Cytomegalovirus High-risk Kidney Transplant Recipients Show No Difference in Long-term Outcomes Following Preemptive Versus Prophylactic Management
- PMID: 37211633
- PMCID: PMC10358437
- DOI: 10.1097/TP.0000000000004615
Cytomegalovirus High-risk Kidney Transplant Recipients Show No Difference in Long-term Outcomes Following Preemptive Versus Prophylactic Management
Abstract
Background: Following kidney transplantation (KT), cytomegalovirus (CMV) infection remains an important challenge. Both prophylactic and preemptive antiviral protocols are used for CMV high-risk kidney recipients (donor seropositive/recipient seronegative; D+/R-). We performed a nationwide comparison of the 2 strategies in de novo D+/R- KT recipients accessing long-term outcomes.
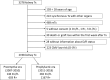
Methods: A nationwide retrospective study was conducted from 2007 to 2018, with follow-up until February 1, 2022. All adult D+/R- and R+ KT recipients were included. During the first 4 y, D+/R- recipients were managed preemptively, changing to 6 mo of valganciclovir prophylaxis from 2011. To adjust for the 2 time eras, de novo intermediate-risk (R+) recipients, who received preemptive CMV therapy throughout the study period, served as longitudinal controls for possible confounders.
Results: A total of 2198 KT recipients (D+/R-, n = 428; R+, n = 1770) were included with a median follow-up of 9.4 (range, 3.1-15.1) y. As expected, a greater proportion experienced a CMV infection in the preemptive era compared with the prophylactic era and with a shorter time from KT to CMV infection ( P < 0.001). However, there were no differences in long-term outcomes such as patient death (47/146 [32%] versus 57/282 [20%]; P = 0.3), graft loss (64/146 [44%] versus 71/282 [25%]; P = 0.5), or death censored graft loss (26/146 [18%] versus 26/282 [9%]; P = 0.9) in the preemptive versus prophylactic era. Long-term outcomes in R+ recipients showed no signs of sequential era-related bias.
Conclusions: There were no significant differences in relevant long-term outcomes between preemptive and prophylactic CMV-preventive strategies in D+/R- kidney transplant recipients.
Copyright © 2023 The Author(s). Published by Wolters Kluwer Health, Inc.
Conflict of interest statement
The authors declare no funding or conflicts of interest.
Figures



Comment in
-
The Best Method for CMV Prevention in High-risk Kidney Transplant Recipients? Either, per National Norwegian Transplant Database: Commentary on Blom et al, Cytomegalovirus High-risk Kidney Transplant Recipients Show No Difference in Long-term Outcomes Following Preemptive Versus Prophylactic Management.Transplantation. 2023 Aug 1;107(8):1671-1672. doi: 10.1097/TP.0000000000004616. Epub 2023 May 22. Transplantation. 2023. PMID: 37211634 No abstract available.
References
-
- Sagedal S, Hartmann A, Nordal KP, et al. . Impact of early cytomegalovirus infection and disease on long-term recipient and kidney graft survival. Kidney Int. 2004;66:329–337. - PubMed
-
- Smedbråten YV, Sagedal S, Leivestad T, et al. . The impact of early cytomegalovirus infection after kidney transplantation on long-term graft and patient survival. Clin Transplant. 2014;28:120–126. - PubMed
-
- Reischig T, Kacer M, Hruba P, et al. . The impact of viral load and time to onset of cytomegalovirus replication on long-term graft survival after kidney transplantation. Antivir Ther. 2017;22:503–513. - PubMed
-
- Sagedal S, Nordal KP, Hartmann A, et al. . A prospective study of the natural course of cytomegalovirus infection and disease in renal allograft recipients. Transplantation. 2000;70:1166–1174. - PubMed
-
- Toupance O, Bouedjoro-Camus MC, Carquin J, et al. . Cytomegalovirus-related disease and risk of acute rejection in renal transplant recipients: a cohort study with case-control analyses. Transpl Int. 2000;13:413–419. - PubMed
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Research Materials

