Circulating CD137+ T Cell Levels Are Correlated with Response to Pembrolizumab Treatment in Advanced Head and Neck Cancer Patients
- PMID: 37108276
- PMCID: PMC10138766
- DOI: 10.3390/ijms24087114
Circulating CD137+ T Cell Levels Are Correlated with Response to Pembrolizumab Treatment in Advanced Head and Neck Cancer Patients
Abstract
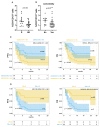
Pembrolizumab, an anti-PD-1 antibody, has been approved as first-line treatment for recurrent or metastatic head and neck squamous cell carcinoma ((R/M) HNSCC). However, only a minority of patients benefit from immunotherapy, which highlights the need to identify novel biomarkers to optimize treatment strategies. CD137+ T cells have been identified as tumour-specific T cells correlated with immunotherapy responses in several solid tumours. In this study, we investigated the role of circulating CD137+ T cells in (R/M) HNSCC patients undergoing pembrolizumab treatment. PBMCs obtained from 40 (R/M) HNSCC patients with a PD-L1 combined positive score (CPS) ≥1 were analysed at baseline via cytofluorimetry for the expression of CD137, and it was found that the percentage of CD3+CD137+ cells is correlated with the clinical benefit rate (CBR), PFS, and OS. The results show that levels of circulating CD137+ T cells are significantly higher in responder patients than in non-responders (p = 0.03). Moreover, patients with CD3+CD137+ percentage ≥1.65% had prolonged OS (p = 0.02) and PFS (p = 0.02). Multivariate analysis, on a combination of biological and clinical parameters, showed that high levels of CD3+CD137+ cells (≥1.65%) and performance status (PS) = 0 are independent prognostic factors of PFS (CD137+ T cells, p = 0.007; PS, p = 0.002) and OS (CD137+ T cells, p = 0.006; PS, p = 0.001). Our results suggest that levels of circulating CD137+ T cells could serve as biomarkers for predicting the response of (R/M) HNSCC patients to pembrolizumab treatment, thus contributing to the success of anti-cancer treatment.
Keywords: 4-1BB; CD137; HNSCC; anti-PD1; immunotherapy.
Conflict of interest statement
The authors declare no conflict of interest. P.M. has and/or had a consultant/advisory role with BMS, Roche Genentech, MSD, Novartis, Amgen, Merck Serono, Pierre Fabre, and Incyte. M.N. reports research grants from Incyte and IPSEN. G.D.A. is a consultant for Roche and MSD.
Figures
Similar articles
-
Pembrolizumab-based first-line treatment for PD-L1-positive, recurrent or metastatic head and neck squamous cell carcinoma: a retrospective analysis.BMC Cancer. 2024 Apr 8;24(1):430. doi: 10.1186/s12885-024-12155-3. BMC Cancer. 2024. PMID: 38589857 Free PMC article.
-
CD137+ and regulatory T cells as independent prognostic factors of survival in advanced non-oncogene addicted NSCLC patients treated with immunotherapy as first-line.J Transl Med. 2024 Apr 3;22(1):329. doi: 10.1186/s12967-024-05142-6. J Transl Med. 2024. PMID: 38570798 Free PMC article.
-
Pembrolizumab in the first-line treatment of advanced head and neck cancer.Expert Rev Anticancer Ther. 2021 Dec;21(12):1321-1331. doi: 10.1080/14737140.2021.1996228. Epub 2021 Nov 2. Expert Rev Anticancer Ther. 2021. PMID: 34689660 Review.
-
Influence of tumor mutational burden, inflammatory gene expression profile, and PD-L1 expression on response to pembrolizumab in head and neck squamous cell carcinoma.J Immunother Cancer. 2022 Feb;10(2):e003026. doi: 10.1136/jitc-2021-003026. J Immunother Cancer. 2022. PMID: 35217573 Free PMC article.
