Impact of Age and Sex Interaction on Post-Acute Sequelae of COVID-19: An Italian Cohort Study on Adults and Children
- PMID: 37109260
- PMCID: PMC10144783
- DOI: 10.3390/jcm12082924
Impact of Age and Sex Interaction on Post-Acute Sequelae of COVID-19: An Italian Cohort Study on Adults and Children
Abstract
Identifying factors predisposing individuals to post-acute sequelae of COVID-19 (PASC) would allow for the timely treatment of those vulnerable. Attention on the role of sex and age is growing, but published studies have shown mixed results. Our objective was to estimate the effect modification of age on sex as a risk factor for PASC. We analyzed data from two longitudinal prospective cohort studies on adult and pediatric subjects positive to SARS-CoV-2 infection that were enrolled between May 2021 and September 2022. Age classes (≤5, 6-11, 12-50, >50 years) were based on the potential role of sex hormones on inflammatory/immune and autoimmune processes. A total of 452 adults and 925 children were analyzed: 46% were female and 42% were adults. After a median follow-up of 7.8 months (IQR: 5.0 to 9.0), 62% of children and 85% of adults reported at least one symptom. Sex and age alone were not significantly associated to PASC, but their interaction was statistically significant (p-value = 0.024): the risk was higher for males aged 0-5 (females vs. males HR: 0.64, 95% CI: 0.45-0.91, p = 0.012) and for females aged 12-50 (HR: 1.39, 95% CI: 1.04-1.86, p = 0.025), especially those in the cardiovascular, neurological, gastrointestinal and sleep categories. Further research on PASC with regard to sex and age is warranted.
Keywords: COVID-19; age; post-acute sequelae; sex hormones.
Conflict of interest statement
The authors declare that they have no conflict of interest.
Figures
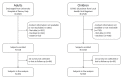


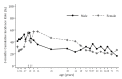
References
-
- Buonsenso D., Munblit D., Pazukhina E., Ricchiuto A., Sinatti D., Zona M., De Matteis A., D’Ilario F., Gentili C., Lanni R., et al. FIMP-Roma. Post-COVID Condition in Adults and Children Living in the Same Household in Italy: A Prospective Cohort Study Using the ISARIC Global Follow-Up Protocol. Front. Pediatr. 2022;10:834875. doi: 10.3389/fped.2022.834875. - DOI - PMC - PubMed
-
- Munblit D., Bobkova P., Spiridonova E., Shikhaleva A., Gamirova A., Blyuss O., Nekliudov N., Bugaeva P., Andreeva M., DunnGalvin A., et al. Sechenov StopCOVID Research Team. Incidence and risk factors for persistent symptoms in adults previously hospitalized for COVID-19. Clin. Exp. Allergy. 2021;51:1107–1120. doi: 10.1111/cea.13997. - DOI - PMC - PubMed
-
- Hirt J., Janiaud P., Gloy V.L., Schandelmaier S., Pereira T.V., Contopoulos-Ioannidis D., Goodman S.N., Ioannidis J., Munkholm K., Hemkens L.G. Robustness of reported postacute health outcomes in children with SARS-CoV-2 infection: A systematic review. Arch. Dis. Child. 2022:1–8. doi: 10.1136/archdischild-2022-324455. - DOI - PMC - PubMed
LinkOut - more resources
Full Text Sources
Miscellaneous

