatively.
Keywords: ACL; MCID; PASS; SCB; clinical outcomes; repair.
© The Author(s) 2023.
Conflict of interest statement
One or more of the authors has declared the following potential conflict of interest or source of funding: R.M. has received consulting fees from Smith & Nephew. J.C. has received education payments from Arthrex and Smith & Nephew; consulting fees from Arthrex, DePuy Synthes, Linvatec, and Smith & Nephew; speaking fees from Linvatec; and hospitality payments from Stryker. AOSSM checks author disclosures against the Open Payments Database (OPD). AOSSM has not conducted an independent investigation on the OPD and disclaims any liability or responsibility relating thereto.
Figures

References
-
- Ahmad SS, Difelice GS, van der List JP, Ateschrang A, Hirschmann MT. Primary repair of the anterior cruciate ligament: real innovation or reinvention of the wheel? Knee Surg Sports Traumatol Arthrosc. 2019;27(1):1–2. - PubMed
-
- Beck EC, Nwachukwu BU, Kunze KN, Chahla J, Nho SJ. How can we define clinically important improvement in pain scores after hip arthroscopy for femoroacetabular impingement syndrome? minimum 2-year follow-up study. Am J Sports Med. 2019;47(13):3133–3140. - PubMed
-
- Beletsky A, Naami E, Lu Y, et al.The patient acceptable symptomatic state in primary anterior cruciate ligament reconstruction: predictors of achievement. Arthroscopy. 2021;37(2):600–605. - PubMed
-
- Biercevicz AM, Miranda DL, Machan JT, Murray MM, Fleming BC. In situ, noninvasive, T2*-weighted MRI-derived parameters predict ex vivo structural properties of an anterior cruciate ligament reconstruction or bioenhanced primary repair in a porcine model. Am J Sports Med. 2013;41(3):560–566. - PMC - PubMed
LinkOut - more resources
Full Text Sources

