Immunotherapy resistance in non-small-cell lung cancer: From mechanism to clinical strategies
- PMID: 37090727
- PMCID: PMC10115980
- DOI: 10.3389/fimmu.2023.1129465
Immunotherapy resistance in non-small-cell lung cancer: From mechanism to clinical strategies
Abstract
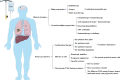
The high primary resistance incidence and unavoidable secondary resistance are the major clinical obstacle to lasting long-term benefits in Non-small-cell lung cancer (NSCLC) patients treated with immunotherapy. The mechanisms of immunotherapy resistance in NSCLC are complex, mainly involving tumor cells and tumor microenvironment (TME) infiltrating immune cells, including TAMs, B cells, NK cells, and T cells. The selection of clinical strategies for NSCLC progression after immunotherapy resistance should depend on the progressive mode. The progression pattern of NSCLC patients after immunotherapy resistance can be divided into oligo-progression and systemic/multiple progression, which should be considered for further treatment selection. In the future, it needs to explore how to optimize the combined therapy and explore strategies to reprogram infiltrating immune cells under various genetic backgrounds of tumor cells and timely reshape TME during antitumor treatments.
Keywords: NSCLC; TME; clinical strategies; immune cells; immunotherapy.
Copyright © 2023 Zhou and Yang.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures


References
-
- Felip E, Altorki N, Zhou C, Csoszi T, Vynnychenko I, Goloborodko O, et al. . Adjuvant atezolizumab after adjuvant chemotherapy in resected stage IB-IIIA non-small-cell lung cancer (IMpower010): a randomised, multicentre, open-label, phase 3 trial. Lancet (2021) 398(10308):1344–57. doi: 10.1016/S0140-6736(21)02098-5 - DOI - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

