Clinical Features and Treatment Progress of Invasive Mucormycosis in Patients with Hematological Malignancies
- PMID: 37233303
- PMCID: PMC10219352
- DOI: 10.3390/jof9050592
Clinical Features and Treatment Progress of Invasive Mucormycosis in Patients with Hematological Malignancies
Abstract
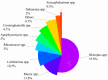
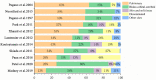
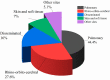
The incidence rate of invasive mucormycosis (IM) in patients with hematological malignancies (HMs) is increasing year by year, ranging from 0.07% to 4.29%, and the mortality rate is mostly higher than 50%. With the ongoing pandemic of COVID-19, COVID-19-associated mucormycosis (CAM) also became a global health threat. Patients with high risk factors such as active HMs, relapsed/refractory leukemia, prolonged neutropenia may still develop breakthrough mucormycosis (BT-MCR) even under the prophylaxis of Mucorales-active antifungals, and such patients often have higher mortality. Rhizopus spp. is the most common genus associated with IM, followed by Mucor spp. and Lichtheimia spp. Pulmonary mucormycosis (PM) is the most common form of IM in patients with HMs, followed by rhino-orbital-cerebral mucormycosis (ROCM) and disseminated mucormycosis. The prognosis of IM patients with neutrophil recovery, localized IM and receiving early combined medical-surgical therapy is usually better. As for management of the disease, risk factors should be eliminated firstly. Liposome amphotericin B (L-AmB) combined with surgery is the initial treatment scheme of IM. Those who are intolerant to L-AmB can choose intravenous formulations or tablets of isavuconazole or posaconazole. Patients who are refractory to monotherapy can turn to combined antifungals therapy.
Keywords: clinical manifestations; hematological malignancies; high risk factors; invasive mucormycosis; treatment.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures
References
-
- Valentine J.C., Morrissey C.O., Tacey M.A., Liew D., Patil S., Ananda-Rajah M. A population-based analysis of attributable hospitalisation costs of invasive fungal diseases in haematological malignancy patients using data linkage of state-wide registry and costing databases: 2009–2015. Mycoses. 2020;63:162–171. doi: 10.1111/myc.13033. - DOI - PubMed
-
- Pagano L., Ricci P., Tonso A., Nosari A., Cudillo L., Montillo M., Cenacchi A., Pacilli L., Fabbiano F., Del Favero A. Mucormycosis in patients with haematological malignancies: A retrospective clinical study of 37 cases. GIMEMA Infection Program (Gruppo Italiano Malattie Ematologiche Maligne dell’Adulto) Br. J. Haematol. 1997;99:331–336. doi: 10.1046/j.1365-2141.1997.3983214.x. - DOI - PubMed
-
- Lewis R.E., Cahyame-Zuniga L., Leventakos K., Chamilos G., Ben-Ami R., Tamboli P., Tarrand J., Bodey G.P., Luna M., Kontoyiannis D.P. Epidemiology and sites of involvement of invasive fungal infections in patients with haematological malignancies: A 20-year autopsy study. Mycoses. 2013;56:638–645. doi: 10.1111/myc.12081. - DOI - PubMed
Publication types
Grants and funding
LinkOut - more resources
Full Text Sources
Miscellaneous