Left Ventricular Systolic Dysfunction in Patients Diagnosed With Hypertrophic Cardiomyopathy During Childhood: Insights From the SHaRe Registry
- PMID: 37226762
- PMCID: PMC10373850
- DOI: 10.1161/CIRCULATIONAHA.122.062517
Left Ventricular Systolic Dysfunction in Patients Diagnosed With Hypertrophic Cardiomyopathy During Childhood: Insights From the SHaRe Registry
Abstract
Background: The development of left ventricular systolic dysfunction (LVSD) in hypertrophic cardiomyopathy (HCM) is rare but serious and associated with poor outcomes in adults. Little is known about the prevalence, predictors, and prognosis of LVSD in patients diagnosed with HCM as children.
Methods: Data from patients with HCM in the international, multicenter SHaRe (Sarcomeric Human Cardiomyopathy Registry) were analyzed. LVSD was defined as left ventricular ejection fraction <50% on echocardiographic reports. Prognosis was assessed by a composite of death, cardiac transplantation, and left ventricular assist device implantation. Predictors of developing incident LVSD and subsequent prognosis with LVSD were assessed using Cox proportional hazards models.
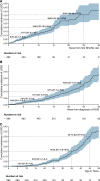
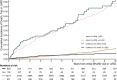
Results: We studied 1010 patients diagnosed with HCM during childhood (<18 years of age) and compared them with 6741 patients with HCM diagnosed as adults. In the pediatric HCM cohort, median age at HCM diagnosis was 12.7 years (interquartile range, 8.0-15.3), and 393 (36%) patients were female. At initial SHaRe site evaluation, 56 (5.5%) patients with childhood-diagnosed HCM had prevalent LVSD, and 92 (9.1%) developed incident LVSD during a median follow-up of 5.5 years. Overall LVSD prevalence was 14.7% compared with 8.7% in patients with adult-diagnosed HCM. Median age at incident LVSD was 32.6 years (interquartile range, 21.3-41.6) for the pediatric cohort and 57.2 years (interquartile range, 47.3-66.5) for the adult cohort. Predictors of developing incident LVSD in childhood-diagnosed HCM included age <12 years at HCM diagnosis (hazard ratio [HR], 1.72 [CI, 1.13-2.62), male sex (HR, 3.1 [CI, 1.88-5.2), carrying a pathogenic sarcomere variant (HR, 2.19 [CI, 1.08-4.4]), previous septal reduction therapy (HR, 2.34 [CI, 1.42-3.9]), and lower initial left ventricular ejection fraction (HR, 1.53 [CI, 1.38-1.69] per 5% decrease). Forty percent of patients with LVSD and HCM diagnosed during childhood met the composite outcome, with higher rates in female participants (HR, 2.60 [CI, 1.41-4.78]) and patients with a left ventricular ejection fraction <35% (HR, 3.76 [2.16-6.52]).
Conclusions: Patients with childhood-diagnosed HCM have a significantly higher lifetime risk of developing LVSD, and LVSD emerges earlier than for patients with adult-diagnosed HCM. Regardless of age at diagnosis with HCM or LVSD, the prognosis with LVSD is poor, warranting careful surveillance for LVSD, especially as children with HCM transition to adult care.
Keywords: cardiomyopathies; cardiomyopathy, hypertrophic; genetics; heart failure; ventricular dysfunction.
Conflict of interest statement
Figures



References
-
- Ommen SR, Mital S, Burke MA, Day SM, Deswal A, Elliott P, Evanovich LL, Hung J, Joglar JA, Kantor P, et al. . 2020 AHA/ACC guideline for the diagnosis and treatment of patients with hypertrophic cardiomyopathy: executive summary: a report of the American College of Cardiology/American Heart Association Joint Committee on Clinical Practice Guidelines. Circulation. 2020;142:e533–e557. doi: 10.1161/CIR.0000000000000938 - PubMed
-
- Elliott PM, Anastasakis A, Borger MA, Borggrefe M, Cecchi F, Charron P, Hagege AA, Lafont A, Limongelli G, Mahrholdt H, et al. ; Authors/Task Force members. 2014 ESC guidelines on diagnosis and management of hypertrophic cardiomyopathy: the Task Force for the Diagnosis and Management of Hypertrophic Cardiomyopathy of the European Society of Cardiology (ESC). Eur Heart J. 2014;35:2733–2779. doi: 10.1093/eurheartj/ehu284 - PubMed
-
- Geske JB, Gersh BJ. The hypertrophic cardiomyopathy paradox: better with age. Eur Heart J. 2019;40:994–996. doi: 10.1093/eurheartj/ehy889 - PubMed
-
- Lipshultz SE, Sleeper LA, Towbin JA, Lowe AM, Orav EJ, Cox GF, Lurie PR, McCoy KL, McDonald MA, Messere JE, et al. . The incidence of pediatric cardiomyopathy in two regions of the United States. N Engl J Med. 2003;348:1647–1655. doi: 10.1056/NEJMoa021715 - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Miscellaneous

