Influence of hyperthermic intraperitoneal chemotherapy on renal blood perfusion
- PMID: 37222835
- PMCID: PMC10209305
- DOI: 10.1007/s00423-023-02948-8
Influence of hyperthermic intraperitoneal chemotherapy on renal blood perfusion
Abstract
Purpose: Hyperthermic intraperitoneal chemotherapy (HIPEC) is accompanied with an increased risk of acute kidney injury (AKI). Whether AKI is induced by chemotoxicity or hyperthermia-related changes in renal perfusion remains controversial. The influence of HIPEC on renal perfusion has not been evaluated in patients yet.
Methods: Renal blood perfusion was assessed in ten patients treated with HIPEC by intraoperative renal Doppler pulse-wave ultrasound. Ultrasound (US) examinations were performed pre-, intra-, and postoperative with analyses of time-velocity curves. Patient demographics, surgical details, and data regarding renal function were recorded perioperatively. For evaluation of renal Doppler US to predict AKI, patients were divided in two groups with (AKI +) and without (AKI -) kidney injury.
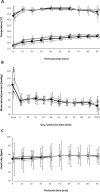
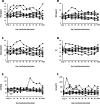
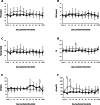
Results: Throughout HIPEC perfusion, neither significant nor consistent changes in renal perfusion could be observed. Postoperative AKI occurred in 6 of 10 participating patients. Intraoperative renal resistive index (RRI) values > 0.8 were observed in one patient developing stage 3 AKI according KDIGO criteria. At 30 min in perfusion, RRI values were significantly higher in AKI + patients.
Conclusion: AKI is a common and frequent complication after HIPEC, but underlying pathophysiology remains elusive. High intraoperative RRI values may indicate an increased risk of postoperative AKI. Present data challenges the relevance of hyperthermia-derived hypothesis of renal hypoperfusion with prerenal injury during HIPEC. More attention should be drawn towards chemotoxic-induced hypothesis of HIPEC-induced AKI and caution applying regimens containing nephrotoxic agents in patients. Further confirmatory and complementary studies on renal perfusion as well as pharmacokinetic HIPEC studies are required.
Keywords: Acute kidney injury; Doppler ultrasound; HIPEC; Renal perfusion; Renal resistive index.
© 2023. The Author(s).
Conflict of interest statement
L. F. L. and A. B. report neither any disclosure nor any financial support.
Figures

Similar articles
-
HIPEC-Induced Acute Kidney Injury: A Retrospective Clinical Study and Preclinical Model.Ann Surg Oncol. 2022 Jan;29(1):139-151. doi: 10.1245/s10434-021-10376-5. Epub 2021 Jul 14. Ann Surg Oncol. 2022. PMID: 34260006 Free PMC article.
-
Extensive Peritonectomy is an Independent Risk Factor for Cisplatin HIPEC-Induced Acute Kidney Injury.Ann Surg Oncol. 2023 May;30(5):2646-2656. doi: 10.1245/s10434-022-12661-3. Epub 2022 Dec 10. Ann Surg Oncol. 2023. PMID: 36496489 Free PMC article.
-
Incidence, risk factors, and outcomes of the transition of HIPEC-induced acute kidney injury to acute kidney disease: a retrospective study.Ren Fail. 2024 Dec;46(1):2338482. doi: 10.1080/0886022X.2024.2338482. Epub 2024 Apr 11. Ren Fail. 2024. PMID: 38604946 Free PMC article.
-
A guide to establishing a hyperthermic intraperitoneal chemotherapy program in gynecologic oncology.Gynecol Oncol. 2020 Sep;158(3):794-802. doi: 10.1016/j.ygyno.2020.06.487. Epub 2020 Jul 2. Gynecol Oncol. 2020. PMID: 32624234 Review.
-
Surgical and oncologic outcomes of hyperthermic intraperitoneal chemotherapy for uterine leiomyosarcoma: A systematic review of literature.Gynecol Oncol. 2021 Apr;161(1):70-77. doi: 10.1016/j.ygyno.2020.12.032. Epub 2021 Jan 6. Gynecol Oncol. 2021. PMID: 33419612
Cited by
-
Nephrotoxicity Associated with Cytoreductive Surgery Combined with Cisplatin-Based Hyperthermic Intraperitoneal Chemotherapy for Peritoneal Malignant Disease: A Systematic Review and Meta-Analysis.J Clin Med. 2024 Jun 28;13(13):3793. doi: 10.3390/jcm13133793. J Clin Med. 2024. PMID: 38999359 Free PMC article. Review.
-
Side-Effects on the Renal function of Cytoreductive Surgery with Hyperthermic Intraperitoneal Chemotherapy.Int J Med Sci. 2024 Sep 30;21(13):2537-2543. doi: 10.7150/ijms.97774. eCollection 2024. Int J Med Sci. 2024. PMID: 39439460 Free PMC article.
References
MeSH terms
LinkOut - more resources
Full Text Sources

