Predictive value of multiple variable models including nutritional risk score (NRS 2002) on mortality and length of stay of patients with covid-19 infections. The INCOVO study
- PMID: 37202068
- PMCID: PMC10085867
- DOI: 10.1016/j.clnesp.2023.04.001
Predictive value of multiple variable models including nutritional risk score (NRS 2002) on mortality and length of stay of patients with covid-19 infections. The INCOVO study
Abstract
Background and aims: This study aimed at evaluating associations between nutritional status and outcomes in patients with Covid-19 and to identify statistical models including nutritional parameters associated with in-hospital mortality and length of stay.
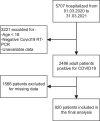
Methods: Data of 5707 adult patients hospitalized in the University Hospital of Lausanne between March 2020 and March 2021 were screened retrospectively 920 patients (35% female) with confirmed Covid-19 and complete data including nutritional risk score (NRS 2002), were included. This cohort was divided into three subgroups: NRS <3: no risk of malnutrition; NRS ≥3 to <5: moderate risk malnutrition; and NRS ≥5: severe risk of malnutrition. The primary outcome was the percentage of in-hospital deaths in the different NRS subgroups. The secondary outcomes were the length of hospital stay (LOS), the percentage of admissions to intensive care units (ICU), and the length of stay in the ICU (ILOS). Logistic regression was performed to identify risk factors associated with in-hospital mortality and hospital stay. Multivariate clinical-biological models were developed to study predictions of mortality and very long length of stay.
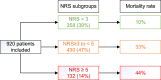
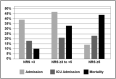
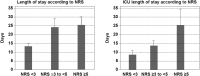
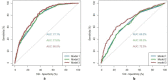
Results: The mean age of the cohort was 69.7 years. The death rate was 4 times higher in the subgroup with a NRS ≥ 5 (44%), and 3 times higher with a NRS ≥ 3 to <5 (33%) compared to the patients with a NRS<3 (10%) (p < 0.001). LOS was significantly higher in the NRS ≥ 5 and NRS ≥ 3 to <5 subgroups (26.0 days; CI [21; 30.9]; and 24.9; CI [22.5; 27.1] respectively) versus 13.4; CI [12; 14.8] for NRS<3 (p < 0.001). The mean ILOS was significantly higher in the NRS ≥ 5 (5.9 days; versus 2.8 for NRS ≥ 3 to <5, and 1.58 for NRS<3 (p < 0.001)). In logistic regression, NRS ≥ 3 was significantly associated with the risk of mortality (OR: 4.8; CI [3.3; 7.1]; p < 0.001) and very long in-hospital stay (>12 days) (OR: 2.5; CI [1.9; 3.3]; p < 0.001). Statistical models that included a NRS ≥ 3 and albumin revealed to be strong predictors for mortality and LOS (area under the curve 0.800 and 0.715).
Conclusion: NRS was found to be an independent risk factor for in-hospital death and LOS in hospitalized Covid-19 patients. Patients with a NRS ≥ 5 had a significant increase in ILOS and mortality. Statistical models including NRS are strong predictors for an increased risk of death and LOS.
Keywords: COVID-19; Length of hospital stay; Mortality; Nutritional risk score (NRS); Nutritional status; Sars-CoV-2.
Copyright © 2023 The Author(s). Published by Elsevier Ltd.. All rights reserved.
Conflict of interest statement
Declaration of competing interest The authors declare no conflict of interest.
Figures
References
-
- Palaiodimos L., Kokkinidis D.G., Li W., Karamanis D., Ognibene J., Arora S., et al. Severe obesity, increasing age and male sex are independently associated with worse in-hospital outcomes, and higher in-hospital mortality, in a cohort of patients with COVID-19 in the Bronx, New York. Metabolism. 2020;108 - PMC - PubMed
-
- Qu G., Li X., Hu L., Jiang G. An imperative need for research on the role of environmental factors in transmission of novel coronavirus (COVID-19) Environ Sci Technol. 2020;54(7):3730–3732. - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

