Simultaneous resection of colorectal cancer and synchronous liver metastases: what determines the risk of unfavorable outcomes? An international multicenter retrospective cohort study
- PMID: 37093069
- PMCID: PMC10389225
- DOI: 10.1097/JS9.0000000000000068
Simultaneous resection of colorectal cancer and synchronous liver metastases: what determines the risk of unfavorable outcomes? An international multicenter retrospective cohort study
Abstract
Background: The use of a simultaneous resection (SIMR) in patients with synchronous colorectal liver metastases (sCRLM) has increased over the past decades. However, it remains unclear when a SIMR is beneficial and when it should be avoided. The aim of this retrospective cohort study was therefore to compare the outcomes of a SIMR for sCRLM in different settings, and to assess which factors are independently associated with unfavorable outcomes.
Methods: To perform this retrospective cohort study, patients with sCRLM undergoing SIMR (2004-2019) were extracted from an international multicenter database, and their outcomes were compared after stratification according to the type of liver and colorectal resection performed. Factors associated with unfavorable outcomes were identified through multivariable logistic regression.
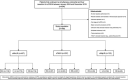
Results: Overall, 766 patients were included, encompassing colorectal resections combined with a major liver resection (n=122), minor liver resection in the anterolateral (n=407), or posterosuperior segments ('Technically major', n=237). Minor and technically major resections, compared to major resections, were more often combined with a rectal resection (29.2 and 36.7 vs. 20.5%, respectively, both P=0.003) and performed fully laparoscopic (22.9 and 23.2 vs. 6.6%, respectively, both P = 0.003). Major and technically major resections, compared to minor resections, were more often associated with intraoperative transfusions (42.9 and 38.8 vs. 20%, respectively, both P = 0.003) and unfavorable incidents (9.6 and 9.8 vs. 3.3%, respectively, both P≤0.063). Major resections were associated, compared to minor and technically major resections, with a higher overall morbidity rate (64.8 vs. 50.4 and 49.4%, respectively, both P≤0.024) and a longer length of stay (12 vs. 10 days, both P≤0.042). American Society of Anesthesiologists grades ≥3 [adjusted odds ratio (aOR): 1.671, P=0.015] and undergoing a major liver resection (aOR: 1.788, P=0.047) were independently associated with an increased risk of severe morbidity, while undergoing a left-sided colectomy was associated with a decreased risk (aOR: 0.574, P=0.013).
Conclusions: SIMR should primarily be reserved for sCRLM patients in whom a minor or technically major liver resection would suffice and those requiring a left-sided colectomy. These findings should be confirmed by randomized studies comparing SIMR with staged resections.
Trial registration: ClinicalTrials.gov NCT05475041.
Copyright © 2023 The Author(s). Published by Wolters Kluwer Health, Inc.
Conflict of interest statement
The authors have no related conflicts of interest to declare.
Sponsorships or competing interests that may be relevant to content are disclosed at the end of this article.
Figures
Similar articles
-
Prescription of Controlled Substances: Benefits and Risks.2025 Jul 6. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan–. 2025 Jul 6. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan–. PMID: 30726003 Free Books & Documents.
-
Comparison of Two Modern Survival Prediction Tools, SORG-MLA and METSSS, in Patients With Symptomatic Long-bone Metastases Who Underwent Local Treatment With Surgery Followed by Radiotherapy and With Radiotherapy Alone.Clin Orthop Relat Res. 2024 Dec 1;482(12):2193-2208. doi: 10.1097/CORR.0000000000003185. Epub 2024 Jul 23. Clin Orthop Relat Res. 2024. PMID: 39051924
-
Simultaneous laparoscopic resection of primary colorectal cancer and associated liver metastases: a systematic review.Tech Coloproctol. 2014 Feb;18(2):129-35. doi: 10.1007/s10151-013-1072-1. Epub 2013 Sep 21. Tech Coloproctol. 2014. PMID: 24057357
-
Staged or simultaneous resection of synchronous liver metastases from colorectal cancer--a systematic review.Colorectal Dis. 2009 Jan;11(1):3-10. doi: 10.1111/j.1463-1318.2008.01625.x. Epub 2008 Jul 11. Colorectal Dis. 2009. PMID: 18637099
-
Intravenous magnesium sulphate and sotalol for prevention of atrial fibrillation after coronary artery bypass surgery: a systematic review and economic evaluation.Health Technol Assess. 2008 Jun;12(28):iii-iv, ix-95. doi: 10.3310/hta12280. Health Technol Assess. 2008. PMID: 18547499
Cited by
-
Surgical Site Infections in Simultaneous Colorectal and Liver Resections for Metastatic Colorectal Adenocarcinoma.Ann Surg Oncol. 2025 Feb;32(2):1043-1053. doi: 10.1245/s10434-024-16489-x. Epub 2024 Nov 21. Ann Surg Oncol. 2025. PMID: 39570297
-
Prognostic factors affecting survival in patients with duodenal adenocarcinoma and isolated liver metastases: a retrospective study.BMC Surg. 2025 Aug 9;25(1):356. doi: 10.1186/s12893-025-03126-x. BMC Surg. 2025. PMID: 40783761 Free PMC article.
-
Immune dynamics shaping pre-metastatic and metastatic niches in liver metastases: from molecular mechanisms to therapeutic strategies.Mol Cancer. 2024 Nov 14;23(1):254. doi: 10.1186/s12943-024-02171-z. Mol Cancer. 2024. PMID: 39543660 Free PMC article. Review.
-
Comparison of textbook outcomes between laparoscopic and open liver resection for patients with hepatocellular carcinoma: a multicenter study.Surg Endosc. 2025 Mar;39(3):2052-2061. doi: 10.1007/s00464-025-11577-9. Epub 2025 Jan 31. Surg Endosc. 2025. PMID: 39890613
-
Predictive risk factors for resection surface-related complications after laparoscopic simultaneous resection of primary colorectal tumor and synchronous liver metastases: a single-center retrospective study.Surg Endosc. 2024 Sep;38(9):5006-5016. doi: 10.1007/s00464-024-10964-y. Epub 2024 Jul 11. Surg Endosc. 2024. PMID: 38992282
References
-
- Sung H, Ferlay J, Siegel RL, et al. . Global Cancer Statistics 2020: GLOBOCAN Estimates of Incidence and Mortality Worldwide for 36 Cancers in 185 Countries. CA Cancer J Clin 2021;71:209–249. - PubMed
-
- Horn SR, Stoltzfus KC, Lehrer EJ, et al. . Epidemiology of liver metastases. Cancer Epidemiol 2020;67:101760. - PubMed
-
- Adam R, de Gramont A, Figueras J, et al. . Managing synchronous liver metastases from colorectal cancer: a multidisciplinary international consensus. Cancer Treat Rev 2015;41:729–741. - PubMed
-
- Lambert LA, Colacchio TA, Barth RJ. Interval hepatic resection of colorectal metastases improves patient selection. Arch Surg 2000;135:473–480. - PubMed
Publication types
MeSH terms
Associated data
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