-
The effects of checkpoint inhibition on head and neck squamous cell carcinoma: A systematic review.Oral Oncol. 2019 Mar;90:67-73. doi: 10.1016/j.oraloncology.2019.01.018. Epub 2019 Feb 5. Oral Oncol. 2019. PMID: 30846179
Cited by
-
Breast cancer scoring based on a multiplexed profiling of soluble and cell-associated (immune) markers facilitates the prediction of pembrolizumab therapy.Cancer Cell Int. 2025 Mar 27;25(1):120. doi: 10.1186/s12935-025-03729-7. Cancer Cell Int. 2025. PMID: 40148963 Free PMC article.
-
Immunotherapy in recurrent/metastatic head and neck squamous cell carcinoma: PD-L1 and beyond.Pathologica. 2025 Apr;117(2):73-83. doi: 10.32074/1591-951X-1092. Pathologica. 2025. PMID: 40474706 Free PMC article. Review.
-
Evaluation of immune microenvironment in non-small cell lung carcinoma after neoadjuvant immunotherapy: a case report.Int J Clin Exp Pathol. 2025 Jul 15;18(7):405-413. doi: 10.62347/NCYZ7977. eCollection 2025. Int J Clin Exp Pathol. 2025. PMID: 40814556 Free PMC article.
-
Peripheral immune biomarkers for immune checkpoint inhibition of solid tumours.Clin Transl Med. 2024 Aug;14(8):e1814. doi: 10.1002/ctm2.1814. Clin Transl Med. 2024. PMID: 39162097 Free PMC article. Review.
-
Anti-PD1 therapies induce an early expansion of Ki67+CD8+ T cells in metastatic non-oncogene addicted NSCLC patients.Front Immunol. 2024 Dec 18;15:1483182. doi: 10.3389/fimmu.2024.1483182. eCollection 2024. Front Immunol. 2024. PMID: 39744631 Free PMC article.
References
-
- Jayaram S.C., Muzaffar S.J., Ahmed I., Dhanda J., Paleri V., Mehanna H. Efficacy, outcomes, and complication rates of different surgical and nonsurgical treatment modalities for recurrent/residual oropharyngeal carcinoma: A systematic review and meta-analysis. Head Neck. 2016;38:1855–1861. doi: 10.1002/hed.24531. - DOI - PubMed
-
- Harrington K.J., Ferris R.L., Blumenschein G., Jr., Colevas A.D., Fayette J., Licitra L., Kasper S., Even C., Vokes E.E., Worden F., et al. Nivolumab versus standard, single-agent therapy of investigator’s choice in recurrent or metastatic squamous cell carcinoma of the head and neck (CheckMate 141): Health-related quality-of-life results from a randomised, phase 3 trial. Lancet Oncol. 2017;18:1104–1115. doi: 10.1016/S1470-2045(17)30421-7. - DOI - PMC - PubMed
-
- Seiwert T.Y., Burtness B., Mehra R., Weiss J., Berger R., Eder J.P., Heath K., McClanahan T., Lunceford J., Gause C., et al. Safety and clinical activity of pembrolizumab for treatment of recurrent or metastatic squamous cell carcinoma of the head and neck (KEYNOTE-012): An open-label, multicentre, phase 1b trial. Lancet Oncol. 2016;17:956–965. doi: 10.1016/S1470-2045(16)30066-3. - DOI - PubMed
-
- Ferris R.L., Haddad R., Even C., Tahara M., Dvorkin M., Ciuleanu T.E., Clement P.M., Mesia R., Kutukova S., Zholudeva L., et al. Durvalumab with or without Tremelimumab in Patients with Recurrent or Metastatic Head and Neck Squamous Cell Carcinoma: EAGLE, a Randomized, Open-Label Phase III Study. Ann. Oncol. 2020;31:942–950. doi: 10.1016/j.annonc.2020.04.001. - DOI - PubMed
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Research Materials
Miscellaneous

