Progression of pulmonary cysts in Birt-Hogg-Dubé syndrome: longitudinal thoracic computed tomography study with quantitative assessment
- PMID: 37221571
- PMCID: PMC10207738
- DOI: 10.1186/s12890-023-02483-8
Progression of pulmonary cysts in Birt-Hogg-Dubé syndrome: longitudinal thoracic computed tomography study with quantitative assessment
Abstract
Background: Birt-Hogg-Dubé (BHD) syndrome is a rare autosomal dominant disorder characterized by fibrofolliculomas, renal tumors, pulmonary cysts, and recurrent pneumothorax. Pulmonary cysts are the cause of recurrent pneumothorax, which is one of the most important factors influencing patient quality of life. It is unknown whether pulmonary cysts progress with time or influence pulmonary function in patients with BHD syndrome. This study investigated whether pulmonary cysts progress during long-term follow-up (FU) by using thoracic computed tomography (CT) and whether pulmonary function declines during FU. We also evaluated risk factors for pneumothorax in patients with BHD during FU.
Methods: Our retrospective cohort included 43 patients with BHD (25 women; mean age, 54.2 ± 11.7 years). We evaluated whether cysts progress by visual assessment and quantitative volume analysis using initial and serial thoracic CT. The visual assessment included the size, location, number, shape, distribution, presence of a visible wall, fissural or subpleural cysts, and air-cuff signs. In CT data obtained from a 1-mm section from 17 patients, the quantitative assessment was performed by measuring the volume of the low attenuation area using in-house software. We evaluated whether the pulmonary function declined with time on serial pulmonary function tests (PFT). Risk factors for pneumothorax were analyzed using multiple regression analysis.
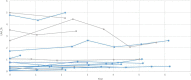
Results: On visual assessment, the largest cyst in the right lung showed a significant interval increase in size (1.0 mm/year, p = 0.0015; 95% confidence interval [CI], 0.42-1.64) between the initial and final CT, and the largest cyst in the left lung also showed significant interval increase in size (0.8 mm/year, p < 0.001, 95% CI; -0.49-1.09). On quantitative assessment, cysts had a tendency to gradually increase in size. In 33 patients with available PFT data, FEV1pred%, FEV1/FVC, and VCpred% showed a statistically significant decrease with time (p < 0.0001 for each). A family history of pneumothorax was a risk factor for the development of pneumothorax.
Conclusions: The size of pulmonary cysts progressed over time in longitudinal follow-up thoracic CT in patients with BHD, and pulmonary function had slightly deteriorated by longitudinal follow-up PFT.
Keywords: Birt-Hogg-Dubé (BHD) syndrome; Computed tomography; Folliculin gene mutation; Pneumothorax; Pulmonary cyst; Pulmonary function test.
© 2023. The Author(s).
Conflict of interest statement
The authors declare that they have no conflicts of interest related to this study.
Figures


References
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

