Chronic cerebral hypoperfusion: a critical feature in unravelling the etiology of vascular cognitive impairment
- PMID: 37309012
- PMCID: PMC10259064
- DOI: 10.1186/s40478-023-01590-1
Chronic cerebral hypoperfusion: a critical feature in unravelling the etiology of vascular cognitive impairment
Abstract
Vascular cognitive impairment (VCI) describes a wide spectrum of cognitive deficits related to cerebrovascular diseases. Although the loss of blood flow to cortical regions critically involved in cognitive processes must feature as the main driver of VCI, the underlying mechanisms and interactions with related disease processes remain to be fully elucidated. Recent clinical studies of cerebral blood flow measurements have supported the role of chronic cerebral hypoperfusion (CCH) as a major driver of the vascular pathology and clinical manifestations of VCI. Here we review the pathophysiological mechanisms as well as neuropathological changes of CCH. Potential interventional strategies for VCI are also reviewed. A deeper understanding of how CCH can lead to accumulation of VCI-associated pathology could potentially pave the way for early detection and development of disease-modifying therapies, thus allowing preventive interventions instead of symptomatic treatments.
Keywords: Chronic cerebral hypoperfusion; Neuronal cell death; Vascular dementia; White matter lesions.
© 2023. The Author(s).
Conflict of interest statement
The authors declare no competing interests.
Figures
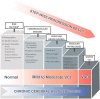
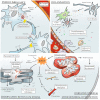
References
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources

