Patient Positioning in Spine Surgery: What Spine Surgeons Should Know?
- PMID: 37226380
- PMCID: PMC10460667
- DOI: 10.31616/asj.2022.0320
Patient Positioning in Spine Surgery: What Spine Surgeons Should Know?
Abstract
Spine surgery has advanced tremendously over the last decade. The number of spine surgeries performed each year has also been increasing constantly. Unfortunately, the reporting of position-related complications in spine surgery has also been steadily increasing. These complications not only result in significant morbidity for the patient but also raises the risk of litigation for the surgical and anesthetic teams. Fortunately, most position-related complications are avoidable with basic positioning knowledge. Hence, it is critical to be cautious and take all necessary precautions to avoid position-related complications. We discuss the various position-related complications associated with the prone position, which is the most commonly used position in spine surgery, in this narrative review. We also discuss the various methods for avoiding complications. Furthermore, we briefly discuss less commonly used positions in spine surgery, like the lateral and sitting positions.
Keywords: Complications; Lateral position; Prone position; Safe spine surgery; Sitting position.
Conflict of interest statement
No potential conflict of interest relevant to this article was reported.
Figures
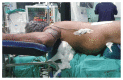

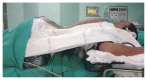
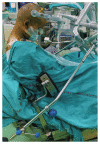
Comment in
-
Letter to the Editor: Patient Positioning in Spine Surgery: What Spine Surgeons Should Know?Asian Spine J. 2023 Dec;17(6):1176-1177. doi: 10.31616/asj.2023.0353.r1. Epub 2023 Dec 21. Asian Spine J. 2023. PMID: 38171027 Free PMC article. No abstract available.
-
Response to Letter to the Editor: Patient Positioning in Spine Surgery: What Spine Surgeons Should Know?Asian Spine J. 2023 Dec;17(6):1178-1179. doi: 10.31616/asj.2023.0353.r2. Epub 2023 Dec 21. Asian Spine J. 2023. PMID: 38171028 Free PMC article. No abstract available.
Similar articles
-
Outcomes in single-level posterior cervical spine surgeries performed in the sitting and prone positions.J Neurosurg Spine. 2020 Jul 3;33(5):667-673. doi: 10.3171/2020.4.SPINE191323. Print 2020 Nov 1. J Neurosurg Spine. 2020. PMID: 32619981
-
The ideal patient positioning in spine surgery: a preventive strategy.EFORT Open Rev. 2023 Feb 21;8(2):63-72. doi: 10.1530/EOR-22-0135. EFORT Open Rev. 2023. PMID: 36805330 Free PMC article. Review.
-
Positioning patients for spine surgery: Avoiding uncommon position-related complications.World J Orthop. 2014 Sep 18;5(4):425-43. doi: 10.5312/wjo.v5.i4.425. eCollection 2014 Sep 18. World J Orthop. 2014. PMID: 25232519 Free PMC article. Review.
-
Complications associated with prone positioning in elective spinal surgery.World J Orthop. 2015 Apr 18;6(3):351-9. doi: 10.5312/wjo.v6.i3.351. eCollection 2015 Apr 18. World J Orthop. 2015. PMID: 25893178 Free PMC article. Review.
-
Modified prone position using lateral brace attachments for cervico-dorsal spine surgeries.Eur Spine J. 2013 Jul;22(7):1474-9. doi: 10.1007/s00586-012-2653-9. Epub 2013 Jan 13. Eur Spine J. 2013. PMID: 23314870 Free PMC article.
Cited by
-
Response to Letter to the Editor: Patient Positioning in Spine Surgery: What Spine Surgeons Should Know?Asian Spine J. 2023 Dec;17(6):1178-1179. doi: 10.31616/asj.2023.0353.r2. Epub 2023 Dec 21. Asian Spine J. 2023. PMID: 38171028 Free PMC article. No abstract available.
-
Transient postoperative femoral neuropathy following prone positioning for posterior spine surgery: illustrative case.J Neurosurg Case Lessons. 2025 Jul 14;10(2):CASE25239. doi: 10.3171/CASE25239. Print 2025 Jul 14. J Neurosurg Case Lessons. 2025. PMID: 40658987 Free PMC article.
-
Efficacy and Safety of Dexmedetomidine in the Prone Position in Elderly Patients with Pneumonia: A Prospective, Double-Blind, Randomized Controlled Study.Lung. 2024 Oct;202(5):553-560. doi: 10.1007/s00408-024-00735-w. Epub 2024 Aug 7. Lung. 2024. PMID: 39107529 Clinical Trial.
-
Letter to the Editor: Patient Positioning in Spine Surgery: What Spine Surgeons Should Know?Asian Spine J. 2023 Dec;17(6):1176-1177. doi: 10.31616/asj.2023.0353.r1. Epub 2023 Dec 21. Asian Spine J. 2023. PMID: 38171027 Free PMC article. No abstract available.
References
-
- Deyo RA, Gray DT, Kreuter W, Mirza S, Martin BI. United States trends in lumbar fusion surgery for degenerative conditions. Spine (Phila Pa 1976) 2005;30:1441–7. - PubMed
-
- Oglesby M, Fineberg SJ, Patel AA, Pelton MA, Singh K. Epidemiological trends in cervical spine surgery for degenerative diseases between 2002 and 2009. Spine (Phila Pa 1976) 2013;38:1226–32. - PubMed
-
- Kutteruf R, Wells D, Stephens L, Posner KL, Lee LA, Domino KB. Injury and liability associated with spine surgery. J Neurosurg Anesthesiol. 2018;30:156–62. - PubMed
-
- Du A, Saba R, Brovman EY, Greenberg P, Urman RD. A contemporary medicolegal analysis of perioperative vision loss from 2007 to 2016. J Healthc Risk Manag. 2020;39:20–7. - PubMed
-
- De la Garza-Ramos R, Samdani AF, Sponseller PD, et al. Visual loss after corrective surgery for pediatric scoliosis: incidence and risk factors from a nationwide database. Spine J. 2016;16:516–22. - PubMed
LinkOut - more resources
Full Text Sources

