Agitation and aggression in people living with dementia and mild cognitive impairment in shared-housing arrangements - validation of a German version of the Cohen-Mansfield Agitation Inventory-Short Form (CMAI-SF)
- PMID: 37248478
- PMCID: PMC10226019
- DOI: 10.1186/s12955-023-02132-y
Agitation and aggression in people living with dementia and mild cognitive impairment in shared-housing arrangements - validation of a German version of the Cohen-Mansfield Agitation Inventory-Short Form (CMAI-SF)
Abstract
Background: The Cohen-Mansfield Agitation Inventory-Short Form (CMAI-SF) is a 14-item scale for assessing agitation and aggression, derived from the original 29-item CMAI, and completed by a proxy. Because the CMAI-SF has not yet been validated in German language, the aim of this study is to explore its construct validity.
Methods: Baseline data from a cluster-randomized trial to evaluate a non-pharmacological complex intervention for people living with dementia (PlwD) and mild cognitive impairment (MCI) were analyzed. The study sample consisted of 97 shared-housing arrangements (SHAs) in Germany, comprising N = 341 residents with mild to severe dementia and MCI. Trained nursing staff collected data by proxy-rating the CMAI-SF, Neuropsychiatric Inventory-Nursing Home Version (NPI-NH), and QUALIDEM. They also conducted the Mini-Mental State Examination (MMSE) and the Montreal Cognitive Assessment (MoCA).
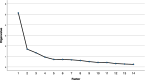
Results: In an exploratory factor analysis, three factors emerged: "aggressive behavior", "verbally agitated behavior", and "physically non-aggressive behavior". The CMAI-SF total score showed good internal consistency (α = .85), and the factors themselves showed adequate internal consistency (α = .75/.76/.73). The CMAI-SF showed convergent validity with the NPI-NH agitation item (r = .66) and the NPI-NH "agitation & restless behavior" factor (r = .82). Discriminant validity was confirmed by a low (r = .28) correlation with the NPI-NH apathy item. Quality of life decreased significantly with agitation, as the CMAI-SF showed a moderate negative correlation with the QUALIDEM total score (r = -.35).
Conclusions: The 14-item CMAI-SF is a time-efficient, reliable, and valid assessment instrument. Three factors emerged that were similar to those already found in nursing home samples for the original CMAI and the CMAI-SF and in day care samples for the CMAI-SF. The findings provide preliminary evidence that the CMAI-SF can be used instead of the CMAI to reduce time, costs, and burden in future trials.
Trial registration: The DemWG study from which data were used to draft this manuscript was prospectively registered on 16 July 2019 at ISRCTN registry (ISRCTN89825211).
Keywords: Aggression; Agitation; CMAI; CMAI-SF; Cohen-Mansfield Agitation Inventory; Dementia; Mild cognitive impairment; Reliability; Shared-housing arrangements; Validity.
© 2023. The Author(s).
Conflict of interest statement
The authors declare no competing interests.
Figures

References
-
- Livingston G, Barber J, Marston L, Rapaport P, Livingston D, Cousins S, Robertson S, La Frenais F, Cooper C. Prevalence of and associations with agitation in residents with dementia living in care homes: MARQUE cross-sectional study. BJPsych Open. 10.1192/bjpo.bp.117.0051812017;3:171–8. - DOI - PMC - PubMed
-
- Cloak N, Al Khalili Y. Behavioral And Psychological Symptoms In Dementia. Treasure Island (FL): StatPearls Publishing; 2021. - PubMed
-
- Baharudin AD, Din NC, Subramaniam P, Razali R. The associations between behavioral-psychological symptoms of dementia (BPSD) and coping strategy, burden of care and personality style among low-income caregivers of patients with dementia. BMC Public Health. 2019;19:447. doi: 10.1186/s12889-019-6868-0. - DOI - PMC - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

