Surgical Management of Retroperitoneal Sarcoma
- PMID: 37232807
- PMCID: PMC10217420
- DOI: 10.3390/curroncol30050349
Surgical Management of Retroperitoneal Sarcoma
Abstract
Surgery is the cornerstone of treatment for retroperitoneal sarcoma (RPS). Surgery should be performed by a surgical oncologist with sub-specialization in this disease and in the context of a multidisciplinary team of sarcoma specialists. For primary RPS, the goal of surgery is to achieve the complete en bloc resection of the tumor along with involved organs and structures to maximize the clearance of the disease. The extent of resection also needs to consider the risk of complications. Unfortunately, the overarching challenge in primary RPS treatment is that even with optimal surgery, tumor recurrence occurs frequently. The pattern of recurrence after surgery (e.g., local versus distant) is strongly associated with the specific histologic type of RPS. Radiation and systemic therapy may improve outcomes in RPS and there is emerging data studying the benefit of non-surgical treatments in primary disease. Topics in need of further investigation include criteria for unresectability and management of locally recurrent disease. Moving forward, global collaboration among RPS specialists will be key for continuing to advance our understanding of this disease and find more effective treatments.
Keywords: collaboration; leiomyosarcoma; liposarcoma; multidisciplinary; retroperitoneal sarcoma.
Conflict of interest statement
The authors declare no conflict of interest.
Figures
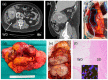
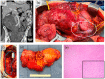
References
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Research Materials

