Risk stratification based on acute-on-chronic liver failure in cirrhotic patients hospitalized for acute variceal bleeding
- PMID: 37173645
- PMCID: PMC10176818
- DOI: 10.1186/s12876-023-02768-6
Risk stratification based on acute-on-chronic liver failure in cirrhotic patients hospitalized for acute variceal bleeding
Abstract
Background and aims: Acute variceal bleeding (AVB) is a life-threatening complication of cirrhosis. Acute-on-chronic liver failure (ACLF) is a syndrome characterized by acute decompensation of cirrhosis, multiple organ failures and high short-term mortality. This study aimed to evaluate the role of ACLF in the risk stratification of cirrhotic patients with AVB.
Methods: Prospective data of 335 cirrhotic patients hospitalized for AVB were retrospectively extracted from Medical Information Mart for Intensive Care (MIMIC)-IV database. ACLF was defined by European Association for the Study of Liver-Chronic Liver Failure Consortium and diagnosed/graded with chronic liver failure-organ failure (CLIF-OF) score. Cox-proportional hazards regression analysis was performed to identify the risk factors for 6-week morality in AVB patients. Discrimination and calibration of prognostic scores were evaluated by plotting the receiver operating characteristics (ROC) curve and calibration curve, respectively. Overall performance was assessed by calculating the Brier score and R2 value.
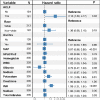
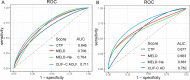
Results: A total of 181 (54.0%) patients were diagnosed with ACLF (grade 1: 18.2%, grade 2: 33.7%, grade 3: 48.1%) at admission. The 6-week mortality in patients with ACLF was significantly higher than that in patients without ACLF (43.6% vs. 8.4%, P < 0.001) and increased in line with the severity of ACLF (22.5%, 34.2% and 63.8% for ACLF grade 1, 2 and 3, P < 0.001). In multivariate analysis, presence of ACLF remained as an independent risk factor for 6-week mortality after adjusting for confounding factors (HR = 2.12, P = 0.03). The discrimination, calibration and overall performance of CLIF-C ACLF and CLIF-C AD were superior to the traditional prognostic scores (CTP, MELD and MELD-Na) in the prediction of 6-week mortality of patients with and without ACLF, respectively.
Conclusion: The prognosis of cirrhotic patients with AVB is poor when accompanied by ACLF. ACLF at admission is an independent predictor for the 6-week mortality in cirrhotic patients with AVB. CLIF-C ACLF and CLIF-C AD are the best prognostic scores in AVB patients with and without ACLF, respectively, and can be used for the risk stratification of these two distinct entities.
Keywords: Acute variceal bleeding; Acute-on-chronic liver failure; Prognosis; Risk stratification.
© 2023. The Author(s).
Conflict of interest statement
The authors declare that they have no competing interests.
Figures


References
-
- Fortune BE, Garcia-Tsao G, Ciarleglio M, Deng Y, Fallon MB, Sigal S, et al. Child-Turcotte-Pugh Class is best at stratifying risk in variceal hemorrhage: analysis of a U.S. multi-center prospective study. J Clin Gastroenterol. 2017;51(5):446–53. doi: 10.1097/MCG.0000000000000733. - DOI - PMC - PubMed
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Research Materials

