Phenobarbital-Based Protocol for Alcohol Withdrawal Syndrome in a Medical ICU: Pre-Post Implementation Study
- PMID: 37091477
- PMCID: PMC10115550
- DOI: 10.1097/CCE.0000000000000898
Phenobarbital-Based Protocol for Alcohol Withdrawal Syndrome in a Medical ICU: Pre-Post Implementation Study
Abstract
We assessed the efficacy and safety of PB compared with benzodiazepine (BZD)-based protocols in treating AWS in MICU.
Design: Single-center, pre-post protocol implementation study.
Setting: The setting is a forty-bed MICU in a tertiary-level academic medical center.
Patients: We included all patients admitted to the MICU with a primary diagnosis of AWS.
Interventions: Intravenous PB 260 mg followed by 130-mg doses every 15-30 minutes as needed up to 15 mg/kg of ideal body weight versus escalating doses of BZD, to achieve a Clinical Institute Withdrawal Assessment Alcohol Scale-Revised score less than 10.
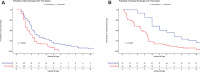
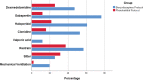
Measurements and main results: ICU and hospital length of stay (LOS), in addition to safety measures were the main outcomes of the study. A total of 102 patients were included, 51 in the PB arm and 51 in the BZD arm. There were no differences in baseline clinical characteristics. Half the patients in each group were admitted with delirium tremens. The use of PB-based protocol was associated with 35% reduction in median ICU LOS (1.5 d [interquartile range, 1.2-2.4 d] vs 2.3 d [1.4-4.8 d]; p = 0.009) and 50% reduction in hospital LOS (3 d [2.7-4 d] vs 6 d [4-10 d]; p < 0.001). After adjustment for comorbidities and clinical factors, PB protocol decreased ICU LOS days by 40% (95% CI; 25.8-53.5%). PB group required fewer adjunctive medications to control symptoms (0.7 [0.5-1] vs 2.5 [2-3]; p < 0.001), less need for intubation (1/51 [2%] vs 10/10 [19.6%]; p = 0.023) and less need for physical restraint (19/51 [37.3%] vs 29/51 [56.9%]; p = 0.047), compared with the BZD group.
Conclusions: A protocol utilizing rapidly escalating doses of PB over a short period is an effective and safe alternative to BZD in treating AWS in MICU.
Keywords: alcohol withdrawal delirium; alcohol withdrawal syndrome; delirium tremens; intensive care units; phenobarbital.
Copyright © 2023 The Authors. Published by Wolters Kluwer Health, Inc. on behalf of the Society of Critical Care Medicine.
Conflict of interest statement
The authors have disclosed that they do not have any potential conflicts of interest.
Figures

Similar articles
-
Effect of early and focused benzodiazepine therapy on length of stay in severe alcohol withdrawal syndrome.Clin Toxicol (Phila). 2019 Jul;57(7):624-627. doi: 10.1080/15563650.2018.1542701. Epub 2019 Feb 7. Clin Toxicol (Phila). 2019. PMID: 30729859
-
Implementation of an ICU-Specific Alcohol Withdrawal Syndrome Management Protocol Reduces the Need for Mechanical Ventilation.Pharmacotherapy. 2018 Jul;38(7):701-713. doi: 10.1002/phar.2127. Epub 2018 Jun 27. Pharmacotherapy. 2018. PMID: 29800507
-
Phenobarbital Versus Benzodiazepines for Alcohol Withdrawal in the Medical Intensive Care Unit (ICU): A Retrospective Cohort Study.J Pharm Pract. 2025 Apr;38(2):231-236. doi: 10.1177/08971900241273144. Epub 2024 Sep 11. J Pharm Pract. 2025. PMID: 39262224
-
Current evidence and clinical utility of phenobarbital for alcohol withdrawal syndrome.Eur J Intern Med. 2023 Jun;112:52-61. doi: 10.1016/j.ejim.2023.03.006. Epub 2023 Mar 21. Eur J Intern Med. 2023. PMID: 36935249
-
Management of Acute Alcohol Withdrawal Syndrome in Critically Ill Patients.Pharmacotherapy. 2016 Jul;36(7):797-822. doi: 10.1002/phar.1770. Epub 2016 Jun 30. Pharmacotherapy. 2016. PMID: 27196747 Review.
Cited by
-
Evaluation of phenobarbital dosing strategies for hospitalized patients with alcohol withdrawal syndrome.Gen Hosp Psychiatry. 2023 Nov-Dec;85:155-162. doi: 10.1016/j.genhosppsych.2023.10.014. Epub 2023 Oct 21. Gen Hosp Psychiatry. 2023. PMID: 37926051 Free PMC article.
-
Trends in alcohol withdrawal management by medical toxicologists in the acute care setting: an analysis of the Toxicology Investigators Consortium (ToxIC) Core Registry, 2016-2022.Alcohol Alcohol. 2025 Jul 16;60(5):agaf047. doi: 10.1093/alcalc/agaf047. Alcohol Alcohol. 2025. PMID: 40736697 Free PMC article.
-
Evaluation of the Use of Phenobarbital and Benzodiazepines in the Management of Alcohol Withdrawal Syndrome in Patients Requiring Neurological/Neurosurgical Critical Care: A Propensity-Matched Analysis.Cureus. 2024 Jun 8;16(6):e61952. doi: 10.7759/cureus.61952. eCollection 2024 Jun. Cureus. 2024. PMID: 38978925 Free PMC article.
-
Phenobarbital Dosing for the Treatment of Alcohol Withdrawal Syndrome: A Review of the Literature.J Pharm Technol. 2024 Aug;40(4):186-193. doi: 10.1177/87551225241249407. Epub 2024 Apr 29. J Pharm Technol. 2024. PMID: 39157637 Free PMC article. Review.
References
-
- Saitz R, O’Malley SS: Pharmacotherapies for alcohol abuse. Withdrawal and treatment. Med Clin North Am 1997; 81:881–907 - PubMed
-
- DeBellis R, Smith BS, Choi S, et al. : Management of delirium tremens. J Intensive Care Med 2005; 20:164–173 - PubMed
-
- Marik P, Mohedin B: Alcohol-related admissions to an inner city hospital intensive care unit. Alcohol Alcoholism 1996; 31:393–396 - PubMed
-
- Sacks JJ, Gonzales KR, Bouchery EE, et al. : 2010 national and state costs of excessive alcohol consumption. Am J Prev Med 2015; 49:e73–e79 - PubMed
LinkOut - more resources
Full Text Sources

