Normal-weight visceral obesity promotes a higher 10-year atherosclerotic cardiovascular disease risk in patients with type 2 diabetes mellitus-a multicenter study in China
- PMID: 37308932
- PMCID: PMC10262529
- DOI: 10.1186/s12933-023-01876-7
Normal-weight visceral obesity promotes a higher 10-year atherosclerotic cardiovascular disease risk in patients with type 2 diabetes mellitus-a multicenter study in China
Abstract
Background: Visceral obesity is associated with high cardiovascular events risk in type 2 diabetes mellitus (T2DM). Whether normal-weight visceral obesity will pose a higher atherosclerotic cardiovascular disease (ASCVD) risk than body mass index (BMI)-defined overweight or obese counterparts with or without visceral obesity remains unclear. We aimed to explore the relationship between general obesity and visceral obesity and 10-year ASCVD risk in patients with T2DM.
Methods: Patients with T2DM (6997) who satisfied the requirements for inclusion were enrolled. Patients were considered to have normal weight when 18.5 kg/m2 ≤ BMI < 24 kg/m2; overweight when 24 kg/m2 ≤ BMI < 28 kg/m2; and obesity when BMI ≥ 28 kg/m2. Visceral obesity was defined as a visceral fat area (VFA) ≥ 100 cm2. Patients were separated into six groups based on BMI and VFA. The odd ratios (OR) for a high 10-year ASCVD risk for different combinations of BMI and VFA were analysed using stepwise logistic regression. Receiver operating characteristic (ROC) curves for diagnosing the high 10-year ASCVD risk were constructed, and areas under the ROC curves were estimated. Potential non-linear relationships between VFA levels and high 10-year ASCVD risk were examined using restricted cubic splines (knot = 4). Multilinear regression was used to identify factors affecting VFA in patients with T2DM.
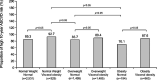
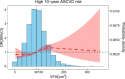
Results: In patients with T2DM, subjects with normal-weight visceral obesity had the highest 10-year ASCVD risk among the six groups, which had more than a 2-fold or 3-fold higher OR than those who were overweight or obese according to BMI but did not have visceral obesity (all P < 0.05). The VFA threshold for high 10-year ASCVD risk was 90 cm2. Multilinear regression showed significant differences in the effect of age, hypertension, drinking, fasting serum insulin, fasting plasma glucose, 2 h postprandial C-peptide, triglyceride, total cholesterol, high-density lipoprotein cholesterol, and low-density lipoprotein cholesterol on VFA in patients with T2DM (all P < 0.05).
Conclusions: T2DM patients with normal-weight visceral obesity had a higher 10-year ASCVD risk than BMI-defined overweight or obese counterparts with or without visceral obesity, which should initiate standardised management for ASCVD primary prevention.
Keywords: Atherosclerotic cardiovascular disease risk; Multicentre study; Normal weight; Obesity paradox; Type 2 diabetes mellitus; Visceral obesity.
© 2023. The Author(s).
Conflict of interest statement
The authors declare no competing interests.
Figures





Similar articles
-
Anthropometric and metabolic parameters associated with visceral fat in non-obese type 2 diabetes individuals.Diabetol Metab Syndr. 2025 Jan 22;17(1):28. doi: 10.1186/s13098-025-01583-1. Diabetol Metab Syndr. 2025. PMID: 39844248 Free PMC article.
-
Visceral adiposity and inflammatory bowel disease.Int J Colorectal Dis. 2021 Nov;36(11):2305-2319. doi: 10.1007/s00384-021-03968-w. Epub 2021 Jun 9. Int J Colorectal Dis. 2021. PMID: 34104989 Review.
-
Association of obesity with cardiovascular outcomes in patients with type 2 diabetes and cardiovascular disease: Insights from TECOS.Am Heart J. 2020 Jan;219:47-57. doi: 10.1016/j.ahj.2019.09.016. Epub 2019 Oct 20. Am Heart J. 2020. PMID: 31707324 Clinical Trial.
-
Visceral fat correlates with insulin secretion and sensitivity independent of BMI and subcutaneous fat in Chinese with type 2 diabetes.Front Endocrinol (Lausanne). 2023 Feb 27;14:1144834. doi: 10.3389/fendo.2023.1144834. eCollection 2023. Front Endocrinol (Lausanne). 2023. PMID: 36909323 Free PMC article.
-
The obesity paradox and diabetes.Eat Weight Disord. 2021 May;26(4):1057-1068. doi: 10.1007/s40519-020-01015-1. Epub 2020 Sep 20. Eat Weight Disord. 2021. PMID: 32954485 Review.
Cited by
-
Association of systemic immune-inflammation index with diabetic kidney disease in patients with type 2 diabetes: a cross-sectional study in Chinese population.Front Endocrinol (Lausanne). 2024 Jan 4;14:1307692. doi: 10.3389/fendo.2023.1307692. eCollection 2023. Front Endocrinol (Lausanne). 2024. PMID: 38239983 Free PMC article.
-
Dietary strategies and nutritional supplements in the management of heart failure: a systematic review.Front Nutr. 2024 Oct 11;11:1428010. doi: 10.3389/fnut.2024.1428010. eCollection 2024. Front Nutr. 2024. PMID: 39464682 Free PMC article.
-
Association of Body Mass Index with Outcomes in Patients with Heart Failure with Reduced Ejection Fraction (HFrEF).Nutrients. 2024 Jul 30;16(15):2473. doi: 10.3390/nu16152473. Nutrients. 2024. PMID: 39125352 Free PMC article.
-
Association between dynamic change patterns of body mass or fat mass and incident stroke: results from the China Health and Retirement Longitudinal Study (CHARLS).Front Cardiovasc Med. 2023 Nov 21;10:1269358. doi: 10.3389/fcvm.2023.1269358. eCollection 2023. Front Cardiovasc Med. 2023. PMID: 38075971 Free PMC article.
-
Combined impact of alcohol consumption and metabolic syndrome on liver dysfunction in an elderly Chinese population.Diabetol Metab Syndr. 2024 Mar 23;16(1):74. doi: 10.1186/s13098-024-01312-0. Diabetol Metab Syndr. 2024. PMID: 38519973 Free PMC article.
References
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical

