Geographical evolutionary pathway of global tuberculosis incidence trends
- PMID: 37095497
- PMCID: PMC10123998
- DOI: 10.1186/s12889-023-15553-7
Geographical evolutionary pathway of global tuberculosis incidence trends
Abstract
Backgrounds: Tuberculosis (TB) remains a serious public health and human development problem, especially in developing countries. Despite the effectiveness of directly observed therapy, short course programs in reducing transmission and progression of TB, poverty reduction and socioeconomic development remain crucial factors in decreasing TB incidence. However, the geographical pathway on the planet is not yet clear.
Objectives: This study was to reconstruct the geographical evolutionary process of TB in 173 countries and territories from 2010 to 2019 to analyze the socioeconomic determinants that impact the global TB epidemic. In addition, the TB incidence in 2030 was predicted.
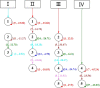
Methods: This study analyses TB incidence data from 173 countries and territories between 2010 and 2019. The Geotree model would be used to reconstruct the geographical evolutionary process of TB, which provides a simplified schema for geo-visualizing the trajectories of TB incidence and their socioeconomic drivers. Additionally, to estimate the future TB incidence in 2030, a multilevel model was utilized in conjunction with the hierarchical nature of the Geotree based on a stratified heterogeneity analysis.
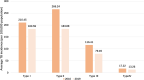
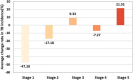
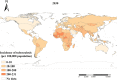
Results: Global TB incidence was found to be associated with the country type and development stages. Between 2010 and 2019, the average TB incidence rate in 173 countries and territories was -27.48%, with marked spatially stratified heterogeneity by country type and development stage. Low-income and lower-middle-income countries were most vulnerable to TB. Upper-middle-income countries experienced a faster decline in TB incidence than high-income countries, and TB incidence generally decreased as the development stage increased, except for the lower-middle development stage in 2019.The highest average rate of decline in TB incidence was observed in the upper-middle development stage of high-income countries, with a reduction of 45.24%. Meanwhile, 37 high-income countries in the high development stage demonstrated an average rate of change of -13.93%. Socioeconomic determinants, including gross domestic product per capita, urbanization rate, and sociodemographic index, were found to inhibit TB incidence. Based on current trends, the predicted average global TB incidence in 2030 is 91.581 per 100,000 population.
Conclusions: The trajectories of the global TB incidence have been reconstructed to formulate targeted public health responses. To eliminate TB, countries at similar development stage can draw on the experiences of countries at higher development stages that are tailored to their unique characteristics. By learning from successful TB control strategies, countries can take strategic steps toward eradicating TB and improving public health outcomes.
Keywords: Geographical evolutionary pathway; Geotree; Stratified heterogeneity; Tuberculosis.
© 2023. The Author(s).
Conflict of interest statement
The authors declare no competing interests.
Figures



Similar articles
-
Migration to middle-income countries and tuberculosis-global policies for global economies.Global Health. 2017 Mar 15;13(1):15. doi: 10.1186/s12992-017-0236-6. Global Health. 2017. PMID: 28298223 Free PMC article.
-
The social determinants of national tuberculosis incidence rates in 116 countries: a longitudinal ecological study between 2005-2015.BMC Public Health. 2023 Feb 15;23(1):337. doi: 10.1186/s12889-023-15213-w. BMC Public Health. 2023. PMID: 36793018 Free PMC article.
-
Modelling and prediction of global non-communicable diseases.BMC Public Health. 2020 Jun 1;20(1):822. doi: 10.1186/s12889-020-08890-4. BMC Public Health. 2020. PMID: 32487173 Free PMC article.
-
Cost of tuberculosis treatment in low- and middle-income countries: systematic review and meta-regression.Int J Tuberc Lung Dis. 2020 Aug 1;24(8):802-810. doi: 10.5588/ijtld.19.0694. Int J Tuberc Lung Dis. 2020. PMID: 32912385
-
Economic and modeling evidence for tuberculosis preventive therapy among people living with HIV: A systematic review and meta-analysis.PLoS Med. 2021 Sep 14;18(9):e1003712. doi: 10.1371/journal.pmed.1003712. eCollection 2021 Sep. PLoS Med. 2021. PMID: 34520463 Free PMC article.
Cited by
-
The Prevalence of Mycobacterium Tuberculosis Infection in Saudi Arabia: A Systematic Review and Meta-analysis.J Epidemiol Glob Health. 2024 Sep;14(3):658-676. doi: 10.1007/s44197-024-00274-w. Epub 2024 Jul 24. J Epidemiol Glob Health. 2024. PMID: 39046668 Free PMC article.
-
Effect of integrating traditional and modern healthcare systems on tuberculosis case detection in Ethiopia: a cluster randomized controlled study.Infect Dis Poverty. 2025 Mar 3;14(1):16. doi: 10.1186/s40249-024-01270-9. Infect Dis Poverty. 2025. PMID: 40025607 Free PMC article. Clinical Trial.
-
Literature Highlights.Int J Tuberc Lung Dis. 2023 Aug 1;27(8):581-583. doi: 10.5588/ijtld.23.9908. Int J Tuberc Lung Dis. 2023. PMID: 37491752 Free PMC article.
-
Development and validation of a diagnostic model for tuberculous meningitis based on laboratory data.Front Cell Infect Microbiol. 2025 May 20;15:1579827. doi: 10.3389/fcimb.2025.1579827. eCollection 2025. Front Cell Infect Microbiol. 2025. PMID: 40463505 Free PMC article.
References
-
- Vos T, Lim SS, Abbafati C, Abbas KM, Abbasi M, Abbasifard M, Abbasi-Kangevari M, Abbastabar H, Abd-Allah F, Abdelalim A, et al. Global burden of 369 diseases and injuries in 204 countries and territories, 1990–2019: a systematic analysis for the Global Burden of Disease Study 2019. The Lancet. 2020;396(10258):1204–1222. doi: 10.1016/S0140-6736(20)30925-9. - DOI - PMC - PubMed
-
- Murray CJ, Ortblad KF, Guinovart C, Lim SS, Wolock TM, Roberts DA, Dansereau EA, Graetz N, Barber RM, Brown JC, et al. Global, regional, and national incidence and mortality for HIV, tuberculosis, and malaria during 1990–2013: a systematic analysis for the Global Burden of Disease Study 2013. Lancet. 2014;384(9947):1005–1070. doi: 10.1016/S0140-6736(14)60844-8. - DOI - PMC - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

