Disease-Modifying Antirheumatic Drug Use and Its Effect on Long-term Opioid Use in Patients With Rheumatoid Arthritis
- PMID: 37092898
- PMCID: PMC10545291
- DOI: 10.1097/RHU.0000000000001972
Disease-Modifying Antirheumatic Drug Use and Its Effect on Long-term Opioid Use in Patients With Rheumatoid Arthritis
Abstract
Background/objectives: The prevalence of chronic pain is high in patients with rheumatoid arthritis (RA), increasing the risk for opioid use. The objective of this study was to assess disease-modifying antirheumatic drug (DMARD) use and its effect on long-term opioid use in patients with RA.
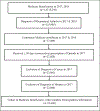
Methods: This cohort study included Medicare beneficiaries with diagnosis of RA who received at least 30-day consecutive prescription of opioids in 2017 (n = 23,608). The patients were grouped into non-DMARD and DMARD users, who were further subdivided into regimens set forth by the American College of Rheumatology. The outcome measured was long-term opioid use in 2018 defined as at least 90-day consecutive prescription of opioids. Dose and duration of opioid use were also assessed. A multivariable model identifying factors associated with non-DMARD use was also performed.
Results: Compared with non-DMARD users, the odds of long-term opioid use were significantly lower among DMARD users (odds ratio, 0.89; 95% confidence interval, 0.83-0.95). All regimens except non-tumor necrosis factor biologic + methotrexate were associated with lower odds of long-term opioid use relative to non-DMARD users. The mean total morphine milligram equivalent, morphine milligram equivalent per day, and total days of opioid use were lower among DMARD users compared with non-DMARD users. Older age, male sex, Black race, psychiatric and medical comorbidities, and not being seen by a rheumatologist were significantly associated with non-DMARD use.
Conclusion: Disease-modifying antirheumatic drug use was associated with lower odds of long-term opioid use among RA patients with baseline opioid prescription. Factors associated with non-DMARD use represent a window of opportunity for intervention to improve pain-related quality of life in patients living with RA.
Copyright © 2023 Wolters Kluwer Health, Inc. All rights reserved.
Conflict of interest statement
The authors declare no conflict of interest.
Similar articles
-
A systematic review of the effectiveness of adalimumab, etanercept and infliximab for the treatment of rheumatoid arthritis in adults and an economic evaluation of their cost-effectiveness.Health Technol Assess. 2006 Nov;10(42):iii-iv, xi-xiii, 1-229. doi: 10.3310/hta10420. Health Technol Assess. 2006. PMID: 17049139
-
Biologics or tofacitinib for rheumatoid arthritis in incomplete responders to methotrexate or other traditional disease-modifying anti-rheumatic drugs: a systematic review and network meta-analysis.Cochrane Database Syst Rev. 2016 May 13;2016(5):CD012183. doi: 10.1002/14651858.CD012183. Cochrane Database Syst Rev. 2016. PMID: 27175934 Free PMC article.
-
Prescription Opioid Use in Older Adults: Trends and Changes in New and Long-Term Use in the United States, 2013-2020.Drugs Aging. 2025 Jul 28. doi: 10.1007/s40266-025-01237-x. Online ahead of print. Drugs Aging. 2025. PMID: 40721568
-
The clinical and cost-effectiveness of anakinra for the treatment of rheumatoid arthritis in adults: a systematic review and economic analysis.Health Technol Assess. 2004 May;8(18):iii-iv, ix-x, 1-105. doi: 10.3310/hta8180. Health Technol Assess. 2004. PMID: 15130461
-
Biologic or tofacitinib monotherapy for rheumatoid arthritis in people with traditional disease-modifying anti-rheumatic drug (DMARD) failure: a Cochrane Systematic Review and network meta-analysis (NMA).Cochrane Database Syst Rev. 2016 Nov 17;11(11):CD012437. doi: 10.1002/14651858.CD012437. Cochrane Database Syst Rev. 2016. PMID: 27855242 Free PMC article.
Cited by
-
Annual trends in pain management modalities in patients with newly diagnosed autoimmune rheumatic diseases in the USA from 2007 to 2021: an administrative claims-based study.Lancet Rheumatol. 2024 Aug;6(8):e518-e527. doi: 10.1016/S2665-9913(24)00120-6. Epub 2024 Jun 27. Lancet Rheumatol. 2024. PMID: 38945137 Free PMC article.
References
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical