The Responsiveness of Three Persian Outcome Measures Following Physiotherapy Intervention in Patients with Chronic Non-Specific Neck Pain
- PMID: 37265526
- PMCID: PMC10231919
- DOI: 10.22038/ABJS.2023.68253.3227
The Responsiveness of Three Persian Outcome Measures Following Physiotherapy Intervention in Patients with Chronic Non-Specific Neck Pain
Abstract
Objectives: A prospective cohort study to evaluate and compare the responsiveness of the Persian version of the neck disability index (NDI), neck pain & disability scale (NPDS), neck outcome score (NOOS), and to determine the minimal clinically important difference (MCID) and minimal detectable change (MDC). To date, no studies have made a direct comparison between the responsiveness of the Persian version of NPDS, NDI, and NOOS questionnaires.
Methods: At the end of the study, 55 patients with chronic non-specific neck pain completed the NPDS, NDI, and NOOS questionnaires at the beginning and end of three weeks of physiotherapy treatment. Additionally, patients completed the global rating of change scale to differentiate between improved and unimproved patients. Comparison of responsiveness was performed using anchor-based methods (receiver operating characteristic (ROC) curve and correlation analysis). MCID and MDC were assessed to investigate relevant changes for each questionnaire.
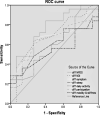
Results: ROC curves analysis showed areas under the curves of 0.70, 0.64, and 0.43 to 0.63 for the NPDS, NDI, and NOOS subscales, respectively. The correlation coefficients between the global rating of the change scale and the change scores of the NPDS and NDI were 0.38 (P<0.01) and 0.30 (P<0.05), respectively. There were no significant correlations between NOOS subscales and global rating of change score (r=0.001- 0.21, P>0.05). The MCID for the NPDS, NDI, and NOOS subscales were 28.09 (score 0-100), 7.5 (score 0-50), and 13.75 to 28.64 (score 0-100), respectively. The MDCs were found to be in the following order: 47.1 points for NPDS, 36.1 for NDI, and 23.5 to 39.7 for NOOS subscales.
Conclusion: The Persian NPDS seems more responsive than the NDI and NOOS questionnaires. The level of clinically meaningful change in NDI, NPDS, and NOOS questionnaires is in the range of measurement error.
Keywords: Disability; Minimal clinically important difference; Neck disability questionnaires; Neck pain; ROC curve.
Conflict of interest statement
The authors do NOT have any potential conflicts of interest for this manuscript.
Figures
Similar articles
-
Translation, Cross-Cultural Adaptation, Reliability, and Validity of the Persian Version of the Neck Outcome Score Questionnaire in Iranian Patients With Nonspecific Neck Pain.J Chiropr Med. 2024 Sep;23(3):127-135. doi: 10.1016/j.jcm.2024.08.004. Epub 2024 Oct 29. J Chiropr Med. 2024. PMID: 39670201 Free PMC article.
-
Responsiveness and Interpretability of the Portuguese Version of the Neck Disability Index in Patients With Chronic Neck Pain Undergoing Physiotherapy.Spine (Phila Pa 1976). 2015 Nov;40(22):E1180-6. doi: 10.1097/BRS.0000000000001034. Spine (Phila Pa 1976). 2015. PMID: 26110663
-
Responsiveness and minimal important changes for the Neck Disability Index and the Neck Pain Disability Scale in Italian subjects with chronic neck pain.Eur Spine J. 2015 Dec;24(12):2821-7. doi: 10.1007/s00586-015-3785-5. Epub 2015 Feb 7. Eur Spine J. 2015. PMID: 25663644
-
Psychometric properties of the Neck OutcOme Score, Neck Disability Index, and Short Form-36 were evaluated in patients with neck pain.J Clin Epidemiol. 2016 Nov;79:31-40. doi: 10.1016/j.jclinepi.2016.03.015. Epub 2016 Mar 31. J Clin Epidemiol. 2016. PMID: 27038852
-
Patient-Reported Outcome Measures Used for Neck Disorders: An Overview of Systematic Reviews.J Orthop Sports Phys Ther. 2018 Oct;48(10):775-788. doi: 10.2519/jospt.2018.8131. Epub 2018 Jun 22. J Orthop Sports Phys Ther. 2018. PMID: 29932874
Cited by
-
Investigating the Effect of Addition of Cervical Proprioceptive Training to Conventional Physiotherapy on Visual, Vestibular and Proprioceptive Dependency of Postural Control in Patients with Chronic Non-Specific Neck Pain: A Randomized Controlled Clinical Trial.Arch Bone Jt Surg. 2024;12(1):36-50. doi: 10.22038/ABJS.2023.74763.3462. Arch Bone Jt Surg. 2024. PMID: 38318308 Free PMC article.
-
Translation, Cross-Cultural Adaptation, Reliability, and Validity of the Persian Version of the Neck Outcome Score Questionnaire in Iranian Patients With Nonspecific Neck Pain.J Chiropr Med. 2024 Sep;23(3):127-135. doi: 10.1016/j.jcm.2024.08.004. Epub 2024 Oct 29. J Chiropr Med. 2024. PMID: 39670201 Free PMC article.
References
-
- Huisstede BM, Wijnhoven HA, Bierma-Zeinstra SM, Koes BW, Verhaar JA, Picavet S. Prevalence and characteristics of complaints of the arm, neck, and/or shoulder (CANS) in the open population. Clin J Pain. 2008;24(3):253–259. - PubMed
-
- Ferrari R, Russell AS. Regional musculoskeletal conditions: neck pain. Best Pract Res Clin Rheumatol. 2003;17(1):57–70. - PubMed
-
- Mousavi SJ, Parnianpour M, Montazeri A, et al. Translation and validation study of the Iranian versions of the Neck Disability Index and the Neck Pain and Disability Scale. Spine (Phila Pa 1976). 2007;32(26):E825–831. - PubMed
-
- Deyo R. Measuring the functional status of patients with low back pain. Arch Phys Med Rehabil. 1988;69(12):1044–1053. - PubMed
-
- Deyo RA, Battie M, Beurskens AJ, et al. Outcome measures for low back pain research A proposal for standardized use. Spine (Phila Pa 1976). 1998;23(18):2003–2013. - PubMed
LinkOut - more resources
Full Text Sources