Serum HBsAg and HBcrAg is associated with inflammation in HBeAg-positive chronic hepatitis B patients
- PMID: 37065191
- PMCID: PMC10102387
- DOI: 10.3389/fcimb.2023.1083912
Serum HBsAg and HBcrAg is associated with inflammation in HBeAg-positive chronic hepatitis B patients
Abstract
Backgrounds & aims: Liver inflammation is the main risk factor for developing liver fibrosis, cirrhosis, and even hepatocellular carcinoma in chronic hepatitis B (CHB) patients. To replace biopsy, additional non-invasive biomarkers to diagnose and grade liver necroinflammation are urgently required in clinical practice.
Method: Ninety-four CHB patients, including 74 HBeAg-positive and 20 HBeAg-negative patients, were enrolled and started entecavir or adefovir therapy. Serum HBV RNA, HBV DNA, HBsAg, hepatitis B core-related antigen (HBcrAg), ALT and AST levels, as well as intrahepatic HBV DNA and cccDNA were measured at baseline and during treatment. Liver inflammation was assessed at baseline and month 60 by liver biopsy. Inflammation regression was defined as a ≥1-grade decrease according to the Scheuer scoring system.
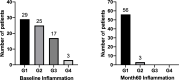
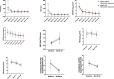
Results: In HBeAg-positive CHB patients, at baseline, serum HBsAg and HBcrAg levels negatively correlated with inflammation grade, while ALT and AST levels positively correlated with inflammation grade. AST plus HBsAg exhibited excellent diagnostic ability for significant inflammation with an AUROC of 0.896. After 60 months of antiviral treatment, almost all the patients' liver inflammation ameliorated to G1, and no patients had inflammation progression.
Conclusion: Besides ALT and AST, serum HBsAg and HBcrAg correlated with inflammation grade in HBeAg-positive CHB patients before NAs treatment. Moreover, the combination of HBsAg and AST exhibited excellent diagnostic ability for significant inflammation.
Keywords: HBcrAg; HBsAg; chronic hepatitis B; inflammation; nucleos(t)ide analogues.
Copyright © 2023 Zhao, Bian, Liao, Wang, Ren, Jiang, Liu, Chen, Hu, Duan, Lu and Zheng.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures


Similar articles
-
Correlation of HBcrAg with Intrahepatic Hepatitis B Virus Total DNA and Covalently Closed Circular DNA in HBeAg-Positive Chronic Hepatitis B Patients.J Clin Microbiol. 2019 Jan 2;57(1):e01303-18. doi: 10.1128/JCM.01303-18. Print 2019 Jan. J Clin Microbiol. 2019. PMID: 30355757 Free PMC article.
-
Serum HBV RNA is associated with liver fibrosis regression in HBeAg-positive chronic hepatitis B patients treated with nucleos(t)ide analogues.J Viral Hepat. 2023 Apr;30(4):303-309. doi: 10.1111/jvh.13790. Epub 2023 Jan 10. J Viral Hepat. 2023. PMID: 36533536
-
Serum HBV DNA plus RNA reflecting cccDNA level before and during NAs treatment in HBeAg positive CHB patients.Int J Med Sci. 2022 May 9;19(5):858-866. doi: 10.7150/ijms.71737. eCollection 2022. Int J Med Sci. 2022. PMID: 35693741 Free PMC article.
-
A critique and systematic review of the clinical utility of hepatitis B core-related antigen.J Hepatol. 2023 Apr;78(4):731-741. doi: 10.1016/j.jhep.2022.12.017. Epub 2022 Dec 28. J Hepatol. 2023. PMID: 36586590
-
Review article: hepatitis B core-related antigen (HBcrAg): an emerging marker for chronic hepatitis B virus infection.Aliment Pharmacol Ther. 2018 Jan;47(1):43-54. doi: 10.1111/apt.14376. Epub 2017 Oct 16. Aliment Pharmacol Ther. 2018. PMID: 29035003 Review.
Cited by
-
Monocyte distribution width as a promising biomarker for differential diagnosis of chronic hepatitis, cirrhosis, and hepatocellular carcinoma.Front Immunol. 2024 Jul 3;15:1406671. doi: 10.3389/fimmu.2024.1406671. eCollection 2024. Front Immunol. 2024. PMID: 39021573 Free PMC article.
-
Evaluating the relationship between hepatitis B viral activity and gestational diabetes mellitus: A prospective cohort study.Womens Health (Lond). 2024 Jan-Dec;20:17455057241265083. doi: 10.1177/17455057241265083. Womens Health (Lond). 2024. PMID: 39051642 Free PMC article.
-
Clinical significance of liver biopsy in the diagnosis of liver disease and the evaluation of the clinical efficacy of antiviral treatment for chronic hepatitis B.Am J Transl Res. 2024 Sep 15;16(9):4867-4875. doi: 10.62347/QQEI5676. eCollection 2024. Am J Transl Res. 2024. PMID: 39398561 Free PMC article.
-
Identification and evaluation of biomarkers for diagnosis of chronic hepatitis B using RNA-seq.Virus Res. 2025 Aug;358:199589. doi: 10.1016/j.virusres.2025.199589. Epub 2025 Jun 4. Virus Res. 2025. PMID: 40480312 Free PMC article.
-
Schizandrin C regulates lipid metabolism and inflammation in liver fibrosis by NF-κB and p38/ERK MAPK signaling pathways.Front Pharmacol. 2023 May 23;14:1092151. doi: 10.3389/fphar.2023.1092151. eCollection 2023. Front Pharmacol. 2023. PMID: 37288106 Free PMC article.
References
-
- Dufour D. R., Lott J. A., Nolte F. S., Gretch D. R., Koff R. S., Seeff L. B. (2000). Diagnosis and monitoring of hepatic injury. II. recommendations for use of laboratory tests in screening, diagnosis, and monitoring. Clin. Chem. 46 (12), 2050–2068. doi: 10.1093/clinchem/46.12.2050 - DOI - PMC - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical

