Spinal Dural Arteriovenous Fistula: Insights Into Operative Management
- PMID: 37273323
- PMCID: PMC10234455
- DOI: 10.7759/cureus.38448
Spinal Dural Arteriovenous Fistula: Insights Into Operative Management
Abstract
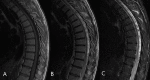
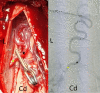
Spinal Dural Arteriovenous Fistula (SDAVF) is a rare and complex vascular condition with significant neurological consequences if left untreated. We present a case of SDAVF in a 46-year-old male who presented with progressive myelopathy. The patient presented with a three-month history of progressive lower extremity weakness, numbness, urinary retention, constipation, and gait disturbance. The spine's magnetic resonance imaging (MRI) showed diffuse T2 hyperintensity and contrast enhancement from T11 to L1, raising the suspicion of an intradural spinal cord lesion. Further evaluation with spinal angiography revealed an SDAVF at the level of T11-T12. The patient underwent surgical resection of the fistula, His lower extremity weakness and numbness improved significantly after surgery, and he was discharged with a plan for close follow-up. Early diagnosis and appropriate treatment prevent neurological deficits and improve patient outcomes. Surgical resection of the fistula can significantly improve neurological symptoms and should be considered a treatment option for SDAVF.
Keywords: erectile dysfunction; sdavf; spinal venous congestion; urinary retention; weakness.
Copyright © 2023, Msheik et al.
Conflict of interest statement
The authors have declared that no competing interests exist.
Figures

References
-
- Altered expression of alpha3-containing GABAA receptors in the neocortex of patients with focal epilepsy. Loup F, Picard F, André VM, Kehrli P, Yonekawa Y, Wieser HG, Fritschy JM. Brain. 2006;129:3277–3289. - PubMed
-
- Embolization of spinal dural arteriovenous fistulas: importance of occlusion of the draining vein. Jellema K, Sluzewski M, van Rooij WJ, Rinkel GJ. J Neurosurg Spine. 2007;7:161–164. - PubMed
-
- Low risk of traumatic intracranial hematoma expansion with factor Xa inhibitors without andexanet reversal. Maragkos GA, Nelton EB, Richter S, Stippler M. World Neurosurg. 2020;142:0. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
