Omega-3 Fatty Acids in Arterial Hypertension: Is There Any Good News?
- PMID: 37298468
- PMCID: PMC10253816
- DOI: 10.3390/ijms24119520
Omega-3 Fatty Acids in Arterial Hypertension: Is There Any Good News?
Abstract
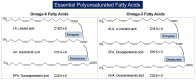
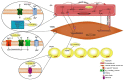
Omega-3 polyunsaturated fatty acids (ω-3 PUFAs), including alpha-linolenic acid (ALA) and its derivatives eicosapentaenoic acid (EPA) and docosahexaenoic acid (DHA), are "essential" fatty acids mainly obtained from diet sources comprising plant oils, marine blue fish, and commercially available fish oil supplements. Many epidemiological and retrospective studies suggested that ω-3 PUFA consumption decreases the risk of cardiovascular disease, but results of early intervention trials have not consistently confirmed this effect. In recent years, some large-scale randomized controlled trials have shed new light on the potential role of ω-3 PUFAs, particularly high-dose EPA-only formulations, in cardiovascular prevention, making them an attractive tool for the treatment of "residual" cardiovascular risk. ω-3 PUFAs' beneficial effects on cardiovascular outcomes go far beyond the reduction in triglyceride levels and are thought to be mediated by their broadly documented "pleiotropic" actions, most of which are directed to vascular protection. A considerable number of clinical studies and meta-analyses suggest the beneficial effects of ω-3 PUFAs in the regulation of blood pressure in hypertensive and normotensive subjects. These effects occur mostly through regulation of the vascular tone that could be mediated by both endothelium-dependent and independent mechanisms. In this narrative review, we summarize the results of both experimental and clinical studies that evaluated the effect of ω-3 PUFAs on blood pressure, highlighting the mechanisms of their action on the vascular system and their possible impact on hypertension, hypertension-related vascular damage, and, ultimately, cardiovascular outcomes.
Keywords: alpha-linoleic acid (ALA); arterial stiffness; docosahexaenoic acid (DHA); eicosapentaenoic acid (EPA); endothelial dysfunction; hypertension; linoleic acid (LA); omega-3 polyunsaturated fatty acids (ω-3 PUFAs); oxylipins; primary prevention; residual cardiovascular risk; secondary prevention.
Conflict of interest statement
The authors declare no conflict of interest.
Figures

References
-
- Williams B., Mancia G., Spiering W., Agabiti Rosei E., Azizi M., Burnier M., Clement D.L., Coca A., de Simone G., Dominiczak A., et al. 2018 ESC/ESH Guidelines for the management of arterial hypertension. Eur. Heart J. 2018;39:3021–3104. doi: 10.1093/eurheartj/ehy339. Erratum in: Eur. Heart J. 2019, 40, 475. - DOI - PubMed
-
- Whelton P.K., Carey R.M., Aronow W.S., Casey D.E.J., Collins K.J., Dennison Himmelfarb C., De Palma S.M., Gidding S., Jamerson K.A., Jones D.W., et al. 2017 ACC/AHA/AAPA/ABC/ACPM/AGS/APhA/ASH/ASPC/NMA/PCNA Guideline for the Prevention, Detection, Evaluation, and Management of High Blood Pressure in Adults: A Report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. Hypertension. 2018;71:e13–e115. doi: 10.1161/hyp.0000000000000076. Erratum in Hypertension 2018, 71, e140–e144. - DOI - PubMed
-
- World Health Organization (WHO) World Health Organization Obesity and Overweight Fact Sheet. World Health Organization; Geneva, Switzerland: 2016.
-
- Lim S.S., Vos T., Flaxman A.D., Danaei G., Shibuya K., Adair-Rohani H., Amann M., Anderson H.R., Andrews K.G., Aryee M., et al. A comparative risk assessment of burden of disease and injury attributable to 67 risk factors and risk factor clusters in 21 regions, 1990–2010: A systematic analysis for the Global Burden of Disease Study 2010. Lancet. 2012;380:2224–2260. doi: 10.1016/S0140-6736(12)61766-8. - DOI - PMC - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Research Materials

