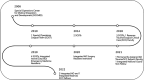
The 16-year evolution of a military-civilian partnership: The University of Alabama at Birmingham experience
- PMID: 37184467
- PMCID: PMC10389557
- DOI: 10.1097/TA.0000000000004051
The 16-year evolution of a military-civilian partnership: The University of Alabama at Birmingham experience
Abstract
Background: At the University of Alabama at Birmingham (UAB), a multi-tiered military-civilian partnership (MCP) has evolved since 2006. We aimed to outline this model to facilitate potential replication nationally.
Methods: We performed a comprehensive review of the partnership between UAB, the United States Air Force Special Operations Command, and the Department of Defense (DoD) reviewing key documents and conducting interviews with providers. As a purely descriptive study, this project did not involve any patient data acquisition or analysis and therefore was exempt from institutional review board approval per institutional policy.
Results: At the time of this review, six core programs existed targeting training, clinical proficiency, and research. Training: (1) The Special Operations Center for Medical Integration and Development trains up to 144 combat medics yearly. (2) UAB trains one integrated military Surgery resident yearly with two additional civilian-sponsored military residents in Emergency Medicine. (3) UAB's Surgical Critical Care Fellowship had one National Guard member with two incoming Active-Duty, one Reservist and one prior service member in August 2022. Clinical Proficiency: (4) UAB hosts four permanently assigned United States Air Force Special Operations Command Special Operations Surgical Teams composed of general surgeons, anesthesiologists, certified registered nurse anesthetists, surgical technologists, emergency physicians, critical care registered nurses, and respiratory therapists totaling 24 permanently assigned active-duty health care professionals. (5) In addition, two fellowship-trained Air Force Trauma Critical Care Surgeons, one Active-Duty and one Reservist, are permanently assigned to UAB. These clinicians participate fully and independently in the routine care of patients alongside their civilian counterparts. Research: (6) UAB's Division of Trauma and Acute Care Surgery is currently conducting nine DoD-funded research projects totaling $6,482,790, and four research projects with military relevance funded by other agencies totaling $15,357,191.
Conclusion: The collaboration between UAB and various elements within the DoD illustrates a comprehensive approach to MCP. Replicating appropriate components of this model nationally may aid in the development of a truly integrated trauma system best prepared for the challenges of the future.
Level of evidence: Economic and Value-based Evaluations; Level IV.
Copyright © 2023 Written work prepared by employees of the Federal Government as part of their official duties is, under the U.S. Copyright Act, a “work of the United States Government” for which copyright protection under Title 17 of the United States Code is not available. As such, copyright does not extend to the contributions of employees of the Federal Government.
Figures
References
-
- Feliciano DV. Contributions of military surgeons to the management of vascular trauma. J Trauma Acute Care Surg. 2017;83(5):777–783. - PubMed
-
- Carmichael SP, Mowery NT, Martin RS, Meredith JW. Management of Acute Trauma. In: Townsend CM, Beauchamp RD, Evers BM, Mattox KL. Sabiston Textbook of Surgery: The Biological Basis of Modern Surgical Practice. Elsevier Health Sciences; 2021;387–388.
-
- Schwab WC. Winds of war: enhancing civilian and military partnerships to assure readiness: white paper. J Am Coll Surg. 2015;221(2):235–254. - PubMed
-
- Cannon JW, Gross KR, Rasmussen TE. Combating the peacetime effect in military medicine. 2021;156(1):5–6. - PubMed
-
- Knudson MM. A perfect storm: 2019 scudder oration on trauma. J Am Coll Surg. 2020;230(3):269–282. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Research Materials
Miscellaneous