Circadian rhythm disturbance and delirium in ICU patients: a prospective cohort study
- PMID: 37312021
- PMCID: PMC10262569
- DOI: 10.1186/s12871-023-02163-4
Circadian rhythm disturbance and delirium in ICU patients: a prospective cohort study
Abstract
Background: Patients treated in the intensive care unit (ICU) may experience a reversal of day and night. The circadian rhythm in ICU patients can be disturbed.
Methods: To explore the relationship between ICU delirium and the circadian rhythms of melatonin, cortisol and sleep. A prospective cohort study was carried out in a surgical ICU of a tertiary teaching hospital. Patients who were conscious during the ICU stay after surgery and were scheduled to stay in the ICU for more than 24 h were enrolled. Serum melatonin and plasma cortisol levels were measured three times a day by drawing arterial blood on the first three days after ICU admission. Daily sleep quality was assessed by the Richard-Campbell Sleep Questionnaire (RCSQ). The Confusion Assessment Method for the Intensive Care Unit (CAM-ICU) was performed twice a day to screen for ICU delirium.
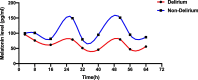
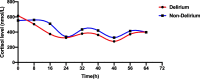
Results: A total of 76 patients were included in this study, and 17 patients developed delirium during their ICU stay. Melatonin levels were different at 8:00 (p = 0.048) on day 1, at 3:00 (p = 0.002) and at 8:00 (p = 0.009) on day 2, and at all three time points on day 3 (p = 0.032, 0.014, 0.047) between delirium and non-delirium patients. The plasma cortisol level in the delirium patients was significantly lower than that in the non-delirium patients at 16:00 on day 1 (p = 0.025). The changes in melatonin and cortisol secretion levels exhibited obvious biological rhythmicity in non-delirium patients (p < 0.001 for melatonin, p = 0.026 for cortisol), while no rhythmicity was found in melatonin and cortisol secretion levels in the delirium group (p = 0.064 for melatonin, p = 0.454 for cortisol). There was no significant difference in RCSQ scores in the first three days between the two groups.
Conclusions: The disturbance of the circadian rhythm of melatonin and cortisol secretion was associated with the development of delirium in ICU patients. Clinical staff should pay more attention to the importance of maintaining patients' normal circadian rhythms in the ICU.
Trial registration: The study was registered with the US National Institutes of Health ClinicalTrials.gov(NCT05342987) (25/04/2022).
Keywords: Circadian rhythm; Cortisol; Delirium; Melatonin.
© 2023. The Author(s).
Conflict of interest statement
The authors declare no competing interests.
Figures
Similar articles
-
Sleep and circadian rhythm disturbances in intensive care unit (ICU)-acquired delirium: a case-control study.J Int Med Res. 2021 Mar;49(3):300060521990502. doi: 10.1177/0300060521990502. J Int Med Res. 2021. PMID: 33730927 Free PMC article.
-
Effects of general versus subarachnoid anaesthesia on circadian melatonin rhythm and postoperative delirium in elderly patients undergoing hip fracture surgery: A prospective cohort clinical trial.EBioMedicine. 2021 Aug;70:103490. doi: 10.1016/j.ebiom.2021.103490. Epub 2021 Jul 17. EBioMedicine. 2021. PMID: 34280784 Free PMC article.
-
Impact of oral melatonin on critically ill adult patients with ICU sleep deprivation: study protocol for a randomized controlled trial.Trials. 2014 Aug 18;15:327. doi: 10.1186/1745-6215-15-327. Trials. 2014. PMID: 25135124 Free PMC article. Clinical Trial.
-
Disruption of Circadian Rhythms and Delirium, Sleep Impairment and Sepsis in Critically ill Patients. Potential Therapeutic Implications for Increased Light-Dark Contrast and Melatonin Therapy in an ICU Environment.Curr Pharm Des. 2015;21(24):3453-68. doi: 10.2174/1381612821666150706105602. Curr Pharm Des. 2015. PMID: 26144941 Review.
-
Potential use of melatonin in sleep and delirium in the critically ill.Br J Anaesth. 2012 Apr;108(4):572-80. doi: 10.1093/bja/aes035. Br J Anaesth. 2012. PMID: 22419624 Review.
Cited by
-
Potential Neuroprotective Role of Melatonin in Sepsis-Associated Encephalopathy Due to Its Scavenging and Anti-Oxidative Properties.Antioxidants (Basel). 2023 Sep 21;12(9):1786. doi: 10.3390/antiox12091786. Antioxidants (Basel). 2023. PMID: 37760089 Free PMC article. Review.
-
Circadian clock activity in human umbilical vein endothelial cells of preterm and term neonates.Pediatr Res. 2024 Dec 13. doi: 10.1038/s41390-024-03705-3. Online ahead of print. Pediatr Res. 2024. PMID: 39672824
-
Prospective cohort study on characteristics, associated factors and short-term prognosis of sleep and circadian rhythm in intensive care unit: protocol for the SYNC study.BMJ Open. 2025 Mar 4;15(3):e091184. doi: 10.1136/bmjopen-2024-091184. BMJ Open. 2025. PMID: 40037668 Free PMC article.
References
-
- Ely EW, et al. Evaluation of delirium in critically ill patients: validation of the Confusion Assessment Method for the Intensive Care Unit (CAM-ICU). Crit Care Med. 2001;29(7):1370–9. - PubMed
-
- Ely EW, et al. Delirium as a predictor of mortality in mechanically ventilated patients in the intensive care unit. JAMA. 2004;291(14):1753–62. - PubMed
Publication types
MeSH terms
Substances
Associated data
LinkOut - more resources
Full Text Sources
Medical

