The clinical manifestation and outcome of COVID-19 in patients with a history of ischemic heart disease; a retrospective case-control study
- PMID: 37149583
- PMCID: PMC10163857
- DOI: 10.1186/s12872-023-03256-1
The clinical manifestation and outcome of COVID-19 in patients with a history of ischemic heart disease; a retrospective case-control study
Abstract
Introduction: Coronary artery disease (CAD) is considered an independent risk factor for COVID-19. However, no study has specifically examined the clinical manifestations and outcomes of COVID-19 in patients with ischemic heart disease (IHD).
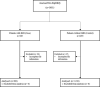
Methods: In a retrospective case-control study between 20 March 2020 to 20 May 2020, the medical record of 1611 patients with laboratory-confirmed SARS-CoV-2 infection was reviewed. IHD was defined as a history of an abnormal coronary angiography, coronary angioplasty, coronary artery bypass graft (CABG), or chronic stable angina. Demographic data, past medical history, drug history, symptoms, vital signs, laboratory findings, outcome, and death were investigated from medical records.
Results: 1518 Patients (882 men (58.1%)) with a mean age of 59.3 ± 15.5 years were included in the study. Patients with IHD (n = 300) were significantly less likely to have fever (OR: 0.170, 95% CI: 0.34-0.81, P < 0.001), and chills (OR: 0.74, 95% CI: 0.45-0.91, P < 0.001). Patients with IHD were 1.57 times more likely to have hypoxia (83.3% vs. 76%, OR: 1.57, 95% CI: 1.13-2.19, P = 0.007). There was no significant difference in terms of WBC, platelets, lymphocytes, LDH, AST, ALT, and CRP between the two groups (P > 0.05). After adjusting for demographic characteristics, comorbidities and vital signs, the risk factors for mortality of these patients were older age (OR: 1.04 and 1.07) and cancer (OR: 1.03, and 1.11) in both groups. In addition, in the patients without IHD, diabetes mellitus (OR: 1.50), CKD (OR: 1.21) and chronic respiratory diseases (OR: 1.48) have increased the odds of mortality. In addition, the use of anticoagulants (OR: 2.77) and calcium channel blockers (OR: 2.00) has increased the odds of mortality in two groups.
Conclusion: In comparison with non-IHD, the symptoms of SARS-CoV-2 infection such as fever, chills and diarrhea were less common among patients with a history of IHD. Also, older age, and comorbidities (including cancer, diabetes mellitus, CKD and chronic obstructive respiratory diseases) have been associated with a higher risk of mortality in patients with IHD. In addition, the use of anticoagulants and calcium channel blockers has increased the chance of death in two groups without and with IHD.
Keywords: COVID-19; Clinical manifestation; Ischemic heart disease.
© 2023. The Author(s).
Conflict of interest statement
The authors declare that they have no competing interests
Similar articles
-
Reconvalescent plasma/camostat mesylate in early SARS-CoV-2 Q-PCR positive high-risk individuals (RES-Q-HR): a structured summary of a study protocol for a randomized controlled trial.Trials. 2021 May 17;22(1):343. doi: 10.1186/s13063-021-05181-0. Trials. 2021. PMID: 34001215 Free PMC article.
-
Outcomes of Covid-19 among patients with ischemic heart disease: A propensity matched analysis.Heart Lung. 2024 Nov-Dec;68:291-297. doi: 10.1016/j.hrtlng.2024.08.010. Epub 2024 Aug 24. Heart Lung. 2024. PMID: 39181103
-
Coronavirus Disease 2019 and Chronic Kidney Disease - A Clinical Observational Study.Saudi J Kidney Dis Transpl. 2021 May-Jun;32(3):744-753. doi: 10.4103/1319-2442.336770. Saudi J Kidney Dis Transpl. 2021. PMID: 35102917
-
Management of Hypertension in Patients with Ischemic Heart Disease.Curr Cardiol Rep. 2015 Dec;17(12):119. doi: 10.1007/s11886-015-0662-0. Curr Cardiol Rep. 2015. PMID: 26482762 Review.
-
API expert consensus document on management of ischemic heart disease.J Assoc Physicians India. 2006 Jun;54:469-80. J Assoc Physicians India. 2006. PMID: 16909697 Review.
Cited by
-
Rhabdomyolysis secondary to COVID-19 infection and vaccination: a review of literature.Front Med (Lausanne). 2024 Nov 20;11:1460676. doi: 10.3389/fmed.2024.1460676. eCollection 2024. Front Med (Lausanne). 2024. PMID: 39635585 Free PMC article. Review.
References
-
- Adhikari SP, Meng S, Wu Y-J, Mao Y-P, Ye R-X, Wang Q-Z, et al. Epidemiology, causes, clinical manifestation and diagnosis, prevention and control of coronavirus disease (COVID-19) during the early outbreak period: a scoping review. Infect Dis poverty. 2020;9(1):1–12. doi: 10.1186/s40249-020-00646-x. - DOI - PMC - PubMed
-
- Zhu N, Zhang D, Wang W, Li X, Yang B, Song J, et al. A novel coronavirus from patients with pneumonia in China, 2019. New England Journal of Medicine; 2020.
-
- WHO. 2020 [Available from: https://covid19.who.int/.
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Research Materials
Miscellaneous