Diagnostic models predicting paediatric viral acute respiratory infections: a systematic review
- PMID: 37085296
- PMCID: PMC10124282
- DOI: 10.1136/bmjopen-2022-067878
Diagnostic models predicting paediatric viral acute respiratory infections: a systematic review
Abstract
Objectives: To systematically review and evaluate diagnostic models used to predict viral acute respiratory infections (ARIs) in children.
Design: Systematic review.
Data sources: PubMed and Embase were searched from 1 January 1975 to 3 February 2022.
Eligibility criteria: We included diagnostic models predicting viral ARIs in children (<18 years) who sought medical attention from a healthcare setting and were written in English. Prediction model studies specific to SARS-CoV-2, COVID-19 or multisystem inflammatory syndrome in children were excluded.
Data extraction and synthesis: Study screening, data extraction and quality assessment were performed by two independent reviewers. Study characteristics, including population, methods and results, were extracted and evaluated for bias and applicability using the Checklist for Critical Appraisal and Data Extraction for Systematic Reviews of Prediction Modelling Studies and PROBAST (Prediction model Risk Of Bias Assessment Tool).
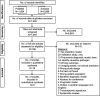
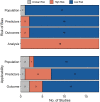
Results: Of 7049 unique studies screened, 196 underwent full text review and 18 were included. The most common outcome was viral-specific influenza (n=7; 58%). Internal validation was performed in 8 studies (44%), 10 studies (56%) reported discrimination measures, 4 studies (22%) reported calibration measures and none performed external validation. According to PROBAST, a high risk of bias was identified in the analytic aspects in all studies. However, the existing studies had minimal bias concerns related to the study populations, inclusion and modelling of predictors, and outcome ascertainment.
Conclusions: Diagnostic prediction can aid clinicians in aetiological diagnoses of viral ARIs. External validation should be performed on rigorously internally validated models with populations intended for model application.
Prospero registration number: CRD42022308917.
Keywords: epidemiology; respiratory infections; virology.
© Author(s) (or their employer(s)) 2023. Re-use permitted under CC BY-NC. No commercial re-use. See rights and permissions. Published by BMJ.
Conflict of interest statement
Competing interests: NBH receives grant support from Sanofi, Quidel and speaker compensation from an education grant supported by Genentech. All other coauthors (DAR, LSP, SD, JCS, SK and NKK) have no conflicts of interest relevant to this article to disclose.
Figures


References
Publication types
MeSH terms
Supplementary concepts
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous
