Mortality data from omission of early thromboprophylaxis in critically ill patients highlights the importance of an individualised diagnosis-related approach
- PMID: 37221578
- PMCID: PMC10207702
- DOI: 10.1186/s12959-023-00499-y
Mortality data from omission of early thromboprophylaxis in critically ill patients highlights the importance of an individualised diagnosis-related approach
Abstract
Background: Venous thromboembolism (VTE) prophylaxis is effective in reducing VTE events, however, its impact on mortality is unclear. We examined the association between omission of VTE prophylaxis within the first 24 h after intensive care unit (ICU) admission and hospital mortality.
Methods: Retrospective analysis of prospectively collected data from the Australian New Zealand Intensive Care Society Adult Patient Database. Data were obtained for adult admissions between 2009 and 2020. Mixed effects logistic regression models were used to evaluate the association between omission of early VTE prophylaxis and hospital mortality.
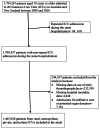
Results: Of the 1,465,020 ICU admissions, 107,486 (7.3%) did not receive any form of VTE prophylaxis within the first 24 h after ICU admission without documented contraindication. Omission of early VTE prophylaxis was independently associated with 35% increased odds of in-hospital mortality (odds ratios (OR): 1.35; 95% CI: 1.31-1.41). The associations between omission of early VTE prophylaxis and mortality varied by admission diagnosis. In patients diagnosed with stroke (OR: 1.26, 95% CI: 1.05-1.52), cardiac arrest (OR: 1.85, 95% CI: 1.65-2.07) or intracerebral haemorrhage (OR: 1.48, 95% CI: 1.19-1.84), omission of VTE prophylaxis was associated with increased risk of mortality, but not in patients diagnosed with subarachnoid haemorrhage or head injury.
Conclusions: Omission of VTE prophylaxis within the first 24 h after ICU admission was independently associated with increased risk of mortality that varied by admission diagnosis. Consideration of early thromboprophylaxis may be required for patients with stroke, cardiac arrest and intracerebral haemorrhage but not in those with subarachnoid haemorrhage or head injury. The findings highlight the importance of individualised diagnosis-related thromboprophylaxis benefit-harm assessments.
Keywords: Critically ill; Intensive care unit; Mortality; Thromboprophylaxis; Venous thromboembolism; VTE.
© 2023. The Author(s).
Conflict of interest statement
All authors declare no financial or non-financial competing interests with regards to the submitted work.
Figures
Similar articles
-
Trends and risk factors for omission of early thromboprophylaxis in Australian and New Zealand ICUs between 2009 and 2020.Intensive Care Med. 2022 May;48(5):590-598. doi: 10.1007/s00134-022-06672-7. Epub 2022 Apr 1. Intensive Care Med. 2022. PMID: 35362763 Free PMC article.
-
Omission of early thromboprophylaxis and mortality in critically ill patients: a multicenter registry study.Chest. 2011 Dec;140(6):1436-46. doi: 10.1378/chest.11-1444. Epub 2011 Sep 22. Chest. 2011. PMID: 21940768
-
Venous thromboembolism prophylaxis in the critically ill: a point prevalence survey of current practice in Australian and New Zealand intensive care units.Crit Care Resusc. 2010 Mar;12(1):9-15. Crit Care Resusc. 2010. PMID: 20196708
-
Venous Thromboembolism Prophylaxis: A Narrative Review With a Focus on the High-Risk Critically Ill Patient.J Intensive Care Med. 2019 Nov-Dec;34(11-12):877-888. doi: 10.1177/0885066618796486. Epub 2018 Aug 30. J Intensive Care Med. 2019. PMID: 30165770 Review.
-
Deep Vein Thrombosis in Intensive Care.Adv Exp Med Biol. 2017;906:167-181. doi: 10.1007/5584_2016_114. Adv Exp Med Biol. 2017. PMID: 27628009 Review.
Cited by
-
Venous Thromboembolism Prophylaxis in the Neurocritically Ill Population.J Clin Med. 2025 Jun 22;14(13):4434. doi: 10.3390/jcm14134434. J Clin Med. 2025. PMID: 40648808 Free PMC article. Review.
-
Risk, incidence and predictors of venous thromboembolism among patients attending the emergency department of tertiary care hospitals in Addis Ababa city, Ethiopia: a multicentre prospective study.BMJ Open. 2025 Jan 14;15(1):e091364. doi: 10.1136/bmjopen-2024-091364. BMJ Open. 2025. PMID: 39809560 Free PMC article.
-
Venous thromboprophylaxis in the ICU: navigating evidence, risk, and practice gaps.Intensive Care Med. 2025 Aug;51(8):1508-1510. doi: 10.1007/s00134-025-08009-6. Epub 2025 Jul 16. Intensive Care Med. 2025. PMID: 40668233 No abstract available.
-
Venous Thromboembolism Risk and Prophylaxis in the Acute Hospital Care Settings in Oman: A National Multicenter Cross-sectional Study.Oman Med J. 2024 Mar 31;39(2):e614. doi: 10.5001/omj.2024.63. eCollection 2024 Mar. Oman Med J. 2024. PMID: 38988795 Free PMC article.
References
LinkOut - more resources
Full Text Sources