Coexistent Relapsing Polychondritis and Clinically Amyopathic Dermatomyositis: A Rare Association of Autoimmune Disorders
- PMID: 37082027
- PMCID: PMC10113061
- DOI: 10.1155/2023/3719502
Coexistent Relapsing Polychondritis and Clinically Amyopathic Dermatomyositis: A Rare Association of Autoimmune Disorders
Abstract
Relapsing polychondritis (RPC) is an uncommon autoimmune systemic disease characterized by recurrent inflammation of the cartilage tissue. It can occur alone or in association with other autoimmune diseases, vasculitis, or hematologic disorders. However, the association of RPC with dermatomyositis is extremely rare. Herein, we present a case of a 38-year-old man who developed concurrent RPC and clinically amyopathic dermatomyositis (CADM) manifested by auricular chondritis, nasal chondritis, polyarthritis, gottron papules, fingertip papules, skin biopsy consistent with dermatomyositis, and positive antimelanoma differentiation-associated gene 5 (MDA5) antibodies. RPC features resolved with corticosteroids, but CADM manifestations were resistant to corticosteroids, cyclophosphamide, azathioprine, and hydroxychloroquine. Subsequent therapy with rituximab was effective to control CADM manifestations. This case highlights the importance of recognizing CADM as part of the autoimmune diseases linked with RPC and maintaining a high level of awareness to initiate effective therapy to avoid the long-term complications associated with these conditions.
Copyright © 2023 Rafael A. Ríos-Rivera and Luis M. Vilá.
Conflict of interest statement
The authors declare that there are no conflicts of interest regarding the publication of this article.
Figures
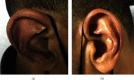

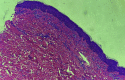

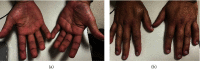
References
Publication types
LinkOut - more resources
Full Text Sources

