Low back pain of disc, sacroiliac joint, or facet joint origin: a diagnostic accuracy systematic review
- PMID: 37096189
- PMCID: PMC10121397
- DOI: 10.1016/j.eclinm.2023.101960
Low back pain of disc, sacroiliac joint, or facet joint origin: a diagnostic accuracy systematic review
Abstract
Background: The accuracy of diagnostic tests available in primary care to identify the disc, sacroiliac joint, and facet joint as the source of low back pain is uncertain.
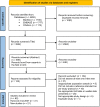
Methods: Systematic review of diagnostic tests available in primary care. MEDLINE, CINAHL, and EMBASE were searched between March 2006 and 25th January 2023. Pairs of reviewers independently screened all studies, extracted data, and assessed risk of bias using QUADAS-2. Pooling was performed for homogenous studies. Positive likelihood ratios (+LR) ≥2 and negative likelihood ratios (-LR) ≤0.5 were considered informative. This review is registered with PROSPERO (CRD42020169828).
Findings: We included 62 studies: 35 investigated the disc, 14 the facet joint, 11 the sacroiliac joint, and 2 investigated all three structures in patients with persistent low back pain. For risk of bias, the domain 'reference standard' scored worst, however approximately half the studies were of low risk of bias for every other domain. For the disc, pooling demonstrated MRI findings of disc degeneration and annular fissure resulted in informative +LRs: 2.53 (95% CI: 1.57-4.07) and 2.88 (95% CI: 2.02-4.10) and -LRs: 0.15 (95% CI: 0.09-0.24) and 0.24 (95% CI: 0.10-0.55) respectively. Pooled results for Modic type 1, Modic type 2, and HIZ on MRI, and centralisation phenomenon yielded informative +LRs: 10.00 (95% CI: 4.20-23.82), 8.03 (95% CI: 3.23-19.97), 3.10 (95% CI: 2.27-4.25), and 3.06 (95% CI: 1.44-6.50) respectively, but uninformative -LRs: 0.84 (95% CI: 0.74-0.96), 0.88 (95% CI: 0.80-0.96), 0.61 (95% CI: 0.48-0.77), and 0.66 (95% CI: 0.52-0.84) respectively. For the facet joint, pooling demonstrated facet joint uptake on SPECT resulted in informative +LRs: 2.80 (95% CI: 1.82-4.31) and -LRs: 0.44 (95% CI: 0.25-0.77). For the sacroiliac joint, a combination of pain provocation tests and absence of midline low back pain resulted in informative +LRs of 2.41 (95% CI: 1.89-3.07) and 2.44 (95% CI: 1.50-3.98) and -LRs of 0.35 (95% CI: 0.12-1.01) and 0.31 (95% CI: 0.21-0.47) respectively. Radionuclide imaging yielded an informative +LR 7.33 (95% CI: 1.42-37.80) but an uninformative -LR 0.74 (95% CI: 0.41-1.34).
Interpretation: There are informative diagnostic tests for the disc, sacroiliac joint, and facet joint (only one test). The evidence suggests a diagnosis may be possible for some patients with low back pain, potentially guiding targeted and specific treatment approaches.
Funding: There was no funding for this study.
Keywords: Diagnosis; Index test; Low back pain; Pathoanatomical; Reference standard.
© 2023 The Author(s).
Conflict of interest statement
We (author team) declare no competing interests.
References
-
- Hoy D., Brooks P., Blyth F., Buchbinder R. The Epidemiology of low back pain. Best Pract Res Clin Rheumatol. 2010;24(6):769–781. - PubMed
-
- Hoy D., March L., Brooks P., et al. The global burden of low back pain: estimates from the Global Burden of Disease 2010 study. Ann Rheum Dis. 2014;73(6):968–974. - PubMed
-
- Dionne C.E., Dunn K.M., Croft P.R., et al. A consensus approach toward the standardization of back pain definitions for use in prevalence studies. Spine (Phila Pa 1976) 2008;33(1):95–103. - PubMed
-
- Oliveira C.B., Maher C.G., Pinto R.Z., et al. Clinical practice guidelines for the management of non-specific low back pain in primary care: an updated overview. Eur Spine J. 2018;27(11):2791–2803. - PubMed
LinkOut - more resources
Full Text Sources