The Potential Role of Adjuvant Chemoradiotherapy in Patients with Microscopically Positive (R1) Surgical Margins after Resection of Cholangiocarcinoma
- PMID: 37232816
- PMCID: PMC10217181
- DOI: 10.3390/curroncol30050358
The Potential Role of Adjuvant Chemoradiotherapy in Patients with Microscopically Positive (R1) Surgical Margins after Resection of Cholangiocarcinoma
Abstract
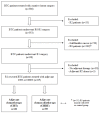
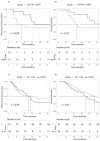
(1) Background: Biliary tract cancers (BTCs) are a heterogeneous group of neoplasms with dismal prognosis and the role of adjuvant chemoradiotherapy in high-risk resected patients is unclear. (2) Methods: We retrospectively analyzed the outcomes of BTC patients who received curative intent surgery with microscopically positive resection margins (R1) and adjuvant chemoradioradiotherapy (CCRT) or chemotherapy (CHT) from January 2001 to December 201. (3) Results: Out of 65 patients who underwent R1 resection, 26 received adjuvant CHT and 39 adjuvant CCRT. The median recurrence-free survival (RFS) in the CHT and CHRT groups was 13.2 and 26.8 months, respectively (p = 0.41). Median overall survival (OS) was higher in the CHRT group (41.9 months) as compared to the CHT group (32.2 months), but the difference was not statistically significant (HR 0.88; p = 0.7). A promising trend in favor of CHRT was observed in N0 patients. Finally, no statistically significant differences were observed between patients undergoing adjuvant CHRT after R1 resection and patients treated with chemotherapy alone after R0 surgery. (4) Conclusions: Our study did not show a significant survival benefit with adjuvant CHRT over CHT alone in BTC patients with positive resection margins, while a promising trend was observed.
Keywords: R1 surgery; biliary tract cancers; chemo-radiotherapy; cholangiocarcinoma; radiotherapy.
Conflict of interest statement
The authors declare no conflict of interest.
Figures

Similar articles
-
Adjuvant concurrent chemoradiation therapy in patients with microscopic residual tumor after curative resection for extrahepatic cholangiocarcinoma.Clin Transl Oncol. 2018 Aug;20(8):1011-1017. doi: 10.1007/s12094-017-1815-y. Epub 2017 Dec 18. Clin Transl Oncol. 2018. PMID: 29256155
-
Effect of Margin Status on Survival After Resection of Hilar Cholangiocarcinoma in the Modern Era of Adjuvant Therapies.Am Surg. 2021 Sep;87(9):1496-1503. doi: 10.1177/0003134820973401. Epub 2020 Dec 21. Am Surg. 2021. PMID: 33345594
-
Role of adjuvant (chemo)radiotherapy for resected extrahepatic cholangiocarcinoma: a meta-analysis.J Zhejiang Univ Sci B. 2020 Jul;21(7):549-559. doi: 10.1631/jzus.B1900691. J Zhejiang Univ Sci B. 2020. PMID: 32633109 Free PMC article.
-
The role of adjuvant chemotherapy and radiotherapy for cholangiocarcinoma.Best Pract Res Clin Gastroenterol. 2015 Apr;29(2):333-43. doi: 10.1016/j.bpg.2015.03.001. Epub 2015 Mar 16. Best Pract Res Clin Gastroenterol. 2015. PMID: 25966432 Review.
-
Systemic adjuvant chemotherapy for cholangiocarcinoma surgery: A systematic review and meta-analysis.Eur J Surg Oncol. 2020 Apr;46(4 Pt A):684-693. doi: 10.1016/j.ejso.2019.11.499. Epub 2019 Nov 15. Eur J Surg Oncol. 2020. PMID: 31761507
Cited by
-
Treatment Sequencing and Independent Outcomes of First- and Second-Line Chemotherapy in a Retrospective Series of Patients with Biliary Tract Cancer.J Clin Med. 2024 Nov 29;13(23):7262. doi: 10.3390/jcm13237262. J Clin Med. 2024. PMID: 39685721 Free PMC article.
References
-
- Jarnagin W.R., Ruo L., Little S.A., Klimstra D., D’Angelica M., DeMatteo R.P., Wagman R., Blumgart L.H., Fong Y. Patterns of Initial Disease Recurrence after Resection of Gallbladder Carcinoma and Hilar Cholangiocarcinoma: Implications for Adjuvant Therapeutic Strategies. Cancer. 2003;98:1689–1700. doi: 10.1002/cncr.11699. - DOI - PubMed
-
- Groot Koerkamp B., Wiggers J.K., Allen P.J., Besselink M.G., Blumgart L.H., Busch O.R.C., Coelen R.J., D’Angelica M.I., DeMatteo R.P., Gouma D.J., et al. Recurrence Rate and Pattern of Perihilar Cholangiocarcinoma after Curative Intent Resection. J. Am. Coll. Surg. 2015;221:1041–1049. doi: 10.1016/j.jamcollsurg.2015.09.005. - DOI - PMC - PubMed
-
- Spolverato G., Kim Y., Alexandrescu S., Marques H.P., Lamelas J., Aldrighetti L., Gamblin T.C., Maithel S.K., Pulitano C., Bauer T.W., et al. Management and Outcomes of Patients with Recurrent Intrahepatic Cholangiocarcinoma Following Previous Curative-Intent Surgical Resection. Ann. Surg. Oncol. 2016;23:235–243. doi: 10.1245/s10434-015-4642-9. - DOI - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

