Clinical Spectrum, Diagnosis, and Treatment Outcome in Individuals With Intravascular Large B-cell Lymphoma Affecting the Nervous System: A Case Series
- PMID: 37139035
- PMCID: PMC10150837
- DOI: 10.7759/cureus.37007
Clinical Spectrum, Diagnosis, and Treatment Outcome in Individuals With Intravascular Large B-cell Lymphoma Affecting the Nervous System: A Case Series
Abstract
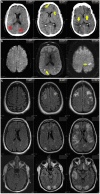
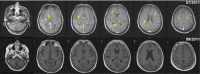
We treated five patients, three females, and two males, with intravascular lymphoma that affected the central or peripheral nervous systems. We reviewed their clinical, laboratory, neuro-imaging, and pathological data and treatment outcomes. The median age of onset was 60 years, with a range of 39 to 69 years. Three patients presented with central nervous system symptoms only, such as confusion, aphasia, seizure, stroke, and ataxia. Three patients presented with systemic lymphoma stage B symptoms, one with peripheral nervous system symptoms, and one with multi-organ failure. Brain imaging revealed white matter lesions, infarcts, hemorrhages, or combinations. Histology showed CD20-positive B-lymphocytes confined to small-size vessels in autopsy or biopsy specimens from the brain or muscle, confirming the diagnosis of intravascular large B-cell lymphoma (IVLBL). The patient with multi-organ failure had diffuse infiltration to the spleen, liver, and kidney. Three patients died within three to four months after the clinical presentation and were diagnosed at autopsy. The other two were diagnosed by biopsy and underwent chemotherapy CHOP-R (cyclophosphamide, hydroxydaunorubicin, Oncovin, and prednisone) or MTX (methotrexate)+Rituximab. The median survival of the chemotherapy patients was 17.5 months, compared to three to four months in those who did not receive chemotherapy. Although IVLBL has distinct pathological features, its clinical presentation can be variable. The patient's best chance for survival depends on the early pathological diagnosis and prompt, aggressive chemotherapy.
Keywords: central nervous system; cerebro-vascular accident (stroke); intravascular large b-cell lymphoma; myopathy; rituximab.
Copyright © 2023, Zhong et al.
Conflict of interest statement
The authors have declared that no competing interests exist.
Figures

Similar articles
-
Rituximab: a review of its use in non-Hodgkin's lymphoma and chronic lymphocytic leukaemia.Drugs. 2003;63(8):803-43. doi: 10.2165/00003495-200363080-00005. Drugs. 2003. PMID: 12662126 Review.
-
[Therapeutic management of central nervous system lymphomas in a single hematological institute].Orv Hetil. 2009 Oct 18;150(42):1937-44. doi: 10.1556/OH.2009.28703. Orv Hetil. 2009. PMID: 19812012 Hungarian.
-
Asian variant of intravascular large B-cell lymphoma: a comparison of clinical features based on involvement of the central nervous system.Korean J Intern Med. 2020 Jul;35(4):946-956. doi: 10.3904/kjim.2018.396. Epub 2019 Nov 25. Korean J Intern Med. 2020. PMID: 31752477 Free PMC article.
-
Diffuse large B-cell lymphoma with involvement of the kidney: outcome and risk of central nervous system relapse.Haematologica. 2011 Jul;96(7):1002-7. doi: 10.3324/haematol.2011.041277. Epub 2011 Apr 12. Haematologica. 2011. PMID: 21486867 Free PMC article.
-
Treatment of relapsed aggressive lymphomas: regimens with and without high-dose therapy and stem cell rescue.Cancer Chemother Pharmacol. 2002 May;49 Suppl 1:S13-20. doi: 10.1007/s00280-002-0447-1. Epub 2002 Apr 12. Cancer Chemother Pharmacol. 2002. PMID: 12042984 Review.
Cited by
-
CT-Imaging Manifestations and Diagnostic Insights in Pulmonary Intravascular Large B-Cell Lymphoma: A Case Series and Literature Review.Cancer Rep (Hoboken). 2025 Mar;8(3):e70159. doi: 10.1002/cnr2.70159. Cancer Rep (Hoboken). 2025. PMID: 40019334 Free PMC article. Review.
-
Case report: Intravascular large B cell lymphoma mimicking acute demyelinating encephalomyelitis after SARS-CoV-2 reinfection: diagnostic value of advanced MRI techniques and the literature review with the assistance of ChatGPT.Front Immunol. 2024 Nov 14;15:1478163. doi: 10.3389/fimmu.2024.1478163. eCollection 2024. Front Immunol. 2024. PMID: 39611151 Free PMC article. Review.
-
Intravascular Lymphoma-Associated Stroke: A Systematic Review of Case Studies.Cureus. 2023 Dec 21;15(12):e50896. doi: 10.7759/cureus.50896. eCollection 2023 Dec. Cureus. 2023. PMID: 38249220 Free PMC article. Review.
References
-
- Presentation and management of intravascular large B-cell lymphoma. Shimada K, Kinoshita T, Naoe T, et al. Lancet Oncol. 2009;10:895–902. - PubMed
-
- Definition, diagnosis, and management of intravascular large B-cell lymphoma: proposals and perspectives from an international consensus meeting. Ponzoni M, Ferreri AJ, Campo E, et al. J Clin Oncol. 2007;25:3168–3173. - PubMed
-
- On the recognition of systematized endotheliomatosis of the cutaneous blood vessels (reticuloendotheliosis? (Article in German) Pfleger L and Tappeiner J. Hautarzt. 1959;10:359–363. - PubMed
-
- Reassessment of malignant "angioendotheliomatosis". Evidence in favor of its reclassification as "intravascular lymphomatosis". Wick M, Mills S, Scheithauer B, et al. Am J Surg Pathol. 1986;10:112–123. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Research Materials
