Breast carcinoma detection in ex vivo fresh human breast surgical specimens using a fast slide-free confocal microscopy scanner: HIBISCUSS project
- PMID: 37178160
- PMCID: PMC10182737
- DOI: 10.1093/bjsopen/zrad046
Breast carcinoma detection in ex vivo fresh human breast surgical specimens using a fast slide-free confocal microscopy scanner: HIBISCUSS project
Abstract
Background: New generation ultra-fast fluorescence confocal microscopy allows the ex vivo intraoperative analysis of fresh tissue. The High resolution Imaging for Breast carcInoma detection in ex vivo Specimens after breast Conserving sUrgery by hiStolog Scanner (HIBISCUSS) project aimed to develop an online learning program to recognize the main breast tissue features on ultra-fast fluorescence confocal microscopy images and to evaluate the performance of surgeons and pathologists in diagnosing cancerous and non-cancerous breast tissue in ultra-fast fluorescence confocal microscopy images.
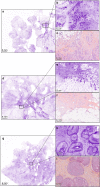
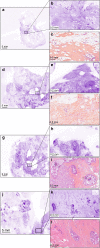
Methods: Patients who underwent conservative surgery or mastectomy for breast carcinoma (invasive or in situ lesions) were included. The fresh specimens were stained with a fluorescent dye and imaged using a large field-of-view (20 cm2) ultra-fast fluorescence confocal microscope.
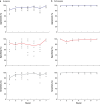
Results: One hundred and eighty-one patients were included. The images from 55 patients were annotated to generate learning sheets and images from 126 patients were blindly interpreted by seven surgeons and two pathologists. The time for tissue processing and ultra-fast fluorescence confocal microscopy imaging was between 8 and 10 min. The training program was composed of 110 images divided into nine learning sessions. The final database for blind performance assessment comprised 300 images. The mean duration for one training session and one performance round was 17 and 27 min respectively. The performance of pathologists was almost perfect with 99.6 per cent (standard deviation (s.d.) 5.4 per cent) accuracy. Surgeons' accuracy significantly increased (P = 0.001) from 83 per cent (s.d. 8.4 per cent) in round 1 to 98 per cent (s.d. 4.1 per cent) in round 7 as well as the sensitivity (P = 0.004). Specificity increased without significance from 84 per cent (s.d. 16.7 per cent) in round 1 to 87 per cent (s.d. 16.4 per cent) in round 7 (P = 0.060).
Conclusion: Pathologists and surgeons showed a short learning curve in differentiating breast cancer from non-cancerous tissue in ultra-fast fluorescence confocal microscopy images. Performance assessment for both specialties supports ultra-fast fluorescence confocal microscopy evaluation for intraoperative management.
Registration number: NCT04976556 (http://www.clinicaltrials.gov).
© The Author(s) 2023. Published by Oxford University Press on behalf of BJS Society Ltd.
Figures


References
-
- Veronesi U, Cascinelli N, Mariani L, Greco M, Saccozzi R, Luini Aet al. . Twenty-year follow-up of a randomized study comparing breast-conserving surgery with radical mastectomy for early breast cancer. N Engl J Med 2002;347:1227–1232 - PubMed
-
- Kouzminova NB, Aggarwal S, Aggarwal A, Allo MD, Lin AY. Impact of initial surgical margins and residual cancer upon re-excision on outcome of patients with localized breast cancer. Am J Surg 2009;198:771–780 - PubMed
-
- Houssami N, Macaskill P, Marinovich ML, Dixon JM, Irwig L, Brennan MEet al. . Meta-analysis of the impact of surgical margins on local recurrence in women with early-stage invasive breast cancer treated with breast-conserving therapy. Eur J Cancer 2010;46:3219–3232 - PubMed
-
- Morrow M, Van Zee KJ, Solin LJ, Houssami N, Chavez-MacGregor M, Harris JRet al. . Society of Surgical Oncology-American Society for Radiation Oncology-American Society of Clinical Oncology Consensus Guideline on margins for breast-conserving surgery with whole-breast irradiation in ductal carcinoma in situ. Ann Surg Oncol 2016;23:3801–3810 - PMC - PubMed
-
- McCahill LE, Single R, Ratliff J, Sheehey-Jones J, Gray A, James T. Local recurrence after partial mastectomy: relation to initial surgical margins. Am J Surg 2011;201:374–378 - PubMed
Publication types
MeSH terms
Associated data
LinkOut - more resources
Full Text Sources
Medical

